
The Application of Image Guidance to Challenging Spinal Surgery Cases
Authors
Eric W. Nottmeier, MD*
Christopher P. Ames, MD**
Volker K. H. Sonntag, MD
Curtis A. Dickman, MD
Stephen M. Papadopoulos, MD
Division of Neurological Surgery, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
Current Addresses:
*Department of Neurosurgery, Mayo Clinic, Jacksonville, Florida
**Department of Neurosurgery, UCSF, San Francisco, California
Abstract
Image guidance serves as a useful adjunct to difficult spinal surgery cases because it allows spinal instrumentation to be inserted more accurately than traditional techniques. We present five challenging spinal surgery cases in which image guidance played a crucial role in obtaining a successful outcome.
Key Words: image guidance, spinal instrumentation
Introduced in 1991, image guidance for intracranial surgery has increased the safety and accuracy of cranial procedures.[1,2,6,9,10] Initially, the application of image guidance to the spine was challenging because registration was difficult due to the dynamic nature of the spine. However, these problems were overcome and by the mid1990s image-guided spinal surgery was becoming more widespread.[5,7] Subsequently, image guidance has been shown to improve the accuracy and safety of spinal procedures.[3,4,8,11,12] The StealthStation (Medtronic SNT, Louisville, CO) is the preferred image-guidance system for spinal surgery at our institution. This article highlights several unique and difficult spinal surgery cases in which image guidance played a crucial role.
Illustrative Cases
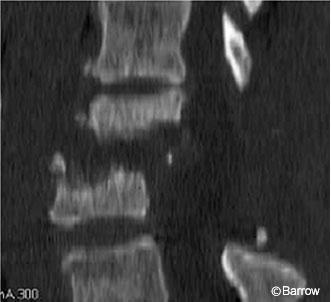
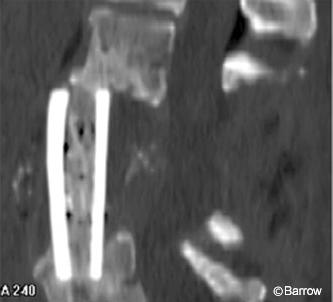
shows pistoning of the strut graft into the L5 vertebral body with anterior displacement
of the upper part of the graft.
Case 1
A neutropenic 69-year-old female, who had already undergone multiple posterior procedures to treat a recurrent lumbar epidural abscess, suffered from progressive destruction of the L3 and L4 vertebral bodies caused by osteomyelitis (Fig. 1). The patient underwent an L3-L4 corpectomy and placement of a tibial strut allograft. The course of the common iliac arteries anterolaterally over the L5 vertebral body prohibited placing instrumentation through this approach, and pedicle screw fixation was planned via a staged posterior procedure. Radiological studies obtained before her staged posterior procedure revealed pistoning of her graft into the L5 vertebral body with associated anterior displacement of its upper portion (Fig. 2).
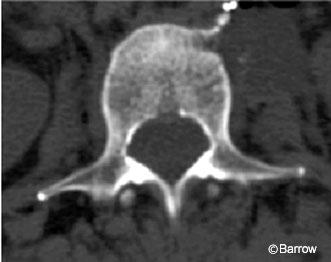
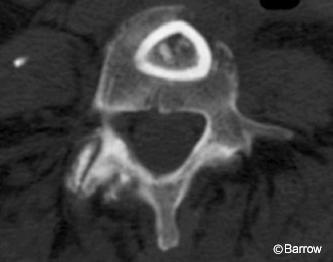
The patient underwent a posterior procedure for pedicle screw-rod fixation from L2 to L5 and possible adjustment of the displaced strut graft. Challenging aspects of the case included the small size of the L2 pedicles (Fig. 3) and the pistoning of the graft into the L5 body, which prohibited the L5 pedicle screws from being placed in the standard trajectory (Fig. 4). After registration at L2, image guidance was used to place the L2 pedicle screws successfully (Fig. 5). While registered at L2, dissection was continued down the remaining portion of the left L3 pedicle. A significant amount of scar tissue existed from her previous posterior procedures. The displaced strut graft could be visualized through a small anterior opening through this scar tissue, lateral to the dura.
