
Hypothalamic Hamartoma
Overview
Hypothalamic hamartomas (HH) are rare, benign (noncancerous) tumors of the hypothalamus, a region of your brain that regulates many of your body’s systems. Hypothalamic hamartomas affect people from infancy through adulthood and commonly cause seizures, precocious (early) puberty, hormonal imbalances, and cognitive and behavioral problems.
Hypothalamic hamartomas are usually diagnosed during evaluation of people for epilepsy or precocious puberty.
Hypothalamic Hamartoma Symptoms
The symptoms of a hypothalamic hamartoma (HH) can include:
- Seizures
- Precocious (early) puberty
- Hormone imbalances
- Cognitive impairment
- Behavioral problems
- Emotional difficulties
frequent gelastic (or laughing) seizures. You may not be able to tell the difference between a gelastic seizure and normal laughter.
The difficulty in identifying gelastic seizures usually delays the diagnosis of epilepsy caused by a hypothalamic hamartoma. Doctors sometimes can have difficulty recognizing gelastic seizures because they are rare, and children affected by them generally develop normally.
Between the ages of four and 10 years old, you may notice the seizures becoming more disabling, with the emergence of different seizure types, such as:
- Complex partial seizures (diminished or altered consciousness with involuntary but coordinated movements)
- Generalized convulsions (involuntary shaking, twitching, and disorganized movements)
- Drop or atonic seizures (brief loss of muscle tone leading to falls)
worsening school performance, and the following behavioral problems:
- Tantrums
- Rage attacks
- Social isolation
Some children with a hypothalamic hamartoma may have endocrine (hormonal) disturbances. Central precocious puberty (early puberty) is the most common sign of these disturbances, and may be the only symptom of hypothalamic hamartoma that your child has.
Not all people with a hypothalamic hamartoma have the same symptoms or the same age of onset. While you might notice gelastic seizures in your newborn, it is also possible that seizures will not develop until later in life. Seizures caused by a hypothalamic hamartoma generally do not respond to medication.
Please seek the help of a licensed medical professional if you are concerned about your health, and dial 9-1-1 if you are experiencing an emergency.
Hypothalamic Hamartoma Treatments
Surgical Removal
Our neurosurgeons at Barrow Neurological Institute at Dignity Health St. Joseph’s Hospital and Medical Center are one of just a few groups in the world with significant experience using the transcallosal approach to remove hypothalamic hamartomas. This approach uses the natural gap between the two hemispheres of your brain to create an avenue to access and remove the tumor.
We also use more traditional subtemporal or orbitozygomatic approaches if they offer the best chance of success. This surgery begins on the side of your head and passes under your brain and above the base of your skull to reach the lesion.
Less-invasive endoscopic surgery can be considered when the size and anatomical positioning of the lesion allows.
Laser Generated Stereotactic Thermoablation
Laser generated stereotactic thermoablation is a new minimally invasive technology that uses energy in the form of light to destroy tumors or damaged tissue. The energy from the laser causes the temperature of the target tissue—in this case a hypothalamic hamartoma—to rise, destroying it.
Computerized safety mechanisms automatically turn the laser off if it approaches brain tissue surrounding the tumor. Magnetic resonance images (MRI) are also used further improve the accuracy of the procedure and guide the placement of the laser.
Gamma Knife Radiosurgery
Gamma Knife radiosurgery uses many beams of radiation that converge on a single point to shrink tumors. Each individual beam is not powerful enough to destroy healthy tissue, but at the point where the beams meet sufficient energy is concentrated to destroy tumor cells.
Treatment and Evaluation Process
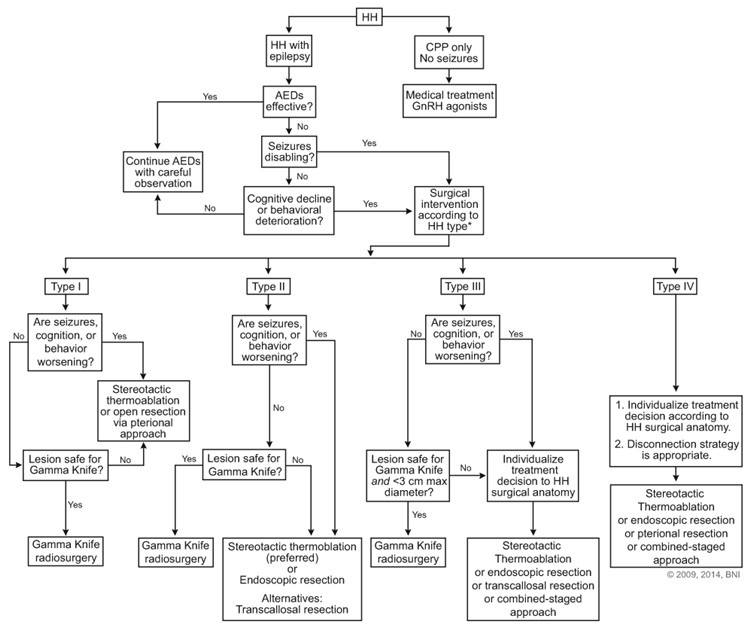
There is not a single treatment plan for hypothalamic hamartoma that is a fit for everyone. Depending on symptoms, response to medication, age, and other factors, you or your loved one’s treatment may take a unique course. The flowchart below shows some of the more common ways that hypothalamic hamartomas are treated at Barrow.
Common Questions
How common are hypothalamic hamartomas?
Hypothalamic hamartomas are very rare, with approximately one tumor occurring in every 200,000 people.
Who gets hypothalamic hamartomas?
Hypothalamic hamartomas form before birth and can occur in people of any gender or ethnicity.
How are hypothalamic hamartomas diagnosed?
Hypothalamic hamartomas are diagnosed by assessment of neurological symptoms, magnetic resonance imaging (MRI), and neurological tests. Early detection can improve the likelihood of successful treatment, especially for children who have worsening seizures or whose learning skills or behavior have begun to deteriorate.
MRI is used to locate a hypothalamic hamartoma and confirm the diagnosis. Hypothalamic hamartomas can be small and difficult to detect, so interpretation by a doctor that specializes in neuroradiology is desirable.
Electroencephalography (EEG) may also be used to identify seizure patterns that suggest a hypothalamic hamartoma



