Volume 22, Issue 2, 2006
Table of Contents
- Comments from the Editor
- Management of Thoracic Vertebral Giant Cell Tumor with Complete Spondylectomy: Case Report
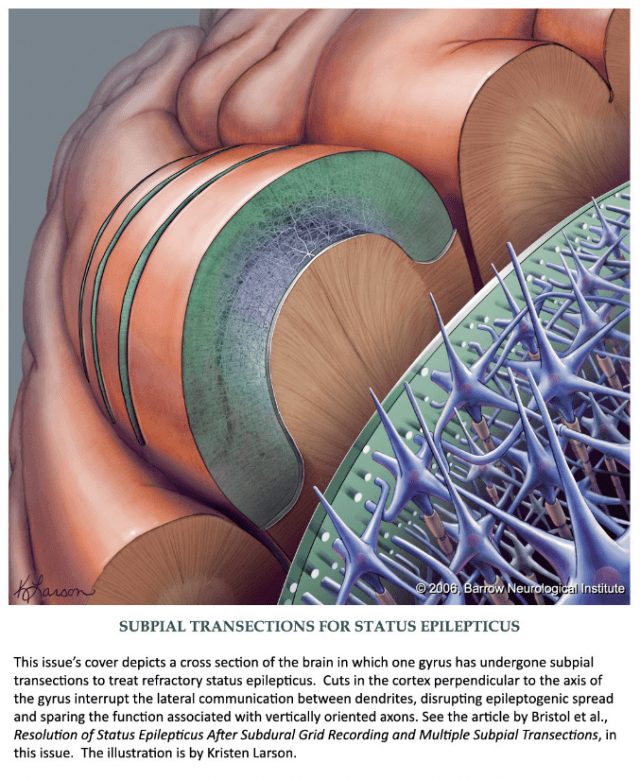
- Resolution of Status Epilepticus After Subdural Grid Recording and Multiple Subpial Transections
- Intracerebral Schwannomas: Case Report and Review of the Literature
- Lateral Ventricle Neoplasm with Skeletal Muscle Differentiation
- Brain Activation Patterns in the Affected and Nonaffected Hand After Subcortical Stroke: Two Case Reports Using Serial fMR Imaging
Journal Information
Editor-in-Chief
Robert F. Spetzler, MD
President, St. Joseph’s Hospital and Medical Center
Linda Hunt
Editorial Staff
Senior Editor
Shelley A. Kick, PhD
Assistant Editor
Dawn Mutchler
Production Editor
Jaime L. Hoffman
Editorial Assistant
Judy Wilson
Medical Illustrators
Mark Schornak, MS
Kristen L. Larson, MS
Three-Dimensional Modeler
Michael Hickman
Graphic Designer
Jaime L. Hoffman
Section Editors
Neurology
Timothy L. Vollmer, MD
Neurosurgery
Volker K. H. Sonntag, MD
Neurobiology
Ronald J. Lukas, PhD
Neuroanesthesiology
Peter A. Raudzens, MD
Neuroradiology
Shahram Partovi, MD
Neuropathology
Stephen W. Coons, MD
BNI News Editor
Andrew G. Shetter, MD
Neuroscience Nursing
Virginia Prendergast, RN, NP-C, CNRN