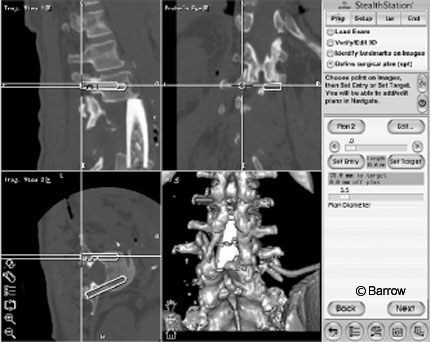
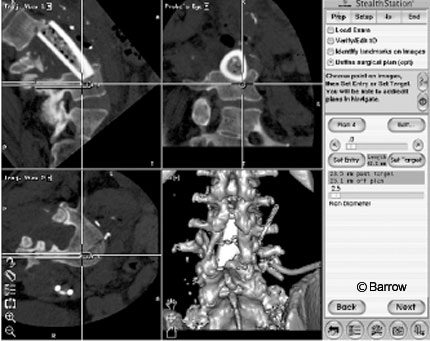
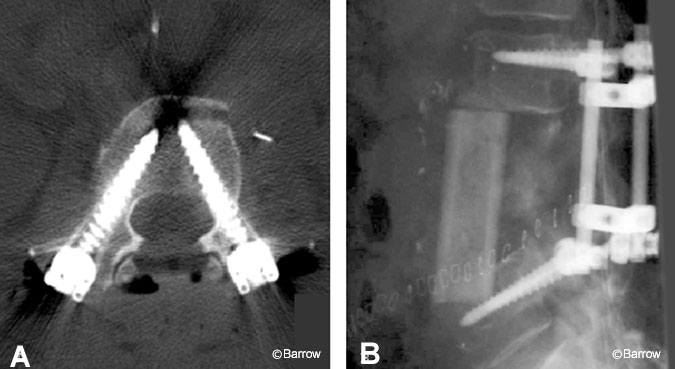
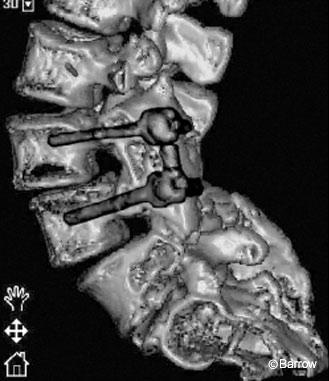
The plan was to adjust the graft by inserting a long-handled tap into it and using the tap to pull the graft posteriorly while applying distractive forces via the pedicle screws. A small hole was drilled unicortically through the posterior aspect of the graft. The optimal location for placement of this hole was ascertained using image guidance. A long-handled, 4.5-mm tap was inserted through this hole and left in place. Next, the L5 level was registered and the L5 pedicle screws were carefully placed using image guidance in a superior-to-inferior trajectory to avoid contact with the pistoned strut graft (Fig. 6). Distraction was accomplished with the instrumentation while simultaneously pulling the upper part of the graft posteriorly using the long-handled tap. Postoperative radiological studies revealed adequate placement of screws with improved positioning of the strut graft (Fig. 7).
Case 2
A 65-year-old female presented with recurrent lower back and buttock pain. About 3 years earlier, she had undergone L3-4 pedicle screw fixation with posterolateral fusion and subsequent removal of the right L3 and L4 pedicle screws after instrument failure. Radiological studies revealed a stable L3-4 fusion, but she was developing instability at L4-L5 (Fig. 8). The patient underwent an L5 laminectomy with pedicle screw fixation and posterolateral fusion at L4-5.
