
Diagnosis and Management of Deformational Plagiocephaly
Timothy R. Littlefield, MS
Jacque L. Reiff, RN, BS*
Harold L. Rekate, MD*
Cranial Technologies, Inc., Phoenix, Arizona
*Division of Neurological Surgery, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
Abstract
Once a relatively rare condition, the incidence of deformational plagiocephaly has increased dramatically in recent years, partially as a result of the American Academy of Pediatrics’ Back to Sleep campaign established to prevent sudden infant death syndrome. The resulting deformity is often much more than just a “flat head.” This article identifies which infants are at highest risk for developing deformational plagiocephaly and presents guidelines for the management of infants with this condition.
Key Words: lambdoid synostosis, plagiocephaly, torticollis
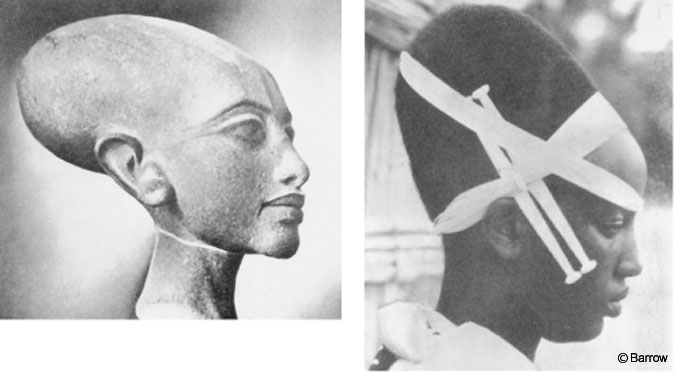
For thousands of years, numerous cultures throughout the world have practiced artificial head molding. Some societies believed that a specific cranial configuration would enhance an individual’s mental or physical abilities while others used a unique head shape to distinguish individuals as member of the nobility (Fig. 1). The methods used to distort the cranium have been as varied as the cultures that practiced them, but each involved applying an external molding force to a growing infant’s cranium to achieve the desired result.[18] These forces were applied continuously until the infant was 6 to 8 months old, whereupon the distortion became permanent.[6]
Today this practice is almost nonexistent; nonetheless, the number of infants with similar cranial deformities is increasing. As with the artificial methods described above, the distortion is the result of an external molding force applied to an infant’s malleable cranium. The condition is known as deformational or positional plagiocephaly (from the Greek, plagio for oblique and kephale for head), and the resulting deformity is often much more than just a “flat head.” In infants with deformational plagiocephaly, the back of the head is often flattened asymmetrically, the ear is misaligned, and the face is significantly asymmetrical. This condition concerns parents but is often dismissed as a problem that will resolve on its own.
Deformational plagiocephaly is not a life-threatening disorder, but steps can and should be taken in early infancy to avoid deformation of the skull and face. Pediatricians can play a key role in reducing the incidence of this condition by understanding the risk factors that make certain infants susceptible, by screening all patients, and by encouraging parents to implement simple conservative intervention techniques. This article reviews how deformational plagiocephaly develops, identifies the infants at greatest risk, discusses how to diagnose the condition, and offers guidelines for the management of infants with deformational plagiocephaly.
Risk Factors for Deformational Plagiocephaly
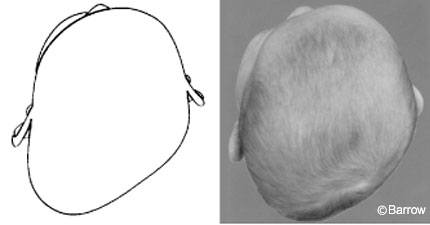
 The infant cranium experiences significant distortion as it passes through the birth canal. This temporary deformation is necessary to ensure successful labor and delivery, and the abnormal head shape that results returns to normal within the first few weeks of life. Often, however, the infant cranium becomes deformed as the result of external molding forces applied prenatally, postnatally, or both.[2,3,11,16,23,24] A large variety of head shapes can ensue, but the most common shape is a parallelogram as viewed from the top of the baby’s head (Fig. 2). Many risk factors are associated with deformational plagiocephaly (Table 1).
