Clinical Images: Type I Modic Changes Associated with Acquired Lumbar Spondylolisthesis After L4-L5 Microdiskectomy
A. Giancarlo Vishteh, MD
Iman Feiz-Erfan, BS
Volker K. H. Sonntag, MD
Division of Neurological Surgery, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
Key Words: lumbar sondylolisthesis, microdiskectomy
On T1-weighted magnetic resonance (MR) images, the signal intensity associated with Type I Modic changes along the vertebral bodies (parallel to the endplates) is decreased compared to normal. Conversely, these changes are manifested as high-intensity signals on T2-weighted MR images. The changes reflect the replacement of the normal marrow of the vertebral body by fibrovascular marrow. Because of the vascularity of fibrous marrow, Type I endplates enhance after the administration of MR contrast agents much like infections. Unlike Type I changes, however, an infected disk space demonstrates a high-intensity signal on T2-weighted MR images compared to the low-intensity signal associated with Type I Modic changes.
Type II marrow changes signify endplate disruption: yellow marrow replaces normal marrow. These changes are manifested as increased signal intensity on T1-weighted MR images and as isointense to slightly increased signal intensity on T2-weighted MR images. Type I changes can progress to Type II changes.
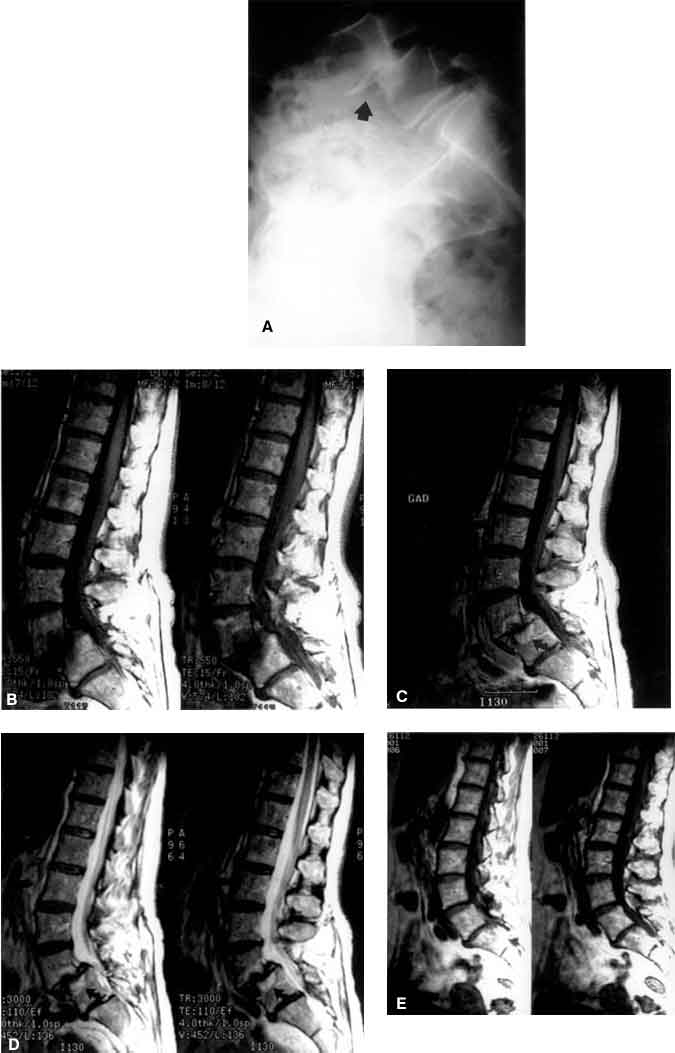
A 61-year-old female presented with signs and symptoms of lumbar radiculopathy refractory to conservative treatment. MR imaging of the lumbar spine revealed a herniated disk on the left at L4-L5. She underwent a left L4-L5 microdiskectomy and her symptoms resolved. Three years later she sought treatment for severe lower back pain. Radiographs revealed grade II spondylolisthesis (Panel A, arrow) at L4-L5. MR imaging revealed degenerative changes in the vicinity of the L4-L5 interspace as well as signal changes associated with the endplate and bone marrow. On T1-weighted images (Panel B) before and (Panel C) after contrast administration, enhancement was seen along the endplates and adjacent vertebral marrow (arrows). On T2-weighted images, these changes appeared as a high-intensity signal (Panel D, arrows). None of these changes were present on the patient’s original MR imaging study (Panel E). She underwent pedicle screw fixation from L4 to S1 for stabilization after undergoing decompressive laminectomy and foraminotomies. There was no surgical or histological evidence of infection.
On MR imaging, signal changes near adjacent endplates and vertebral bodies can signify degenerative disk changes along the spinal axis. When there is no clear evidence of pathology (i.e., disk herniation or spondylolisthesis), the presence of Modic changes near the disk space can signify chronic degeneration and micromotion, which could explain the presence of mechanical pain in the lower back.