
Cerebellopontine Angle Lipoma Presenting with Tinnitus and Vertigo: Case Report
Ernesto Coscarella, MD
Sergio Paolini, MD*
Robert F. Spetzler, MD
A. Giancarlo Vishteh, MD
Division of Neurological Surgery, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona *Current Address: Department of Neurological Sciences, Neurosurgery I, “La Sapienza” University, Rome, Italy
Abstract
A 47-year-old female sought treatment for tinnitus and vertigo. Magnetic resonance imaging revealed a right cerebellopontine angle (CPA) mass extending into the internal acoustic canal. At surgery a glistening mass encased the seventh and eighth cranial nerves, anterior inferior cerebellar artery, and petrosal vein. Lipoma was diagnosed intraoperatively and debulking ensued. Surgical resection is not indicated for CPA lipomas unless intractable symptoms other than hearing loss develop.
Key Words: cerebellopontine angle, lipoma, tumor
Intracranial lipomas account for only about 0.3% of all intracranial tumors.4,11 Typically, they involve midline structures such as the corpus callosum, quadrigeminal plate, and suprasellar area and rarely occur within the cerebellopontine angle (CPA). To date, 36 surgically treated cases have been reported.1,13,17 Most patients with lipomas, however, remain asymptomatic, and the tumors are described only after autopsy.2,12 More recently, lipomas have been described as incidental findings on magnetic resonance (MR) imaging.1,20 If symptoms occur in association with a CPA lipoma, they usually mimic those associated with acoustic neuromas. We describe a patient complaining of tinnitus and vertigo who underwent subtotal resection of a right CPA lipoma.
Case Report
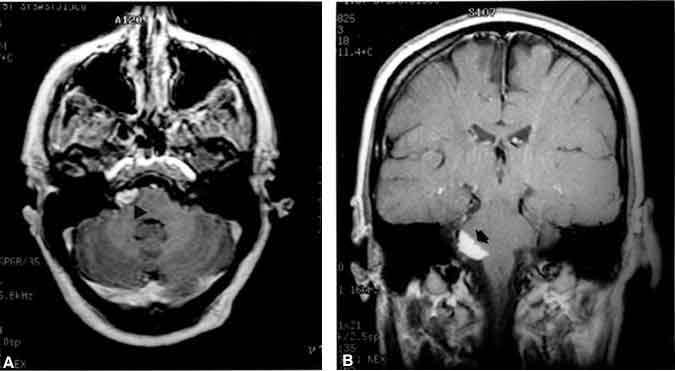
A 47-year-old female sought treatment for tinnitus and vertigo. Brain MR imaging revealed a mass at the CPA that extended into the internal acoustic canal. On T1-weighted MR images, the signal intensity of the lesion was high, and the surrounding area did not enhance upon administration of gadolinium (Fig. 1). On T2-weighted MR images, the signal intensity of the lesion was low.
The patient underwent a right retrosigmoid craniotomy. A glistening mass interdigitated with the seventh and eighth cranial nerves, anterior inferior cerebellar artery, and petrosal vein. The lesion extended inferiorly and appeared to be independent of the choroid plexus that extruded from the foramen of Luschka. The mass was debulked, and the specimen was sent for histopathological examination. Lipoma was diagnosed. Aggressive resection was not pursued because the tumor adhered tightly to the involved neurovascular structures. The wound was closed, and the patient was transferred to the intensive care unit in stable condition. Her postoperative course was uneventful, and she was discharged home 2 days later with intact hearing and facial nerve function.
Discussion
Lipomas are commonly referred to as “tumors.” Credible pathogenetic theories, however, consider lipomas to be congenital malformations with one or two possible origins. A dysraphic disorder may cause mesodermal inclusions to remain trapped within the closing neural tube, or dysgenesis of indigenous tissue may cause the meninx primitiva to differentiate abnormally into adipose tissue.2,20 The former theory would account for the reportedly high incidence of associated intracranial malformations such as micropolygyria, hypoplasia, or agenesis of the corpus callosum.
Very rarely, lipomas arise in the CPA. In this region they show a predilection for the pontomedullary junction near the emergence of the seventh and eighth cranial nerves. The abundance of arachnoid at this site, as in other sites favored by these lesions, corroborates that lipomas originate as “maldifferentiated leptomeninges.”18 The close relationship of lipomas of the CPA to the eighth cranial nerve is both peculiar and unexplained but confirmed by the sporadic occurrence of purely intracanalicular lipomas.8,16,18
The incidence of CPA lipomas is difficult to determine. Due to the non-neoplastic and usually asymptomatic behavior of lipomas, their true incidence is unknown but will likely be better defined as the number of MR imaging-diagnosed cases increases. Recently, Bigelow et al.1 added 17 additional cases to 67 previously reported lipomas associated with the CPA or internal carotid artery. Only 36 cases were surgically diagnosed and involved the CPA angle; 43 lesions were purely intracanalicular or diagnosed radiologically. Five were incidental autopsy findings.