The infant cranium experiences significant distortion as it passes through the birth canal. This temporary deformation is necessary to ensure successful labor and delivery, and the abnormal head shape that results returns to normal within the first few weeks of life. Often, however, the infant cranium becomes deformed as the result of external molding forces applied prenatally, postnatally, or both.[2,3,11,16,23,24] A large variety of head shapes can ensue, but the most common shape is a parallelogram as viewed from the top of the baby’s head (Fig. 2). Many risk factors are associated with deformational plagiocephaly (Table 1).
Restrictive Uterine Environment
A restrictive uterine environment is considered one of the leading risk factors for the development of deformational plagiocephaly. The initial distortion of the infant’s cranium actually begins in utero, and it continues to deform after birth. A number of factors can be involved: very large fetuses, fetuses with very large heads, multiple fetuses, a small maternal pelvis, a small or malformed uterus, increased uterine or abdominal muscle tone, or an excess or paucity of amniotic fluid.[2,16] A breech orientation also can lead to an abnormal head shape when the infant’s head becomes wedged under the mother’s ribs, restricting the lateral growth of the cranium.[7] In retrospect, many mothers of children with deformational plagiocephaly report experiencing considerable pain in the hip or pain radiating into the leg related to the pressure of the fetus on the pelvic wall.
Congenital Muscular Torticollis
Although a restrictive intrauterine environment can distort the cranium directly, it also can shorten the strap muscles of the neck asymmetrically. This effect is well recognized when associated with unilateral shortening of the sternocleidomastoid muscle, but it also can be associated with asymmetric shortening of one of the trapezius muscles. Such unilateral shortening restricts mobility of the neck and is called congenital muscular torticollis (CMT).
Historically, CMT has been linked to the development of plagiocephaly as a result of the persistent positioning an infant’s head against the mattress.[12] Even mild forms of neck immobility can cause an infant to favor a single position. CMT is most often cited as the result of unilateral fibrosis or shortening of the sternocleidomastoid muscle. In the authors’ experience, however, abnormalities of the sternocleidomastoid muscle are rare, and CMT is often associated with abnormalities of the trapezius muscle. CMT may be quite subtle, and the examiner must look for evidence of asymmetry in the range of motion of these muscle groups.
Prematurity
Prematurity can increase the risk of positional head molding for several reasons. Prematurity itself can affect the ability of an infant’s cranium to resist deformation. During the last 10 weeks of gestation, the stiffness of the calvarial bones increases 5- to 10-fold.[14] Premature delivery makes the already malleable cranium even more susceptible to the external molding forces. Many premature infants are also more likely to be either mentally or physically delayed, and these delays can inhibit the normal repositioning of the head during rest. Finally, many premature infants spend extended periods in the neonatal intensive care unit on a respirator. A respirator artificially maintains the head in a fixed orientation, typically from side to side, and a long and narrow scaphocephalic-shaped head can result.
Supine Sleeping Position
Before 1992 the primary risk factors associated with deformational plagiocephaly were considered to be a restrictive uterine environment and CMT, as discussed above. After the publication of the American Academy of Pediatrics’ recommendation to place infants on their back to reduce the risk of sudden infant death syndrome (SIDS), craniofacial centers around the country began to observe a dramatic increase in the number of infants with abnormally shaped heads. By 1996 several studies had documented the cause-and-effect relationship between a supine sleeping position and the development of plagiocephaly.[1,11,24]
The recognition that a supine sleeping position has increased the number of infants who develop deformational plagiocephaly should not be interpreted as a criticism of this important recommendation. Since its inception, the Back-to-Sleep campaign has saved thousands of lives: The incidence of SIDS has decreased more than 40% since 1992.[23] With such a dramatic reduction in SIDS, it is unlikely that the recommendation will be reversed. Consequently, pediatricians will be confronted with an increasing number of infants with deformational plagiocephaly.
