
Patient Surgical Guide
The prospect of brain surgery or spine surgery can be a daunting one. We understand that you may feel scared and apprehensive as your surgery nears. On the other hand, many people also feel relieved and hopeful–and rightly so. You’ve made the decision to let us help you get better.
We’ve assembled this surgical guide to help you and those helping you with your treatment recognize, address, and prepare for the events that will happen before, during, and after your neurosurgical procedure.
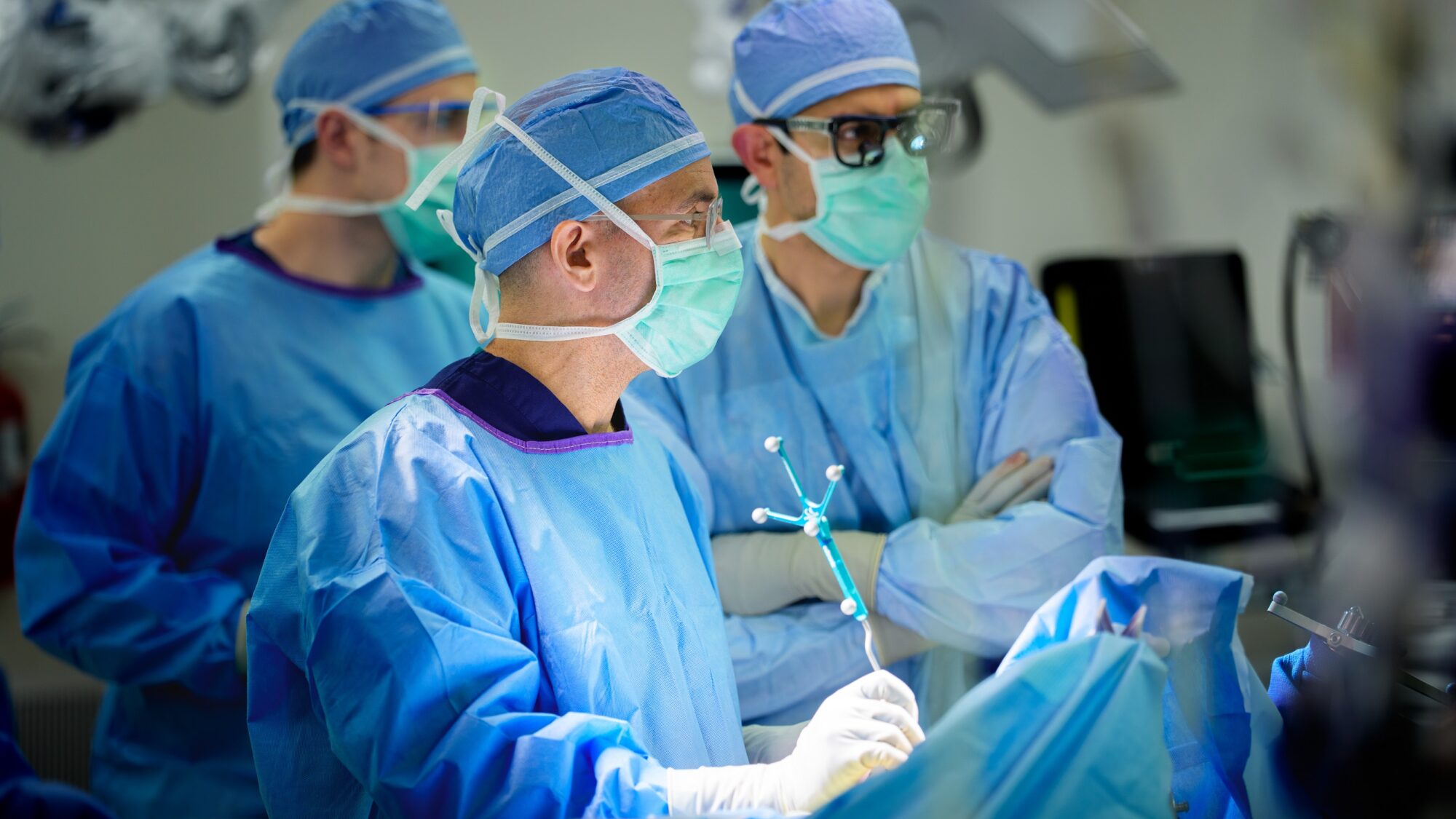
Important Phone Numbers
- Barrow Brain and Spine Appointments: (888) 779-0441
- St. Joseph’s Hospital Main Number: (602) 406-3000
- Registration: (602) 307-2305
- Preoperative Center: (602) 406-3192
- St. Joseph’s Hospital Concierge Services: (602) 406-3970
- St. Joseph’s Hospital McAuley Pharmacy (602) 406-3970
Before Surgery
Hospital Registration
Registration can be completed the morning of surgery or in advance by calling (602) 307-2305 or by visiting St. Joseph’s Hospital website.
