
Bone-Anchored Hearing Aid (BAHA)
Mark J. Syms, MD
Section of Neurotology, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
Abstract
Single-sided deafness is a common presenting symptom or outcome of therapy for acoustic neuromas. Single-sided deafness manifests with an inability to hear on the side of the loss, decreased ability to hear in background noise and loss of the ability to determine the location of the origin of a sound. The boneanchored hearing aid (BAHA) is effective for the rehabilitation of single sideddeafness. The BAHA is composed of an osseointegrated abutment, which is placed during a 45-minute outpatient surgery, and an external processor. Compared to individuals who wear hearing aids, patients with the BAHA system report greater comfort and often comment that they forget that they are wearing the device.
Key Words: BAHA device, bone conduction, hearing aid, hearing loss, single-sided deafness
Unfortunately, hearing loss is a common presenting symptom or outcome of therapy for acoustic neuromas. The resultant hearing loss is called singlesided deafness. Alternative causes of singlesided deafness are viral infections, Ménière’s disease, and head and ear trauma. Each year in the United States, an estimated 60,000 people acquire singlesided deafness.
Clinical Manifestations of Single-Sided Deafness
The manifestations of single-sided deafness are threefold. The most obvious problem is that a person with single-sided deafness is unable to hear on the side of the deaf ear. When hearing is lost in one ear, the ability to perceive the directionality of sound is also lost. Humans can identify the location of sound based on a split-second difference in the arrival time of a sound at the two ears. Based on the detected difference, the brain then calculates where the sound is coming from. The third manifestation of single-sided deafness is a decreased ability to hear speech in background noise. This difficulty is caused by the “head shadow effect,” in which the head acts as a sound barrier that separates the speaker’s voice from noise. Patients with single-sided deafness lose this capability.
Until recently, the rehabilitative options for single-sided deafness have been limited. A long-standing rehabilitative option for single-sided deafness is CROS (contralateral routing of signal) hearing aids. These devices consist of an in-theear or behind-the-ear microphone-transmitter placed on the deaf side. The sound is transmitted to a receiver on the hearing side via a wire or wirelessly. The sound is presented to the hearing ear and amplified if needed.
Patients and hearing professionals have been less than satisfied with the results of CROS hearing aids. Patients dislike the aesthetics of wearing two devices for one deaf ear. Patients also dislike the altered nature of sound in the hearing ear caused by the receiver occluding the ear canal. Most patients offered CROS hearing aids for a trial period do not purchase the aids. Of the people who do purchase the aids, only a fraction wear the aids full-time a year or two later. The true measure of patient satisfaction with hearing aids is whether the aids are used on a regular basis.

Bone-Anchored Hearing Aids
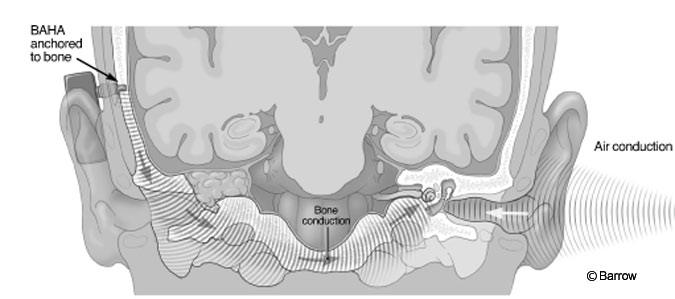
Bone-anchored hearing aid (BAHA) systems have been used in Europe since the late 1970s and were first approved by the Food and Drug Administration for use in individuals with mixed and conductive hearing loss in 1996. In 1999 the indications were expanded to include children 5 years and older. In 2002 the BAHA system was approved for the treatment of single-sided deafness. Currently, the BAHA system is worn by more than 17,000 people worldwide. The BAHA system uses bone conduction to transmit the sound from the nonhearing side to the functional cochlea. Bone conduction means that sound is transmitted through the skull via the bone (e.g., the sound of chewing on ice is very loud only to the person chewing the ice). Sound is not transmitted from the mouth to the ear via air. Rather, the sound travels directly via bone through the teeth, upper jaw and skull to the cochlea. The BAHA system (Fig. 1) uses the same mechanism of conduction.
Surgical Implantation of BAHA
One component of the BAHA system is an abutment that is surgically placed in the skull (Fig. 2). When an acoustic neuroma is removed, the implant can be placed at the time of removal or a few months later. If the procedure is performed separately, it can be performed in an outpatient setting in about 45 minutes under either general or local anesthesia.
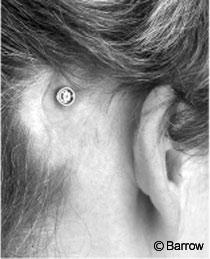
During placement of the implant, a hole is drilled and threaded in the skull. The titanium implant, which uses the same metal and technology as jaw implants for teeth, is slowly screwed into the hole. The muscle and fat between the bone and skin must be removed so conduction of the sound is not dampened. The skin flap is thinned enough to remove the hair follicles to insure that the area is free of hair once it has healed. A hole is punched through the skin through which the implant is expressed, and the incision is closed. A cap is snapped onto the abutment. Packing is placed between the abutment and the cap to encourage the skin to heal to the bone to prevent the accumulation of fluid or blood.
The cap is removed 1 week after surgery to assess the healing. If the skin flap has healed well, the healing cap is removed permanently (Fig. 3). If needed, however, packing is placed for an additional week. Once the area has healed, a brush is used to keep the interface between the skin and implant free of debris.

At least 3 months of healing is needed to enable osseointegration of the implant. The bone needs to grow into the implant, which becomes an integral part of the bone. Sound is thereby conducted and the implant remains secure. After 3 months of healing, the sound processor is placed on the abutment (Fig. 4). The color of the processor can be selected to match the patient’s hair. Typically, the sound processor has a sufficiently low profile so that it can be covered by the patient’s hair. It is placed behind the patient’s ear, which makes it even less noticeable. An advantage of the BAHA system is that no devices are placed in the ear, thereby improving cosmesis. Patients also prefer having an unobstructed ear canal in their only hearing ear. Compared to individuals who wear hearing aids, patients with the BAHA system report greater comfort and often comment that they forget that they are wearing the device.
Conclusions
The results of the BAHA system are exciting. Patients are pleased with their improved hearing and the comfort of the device. Patients with single-sided deafness who wear the device may understand soft speech originating on the side of the deafness, and their ability to understand speech in background noise improves. However, the BAHA system does not improve the ability to localize sound, which still arrives at only one cochlea. Overall, patients who have worn the BAHA system are happy with the device and wear it.
Recommended Readings
- Hol MK, Bosman AJ, Snik AF, et al: Bone-anchored hearing aid in unilateral inner ear deafness: A study of 20 patients. Audiol Neurootol 9:274-281, 2004
- Hol MK, Spath MA, Krabbe PF, et al: The bone-anchored hearing aid: Quality-of-life assessment. Arch Otolaryngol Head Neck Surg 130:394-399, 2004
- McLarnon CM, Davison T, Johnson IJ: Bone-anchored hearing aid: Comparison of benefit by patient subgroups. Laryngoscope 114:942-944, 2004
- Snik AF, Bosman AJ, Mylanus EA, et al: Candidacy for the bone-anchored hearing aid. Audiol Neurootol 9:190-196, 2004 5. Wazen JJ, Spitzer JB, Ghossaini SN, et al: Transcranial contralateral cochlear stimulation in unilateral deafness. Otolaryngol Head Neck Surg 129:248-254, 2003