Diagnosis of Deformational Plagiocephaly
Deformational plagiocephaly can be diagnosed quickly and easily if the child’s head shape is observed from above as part of the standard well-baby evaluation. Observing the baby’s face from a frontal perspective often fails to reveal the deformity. When viewed from the vertex, however, the child’s head looks like a parallelogram with the occiput flattened on one side (Fig. 2). Compensatory changes are evident in the remainder of the skull. On the side of the occipital flattening, the frontal region may bulge and the ear is often distorted anteriorly. The contralateral side is characterized by flattening of the forehead and occipital bulging. Some degree of facial distortion is usually apparent and becomes more evident when the infant is held up to a mirror.
Typically, the diagnosis of deformational plagiocephaly is straightforward. It is the only condition that makes the head look like a parallelogram when viewed from the vertex.[9] There is, however, considerable confusion in the literature regarding the differentiation of deformational plagiocephaly from lambdoid craniosynostosis. Lambdoid synostosis is exceptionally rare (prevalence, 0.003%) and represents only 1 to 3% of cases of true craniosynostosis.[21] In lambdoid synostosis, the head is shaped like a trapezoid, not a parallelogram (Fig. 3). A prominent bulge is visible behind the ear on the involved side. The ear is pushed forward and downward. The forehead is flattened on the same side of the skull as the occiput.

A physical examination is usually sufficient to diagnose both deformational plagiocephaly and lambdoid synostosis. When, however, the diagnosis is questionable, a computed tomography (CT) study with bone windows can be used to resolve the issue. In deformational plagiocephaly, the sutures may be distorted but are definitely open. In lambdoid synostosis, the lambdoid suture is closed and a ridge that is easily seen on CT is formed. In lambdoid synostosis, CT also reveals a much more dramatic degree of distortion of the skull base than occurs in deformational plagiocephaly. If questions persist regarding the diagnosis, a pediatric neurosurgeon or craniofacial surgeon should be consulted.
Dysfunction of the neck musculature is almost a universal finding in patients with deformational plagiocephaly. Sometimes this dysfunction is overt, and infants are unable to turn their head beyond the midline. More often, however, the problem is subtle. Neck dysfunction can be diagnosed in two ways. The “rotating stool test” can be used in children 3 months or older (those with independent head control). In this test the examiner holds the baby in his or her lap while sitting on a rotating stool. The parent is seated at a distance from the child and asked to engage the child or get the child’s attention. As the examiner rotates the stool 90 degrees, first to the right and then to the left, the child attempts to remain fixed on the parent. As the stool is rotated to one side, the infant maintains eye contact by rotating the head over the shoulder. When the rotation is in the opposite direction, a child with torticollis either rotates the entire body or breaks eye contact with the parent. This test not only diagnoses neck muscle dysfunction, but it also helps the parent to understand the importance of the neck dysfunction in the development of plagiocephaly. This understanding increases compliance from the family in terms of performing the neck-stretching exercises that can be used to help treat the condition (described below).
The second method of diagnosing neck muscle dysfunctions involves performing the neck-stretching exercises. When these exercises are performed, a definite resistance to either rotation of the chin to the shoulder or tipping the infant’s ear to the shoulder can be observed. Because torticollis can involve multiple muscles, the neck-stretching exercises and position modification help improve any combination of muscle disorders.
Screening for neck dysfunction also should include observing the neck for uneven creases and viewing the infant from the back of the head to determine if the level of one ear is unequal compared to the other. In very young infants, an unequal breast-feeding pattern often provides clues that the infant may have problems with neck mobility. In this situation, the child may nurse well on one side, but only for a few moments on the other because of neck discomfort.