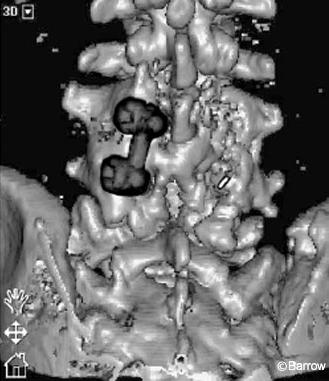
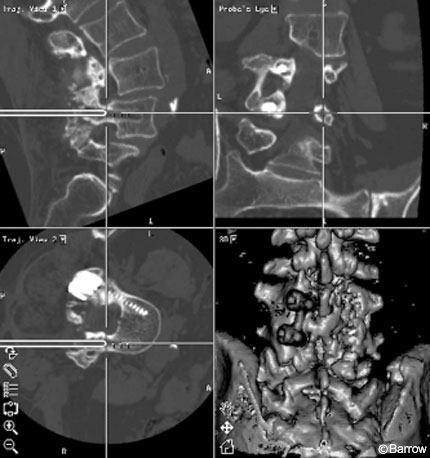
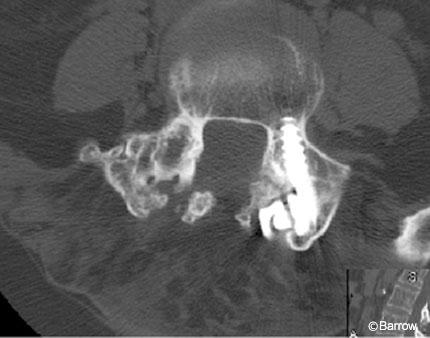
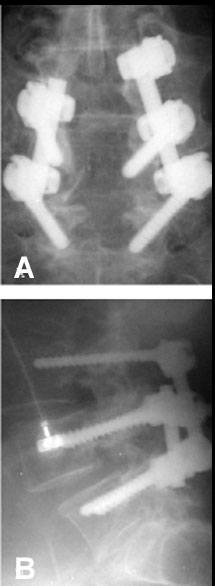
Image guidance was used to place the pedicle screws and proved to be helpful for several reasons. First, the patient’s previous laminectomies at L3 and L4 were associated with a significant fusion mass partially overlying the laminectomy defects. The three-dimensional (3D) image on the StealthStation served as a helpful guide during the dissection down to the spine. The bony landmarks on the patient’s fusion mass could be identified on the 3D image, which helped prevent inadvertent injury to the partially exposed thecal sac while facilitating a thorough dissection of the remaining posterior elements of the spine (Fig. 9). Second, the right L4 pedicle screw had to be placed in the same hole occupied by the previous L4 pedicle screw, which had been removed months earlier. Normal anatomic landmarks were significantly obscured by the fusion mass. This fusion mass also overlay the pedicle hole, making it difficult to localize (Fig. 10). With image guidance, the bone overlying the pedicle hole was localized and removed, allowing the probe to be inserted (Fig. 11) and the right L4 pedicle screw to be placed into the hole. At L5, image guidance was used to place the pedicle screws without difficulty. Postoperative radiographs revealed adequate positioning of the hardware (Fig. 12).
Case 3
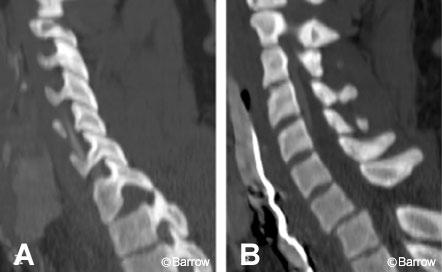
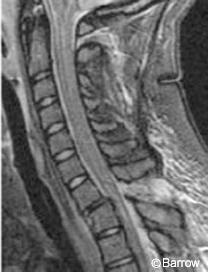
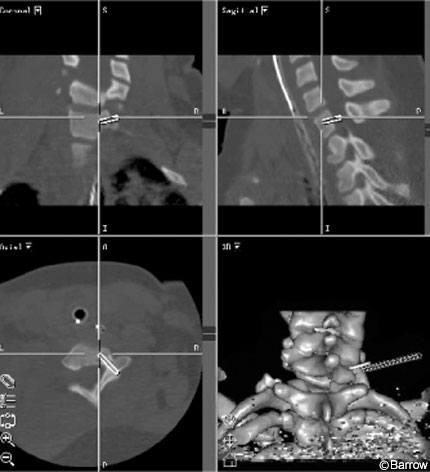
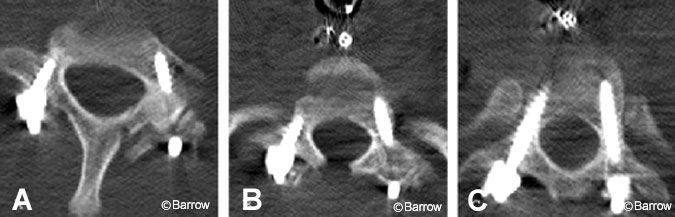
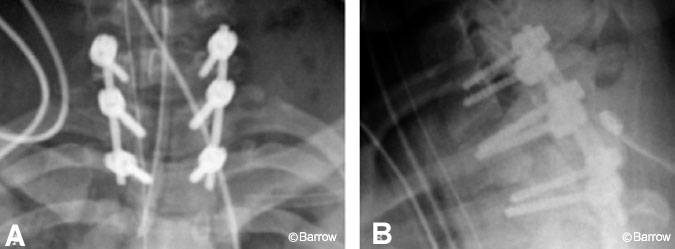
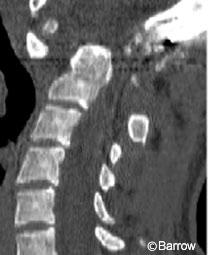
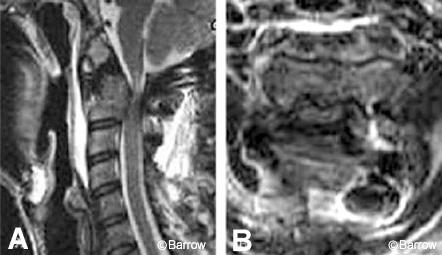