MR imaging has now achieved a very high sensitivity and specificity for detecting lipomas. On T1-weighted MR images, lipomas typically appear hyperintense compared with brain tissue and hypointense on T2-weighted MR images. As in our case, they do not enhance after the administration of contrast agent. In the CPA the lesion should be distinguished from arachnoid cysts and dermoid and epidermoid tumors. Lipomas can be misdiagnosed as the latter two lesions, especially if a large amount of cholesterol is present in the latter.17
Intracranial lipomas are almost static lesions, and symptoms are usually related to coexisting malformations rather than to the lipoma itself. Unlike their other intracranial counterparts, CPA lipomas have not been reported in association with other malformations. Thus, when present, symptoms reflect impingement on cranial nerves or the brain stem by the lipomatous mass. Like acoustic neuromas, eighth nerve dysfunction is the most frequent presenting symptom although hemifacial spasm or weakness 9,14,19 and trigeminal neuralgia 2,7,10 have also been reported.
From a surgical perspective, lipomas act as true tumors. Moreover, they are strikingly adherent to surrounding structures, encasing vessels and nerves rather than displacing fatty tissue. Pathological specimens demonstrate a thorough infiltration of the adipose tissue within the nerve bundles and in between the single fascicles.3 This infiltration likely accounts for the poor outcomes that follow attempts to dissect the tumor away from the nerves.
Hearing loss is highly unlikely to recover after surgery.1,17 Of the cases reviewed by Bigelow et al.,1 64% experienced increased hearing loss after surgery. Other symptoms, however, did improve.2,5,14 Good outcomes have been reported after vestibular and partial trigeminal neurectomy for the relief of intractable vertigo or trigeminal neuralgia, respectively.1,7,10,15 In our case, the patient’s tinnitus remained at baseline. Reducing the intake of alimentary fat has also been reported to reduce the size of a lipoma.1,6
Overall, surgical treatment should be reserved for the small subset of patients with intractable vestibular symptoms or symptoms related to the compression of the fifth and seventh cranial nerves or brain stem. Follow-up imaging is prudent in most cases.”
References
- Bigelow DC, Eisen MD, Smith PG, et al: Lipomas of the internal auditory canal and cerebellopontine angle. Laryngoscope 108:1459-1469, 1998
- Budka H: Intracranial lipomatous hamartomas (intracranial “lipomas”). A study of 13 cases including combinations with medulloblastoma, colloid and epidermoid cysts, angiomatosis and other malformations. Acta Neuropathol (Berl) 28:205-222, 1974
- Christensen WN, Long DM, Epstein JI: Cerebellopontine angle lipoma. Hum Pathol 17:739-743, 1986
- Eghwrudjakpor PO, Kurisaka M, Fukuoka M, et al: Intracranial lipomas. Acta Neurochir (Wien) 110:124-128, 1991
- Ferreira MP, Ferreira NP, Lenhardt R: Lipoma of the cerebellopontine angle. Case reports and literature review. Arq Neuropsiquiatr 52:58-63, 1994
- George WE, Jr., Wilmot M, Greenhouse A, et al: Medical management of steroid-induced epidural lipomatosis. N Engl J Med 308:316-319, 1983
- Graves VB, Schemm GW: Clinical characteristics and CT findings in lipoma of the cerebellopontine angle. Case report. J Neurosurg 57:839-841, 1982
- Greinwald JH, Jr, Lassen LF: Lipomas of the internal auditory canal. Laryngoscope 107:364-368, 1997
- Inoue T, Maeyama R, Ogawa H: Hemifacial spasm resulting from cerebellopontine angle lipoma: Case report. Neurosurgery 36:846-850, 1995
- Kato T, Sawamura Y, Abe H: Trigeminal neuralgia caused by a cerebellopontine-angle lipoma: Case report. Surg Neurol 44:33-35, 1995
- Kazner E, Stochdorph O, Wende S, et al: Intracranial lipoma. Diagnostic and therapeutic considerations. J Neurosurg 52:234-245, 1980
- Kolb J: Zur pathologie der fettgeschwulste. Z K K Gesellsch Arzte Wien 673-675, 1859
- Leibrock LG, Deans WR, Bloch S, et al: Cerebellopontine angle lipoma: A review. Neurosurgery 12:697-699, 1983
- Levin JM, Lee JE: Hemifacial spasm due to cerebellopontine angle lipoma: Case report. Neurology 37:337-339, 1987
- Pensak ML, Glasscock ME, 3rd, et al: Cerebellopontine angle lipomas. Arch Otolaryngol Head Neck Surg 112:99-101, 1986
- Saunders JE, Kwartler JA, Wolf HK, et al: Lipomas of the internal auditory canal. Laryngoscope 101:1031-1037, 1991
- Schuhmann MU, Ludemann WO, Schreiber H, et al: Cerebellopontine angle lipoma: A rare differential diagnosis. Skull Base Surg 7:199-205, 1997
- Singh SP, Cottingham SL, Slone W, et al: Lipomas of the internal auditory canal. Arch Pathol Lab Med 120:681-683, 1996
- Sprik C, Wirtschafter JD: Hemifacial spasm due to intracranial tumor. An international survey of botulinum toxin investigators. Ophthalmology 95:1042-1045, 1988
- Truwit CL, Barkovich AJ: Pathogenesis of intracranial lipoma: An MR study in 42 patients. AJR 155:855-865, 1990