Treatment Options
Knowledge of treatment options becomes essential when infants already have an existing deformity. The key to the successful management of infants with deformational plagiocephaly is early diagnosis and treatment. Most forms of intervention rely on redirecting symmetrical growth of the skull. Almost 80% of this growth occurs before 12 months of age; only a small window of opportunity is available to provide conservative, nonsurgical treatment. Typically, the earlier the deformity is identified and treated, the more likely is the chance of correcting it completely.[13] Recommended guidelines for the treatment of deformational plagiocephaly are discussed below.
Repositioning
In most cases the original deformity is caused by infants holding their head in a single position at rest. Consequently, repositioning the infant off this flat spot should return the head to a more normal configuration. If the deformity is detected at an early age, repositioning can be a successful treatment. Several clinical investigations have reported some success with simple position modification in infants less than 6 months old who were categorized as having a mild-to-moderate cranial deformity.[8,19] Six months of age is the upper limit at which repositioning is believed to be effective because most infants develop the ability to reposition themselves by that age.
Parents need instruction and encouragement to modify their child’s position (see Positioning Protocol). Repositioning can be exceptionally difficult to achieve because most infants develop their own “position of comfort.” Parents are more likely to comply with repositioning if they understand the pathophysiology of the deformity and that modifying the child’s environment can influence head shape. Parents should be encouraged to reposition their child frequently by alternating the arm in which the child is carried and fed and by rotating the position of toys in the crib, stroller, swing, and car seat. All of these activities improve the range of motion of the neck and rotate the pressure sites on the skull. If the deformity is moderate to severe, repositioning the infant off the flattened area may not be physically possible due to the asymmetry of the back of the head.
Parents also need education about the importance of supervised “tummy time” and how it promotes development of the trunk musculature and improves both gross and fine motor skills. Many parents, understandably concerned about SIDS, are hesitant to place their child prone, even while the infant is awake and supervised. In our treatment population, parents often report that the child cried so much that they immediately returned the baby to his or her back. Parents often respond to crying by leaving the child on his or her back and orienting toys or other entertainment to accommodate. Thus the time the infant spends supine increases and any stimulus for the infant to change its position is removed.
Neck-Stretching Exercises
Most infants who develop plagiocephaly have some form of neck dysfunction. Therefore, the importance of physical therapy and neck-stretching exercises cannot be overemphasized. As discussed earlier, persistent positioning of the head against a mattress is often caused by CMT, involving either the sternocleidomastoid or trapezius muscles. Resolution of torticollis through aggressive and repetitive neck-stretching exercises can remove this restriction and allow infants at rest to alter their head orientation more freely.
When used in conjunction with repositioning at an early age, the combination of exercise and altered positioning can improve an abnormally shaped head. Suggested exercises for torticollis are presented in the Neck-Stretching Exercises parent-education handout. Severe cases of CMT can require surgical release.
If a child has severe torticollis or torticollis in conjunction with a syndrome or multiple congenital anomalies, range-of-motion exercises may be contraindicated. A radiographic series of the cervical spine, an orthopedic or neurosurgical evaluation, and formal physical therapy may be warranted.
Orthotic Management
Although first introduced in 1979, the use of orthotic helmets for the treatment of positional plagiocephaly did not gain widespread acceptance until recently.[3] With the dramatic increase in the number of infants developing positional plagiocephaly, numerous orthotic programs have been established throughout the country.