A 20-year-old female was involved in a motor vehicle accident, in which she sustained a right unilateral perched facet at C7-T1 with subluxation and angulation at that level (Fig. 13). Magnetic resonance (MR) imaging of the cervical spine showed significant posterior ligamentous injury (Fig. 14). Weighted traction was used in an attempt at closed reduction, which failed. The patient then underwent posterior fusion with pedicle screw fixation from C7-T2. Image guidance was key in placing the pedicle screws because the pedicles at these levels are so small (Fig. 15). Postoperative radiological studies revealed adequate placement of the hardware and anatomic alignment (Figs. 16 and 17).
Case 4
At an outside facility, a 38-year-old male underwent prior C1 laminectomy with occiput-to-C3 fusion to treat nonunion of a Type II odontoid fracture. He sought treatment about 6 months later for progressive myelopathy. Radiologic studies revealed a failed occipitocervical fusion with progressive kyphotic deformity at the occipitocervical junction and anterior subluxation of C1 on C2 with severe compromise of the spinal canal (Fig. 18). The patient underwent decompression and revision of his occiput-C3 fusion. Reduction was achieved at surgery, but postoperative MR imaging revealed persistent anterior compression by the C2 vertebral body (Fig. 19).
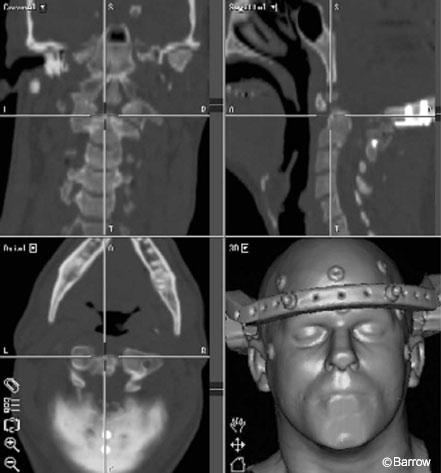
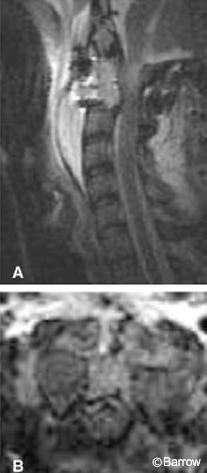
A transoral C2 corpectomy was performed using image guidance. Registration was accomplished with the use of scalp fiducials, similar to the registration method used with image-guided cranial applications. Image guidance helped define the lateral limits of the corpectomy and determined the location of the tips of the instruments in relation to the spinal canal (Fig. 20). The patient tolerated the procedure well. Postoperative MR imaging revealed adequate decompression of the spinal canal (Fig. 21).