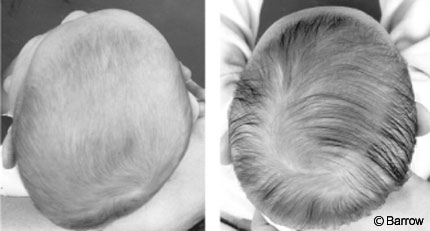
Dynamic Orthotic Cranioplasty[SM] (Cranial Technologies, Phoenix, Arizona, Fig. 4) was developed as a proactive approach for treating this condition. This orthosis applies a mild constant pressure on the most anterior and posterior prominences where growth is undesirable. Room is left in the adjacent flattened regions to encourage the cranium to grow in those areas. The orthosis is adjusted frequently to ensure proper growth of the head and to monitor the correction being achieved. Treatment may be initiated as early as three months or as late as 18 months of age although early intervention is certainly advantageous.[13] Numerous clinical studies have demonstrated the success of this technique (Fig. 5).[13,15,22]
Surgery
The role of surgery remains controversial for the most severe cases of deformational plagiocephaly. Many cranial remodeling operations have been performed primarily when this condition was attributed to lambdoidal craniosynostosis.[4,5,17,20] In severe cases referred too late to benefit from orthotic treatment or in whom the devices have failed to improve the child’s condition, surgery, which is still performed in a number of centers, may be warranted.
If surgery is considered necessary, several types of surgical procedures can be used to correct the deformity. These operations range from a strip craniectomy to occipital transposition or formal craniofacial reconstruction. Surgical management of this condition is rare. If indicated, surgical options should be discussed with a pediatric neurosurgeon or craniofacial surgeon to determine the appropriate timing and type of procedure.
Conclusions
Current research on the incidence of deformational plagiocephaly suggests that almost 20% of infants have noticeable flattening of the head, asymmetry of the skull base and face, or both. In many of these cases the molding is mild, and parents may be advised to reposition the child and to observe the infant closely to ensure that the deformity does not worsen. Approximately one in every 65 infants develops a more significant deformity and may require a more aggressive form of treatment to normalize the shape of the head. Although this determination can be subjective, most physicians agree that a notable disparity between the right and left sides of the back of the head, distortion of the skull base (misalignment of the ears), and/or facial asymmetry constitute at least a moderate deformity. For such infants, a more aggressive treatment regimen, including neck-stretching exercises and orthotic management, may be indicated. The type and extent of treatment are determined by a joint decision made by the physician and the family.
Deformational plagiocephaly is not a progressive disease like craniosynostosis. Severe cases, however, can cause severe emotional and body image problems for patients. These effects are similar to those experienced by children whose head is deformed by craniosynostosis.[21] Excessive teasing is common. One adult patient relates being prevented from playing high school football because he could not find a football helmet to fit. Recently, we have been contacted by three adult males (ages 16, 25, and 45) all inquiring whether it was still possible to correct their deformity. A mother of a 6-year-old boy had the same request because her son was being teased relentlessly and she could not find a bicycle helmet to fit his lopsided head. With the ever increasing number of infants developing deformational plagiocephaly, pediatricians have a unique opportunity to reduce the number of affected patients by early screening, by identifying patients at risk, and by educating parents about the importance of rotating infants and providing supervised tummy time. Early intervention and proper parental instruction have the potential to reduce the incidence of deformational plagiocephaly significantly.[10]
Treatment of deformational plagiocephaly requires the concerted effort of pediatricians and parents. It begins with an assessment of the infant’s head shape and neck range-of-motion during the first newborn office visit and again at the 2-month evaluation. Immediate intervention should begin if torticollis or cranial asymmetry is noted.
When parents are equipped with information about the cause and treatment of deformational plagiocephaly, they are empowered to become active participants in their child’s care. Their rapport with the physician also increases. Early intervention increases the opportunity for the deformity to be corrected with conservative, low-cost treatment A late diagnosis or advising parents not to worry because the head will round out on its own can cause parents frustration and anxiety when the deformity persists beyond the infant’s first birthday. Such advice also prevents patients from benefiting from the effective conservative interventions identified above.