Case 5
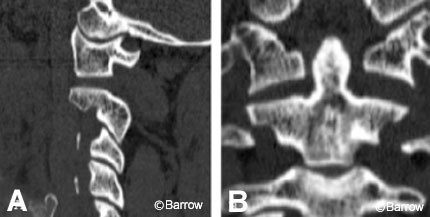
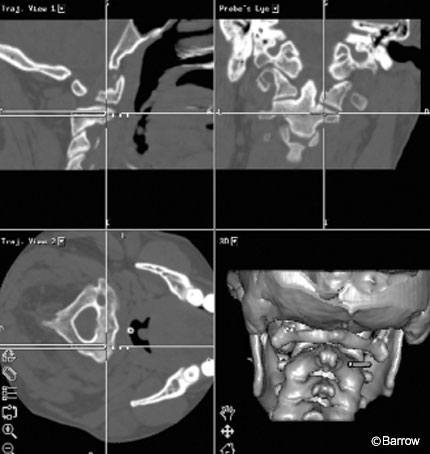
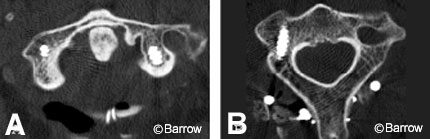
A 40-year-old male struck by an automobile sustained a C1-2 distraction injury (Fig. 22). He underwent posterior atlantoaxial arthrodesis consisting of bilateral C1 lateral mass screws connected to a right C2 pedicle screw and a left C2 laminar hook via a rod. An anomalous vertebral artery prevented insertion of a C2 pedicle screw on the left and necessitated the use of the laminar hook. The safe placement of the bilateral C1 lateral mass screws and the right C2 pedicle screw was facilitated by image guidance (Fig. 23). Postoperative computed tomography showed good reduction with adequate placement of all screws (Fig. 24).
Discussion
Image guidance is a useful adjunct to difficult spinal surgery cases by helping the surgeon ascertain appropriate entry points and trajectories for inserting spinal instrumentation. It is especially helpful in patients who have undergone prior surgery that has obscured the normal anatomic landmarks on the surface of the spine. For anterior decompressive procedures involving the upper cervical spine, image guidance aids the surgeon in determining the extent of the decompression, thereby helping to prevent inadvertent injury to adjacent vascular and neural structures. Image guidance should serve as an adjunct to spinal surgery. It should never serve as a substitute to thorough knowledge of spinal anatomy.
References
- Barnett GH, Kormos DW, Steiner CP, et al: Use of a frameless, armless stereotactic wand for brain tumor localization with two-dimensional and three-dimensional neuroimaging. Neurosurgery 33:674-678, 1993
- Barnett GH, Steiner CP, Weisenberger J: Intracranial meningioma resection using frameless stereotaxy. J Image Guided Surg 1:46-52, 1995
- Block O, Holly LT, Park J, et al: Effect of frameless stereotaxy on the accuracy of C1-2 transarticular screw placement. J Neurosurg 95:74-79, 2001
- Bolger C, Wigfield C: Image-guided surgery: Applications to the cervical and thoracic spine and a review of the first 120 procedures. J Neurosurg 92:175-180, 2000
- Foley KT, Smith MM: Image guided spinal surgery. Neurosurg Clin N Am 7:171-186, 1996
- Hodaie M, Musharbash A, Otsubo H, et al: Image-guided frameless stereotactic sectioning of the corpus callosum in children with intractable epilepsy. Pediatr Neurosurg 34:286-294, 2001
- Kalfas I, Kormos D, Murphy M, et al: Application of frameless stereotaxy to pedicle screw fixation of the spine. J Neurosurg 83:641-647, 1995
- Kamimura M, Ebara S, Itoh H, et al: Cervical pedicle screw insertion: Assessment of safety and accuracy with computer-assisted image guidance. J Spinal Disorders 13:218-224, 2000
- Olivier A, Germano IM, Cukiert A, et al: Frameless stereotaxy for surgery of the epilepsies: Preliminary experience. Technical note. J Neurosurg 81:629-633, 1994
- Paleologos TS, Wadley JP, Kitchen ND, et al: Clinical utility and cost-effectiveness of interactive image-guided craniotomy: Clinical comparison between conventional and image-guided meningioma surgery. Neurosurgery 47:40-48, 2000
- Wigfield C, Bolger C: A technique for frameless stereotaxy and placement of transarticular screws for atlanto-axial instability in rheumatoid arthritis. Eur Spine J 10:264-268, 2001
- Youkilis AS, Quint DJ, McGillicuddy JE, et al: Stereotactic navigation for placement of pedicle screws in the thoracic spine. Neurosurgery 48:771-778, 2001