References
- American Academy of Pediatrics AAP Task Force on Infant Positioning and SIDS: Positioning and SIDS. Pediatrics 89:1120-1126, 1992
- Clarren SK, Smith DW: Congenital deformities. Pediatr Clin North Am 24:665-677, 1977
- Clarren SK, Smith DW, Hanson JW: Helmet treatment for plagiocephaly and congenital muscular torticollis. J Pediatr 94:43-46, 1979
- Dias MS, Klein DM: Occipital plagiocephaly: Deformation or lambdoid synostosis? II. A unifying theory regarding pathogenesis. Pediatr Neurosurg 24:69-73, 1996
- Dias MS, Klein DM, Backstrom JW: Occipital plagiocephaly: Deformation or lambdoid synostosis? I. Morphometric analysis and results of unilateral lambdoid craniectomy. Pediatr Neurosurg 24:61-68, 1996
- Dingwall EJ: Artificial Cranial Deformation. London, England: John Bale, Sons & Danielsson, 1931
- Haberkern CM, Smith DW, Jones KL: The ‘breech head’ and its relevance. Am J Dis Child 133:154-156, 1979
- Hellbusch JL, Hellbusch LC, Bruneteau RJ: Active counter-positioning treatment of deformational occipital plagiocephaly. Nebr Med J 80:344-349, 1995
- Huang MH, Gruss JS, Clarren SK, et al: The differential diagnosis of posterior plagiocephaly: True lambdoid synostosis versus positional molding. Plast Reconstr Surg 98:765-774, 1996
- Hunt CE, Puczynski MS: Does supine sleeping cause asymmetric heads? Pediatrics 98:127-129, 1996
- Kane AA, Mitchell LE, Craven KP, et al: Observations on a recent increase in plagiocephaly without synostosis. Pediatrics 97:877-885, 1996
- Kawamoto HK: Torticollis versus plagiocephaly, in Marchac D (ed): Craniofacial Surgery: International Society for Craniomaxillofacial Surgery. New York: Springer-Verlag, 1987, pp 105-109
- Kelly KM, Littlefield TR, Pomatto JK, et al: Importance of early recognition and treatment of deformational plagiocephaly with orthotic cranioplasty. Cleft Palate Craniofac J 36:127-130, 1999
- Kriewall TJ: Structural, mechanical, and material properties of fetal cranial bone. Am J Obstet Gynecol 143:707-714, 1982
- Littlefield TR, Beals SP, Manwaring KH, et al: Treatment of craniofacial asymmetry with dynamic orthotic cranioplasty. J Craniofac Surg 9:11-19, 1998
- Littlefield TR, Kelly KM, Pomatto JK, et al: Multiple-birth infants at higher risk for development of deformational plagiocephaly. Pediatrics 103:565-569, 1999
- Muakkassa KF, Hoffman HJ, Hinton DR, et al: Lambdoid synostosis. Part 2: Review of cases managed at The Hospital for Sick Children 1972-1982. J Neurosurg 61:340-347, 1984
- Nichter LS, Persing JA, Horowitz JH, et al: External cranioplasty: Historical perspectives. Plast Reconstr Surg 77:325-332, 1986
- Pollack IF, Losken HW, Fasick P: Diagnosis and management of posterior plagiocephaly. Pediatrics 99:180-185, 1997
- Rekate HL: Diagnosis and management of plagiocephaly. BNI Quarterly 2:69-75, 1986
- Rekate HL: Occipital plagiocephaly: A critical review of the literature. J Neurosurg 89:24-30, 1998
- Ripley CE, Pomatto JK, Beals SP, et al: Treatment of positional plagiocephaly with dynamic orthotic cranioplasty. J Craniofac Surg 5:150-159, 1994
- Task Force on Infant Sleep Position and Sudden Infant Death Syndrome: Changing concepts of sudden infant death syndrome: Implications for infant sleeping environment and sleep position. American Academy of Pediatrics. Pediatrics 105:650-656, 2000
- Turk A, McCarthy JG, Thorne CH, et al: The “back to sleep campaign” and deformational plagiocephaly: Is there cause for concern? J Craniofac Surg 7:12-18, 1996