Diet
In the weeks before your surgery, begin eating a balanced diet if you are not already doing so.
- Include protein and dairy in each meal.
- Eat 3-4 meals per day
Decrease your intake of alcohol, caffeine and cigarettes weeks or months prior to your surgery if possible. It is not recommended that you abruptly stop smoking days before surgery. Doing so can have an adverse affect on your breathing passages.
Medications
Notify your surgeon if you are currently taking the following medications:
- hypoglycemics (insulin or oral agents)
- anti-coagulants/anti-platelets such as Aspirin, Excedrin, Coumadin, Plavix, Heparin, Lovenox, etc.
- anticonvulsants (Depakote)
- anti-inflammatory drugs including Anaprox, Dolobid, Feldene, Motrin, Ibuprofen, Naprosyn, Toradol, Vioxx, Aleve, Advil, etc.
- natural supplements such as Vitamin E
- herbal medications such as gingko and St. John’s wort
Your surgeon may ask you to discontinue some medications before surgery because many of these substances contain ingredients that interfere with normal body functions and can increase the risks of complications during surgery.
Planning
Plan your discharge ahead of time:
- Identify a companion to help you for a few days after you arrive home.
- Arrange transportation to and from the hospital. Discharge usually takes place by 11:00 AM.
- Stock your refrigerator.
- Prepare meals in advance.
- Contact your insurance company to determine your benefits regarding outpatient therapy or medical devices such as walkers and shower chairs that you may need once you are home.

Preparation
Remove nail polish, jewelry, and body-piercing jewelry. Your surgeon may request that you take a shower with Chlorhexadine the night before and morning of surgery, from the neck down, giving special attention to the area of surgery. If you are scheduled for head or neck surgery, you may also be asked to shampoo your hair with your shampoo of choice when you shower as instructed above. Do not use hair spray, other styling products, lotions, or perfumes. Underarm deodorant may be used unless you are undergoing a thoracoscopic procedure for hyperhydrosis.Traditionally, patients are advised not to eat or drink at least eight hours prior to their surgical procedure. Please consult your surgeon for the restrictions that apply to your specific case. Specific guidelines are given to children based on their age, body weight, and time of surgery. Always remember to consult your surgeon for specific instructions.
Day of Surgery
Parking
The closest parking for surgical patients is in the 6th avenue garage. Additional parking may be available in the 3rd avenue garage. Upon request, hospital security will escort you to your car and may be available to shuttle you to and from nearby hotels. Valet services are available from 6:00 a.m. to 8:00 p.m. Fees for valet services as well as the parking garage are available at the hospital information desk.
Arrival
The morning of surgery you will arrive in the Preoperative Center at 5:00 a.m. (unless directed otherwise by your surgeon). This department is located on the 2nd floor of the neuroscience tower.
Do not bring the following items to the hospital:
- Unnecessary valuables or jewelry
- Medications from home. Hospital policy prohibits patients from receiving medication from outside the hospital for safety precautions.
Do bring the following to the hospital:
- complete list of medications that you take at home, including dosages and frequency
- insurance card and means to pay hospital co-payment
- identification
- living wills and advance directives
- test results
If you have had a chest x-ray within the last year, notify your surgeon to avoid unnecessary testing the morning of surgery. Also tell your physician if you have had an EKG (electrocardiogram) test completed within the last month. Your surgical team will want to see the results of this test. Give these documents to your surgeon’s office before surgery or bring them with you the morning of surgery.
If you have experienced any medical challenges such as cardiac, renal, or respiratory conditions, please make sure that your specialist is aware of your upcoming surgery. These physicians must “clear” you for surgery; that is, they must provide a written release stating that your condition does not prohibit you from undergoing surgery.
Preoperative Center Services
Once you are admitted to this department, various tests and examinations are performed:
- Blood is drawn unless you have been pretested or have copies of results from an outside laboratory.
- A nurse checks your vital signs (blood pressure, pulse, temperature). Procedures may be cancelled if you have a fever and other symptoms of illness.
Please notify your surgeon’s office if your temperature is higher than normal or if you have other symptoms of illness before the day of surgery. You may undergo x-rays, CT, or MRI studies before your procedure on the day of surgery or in the days leading up to it.
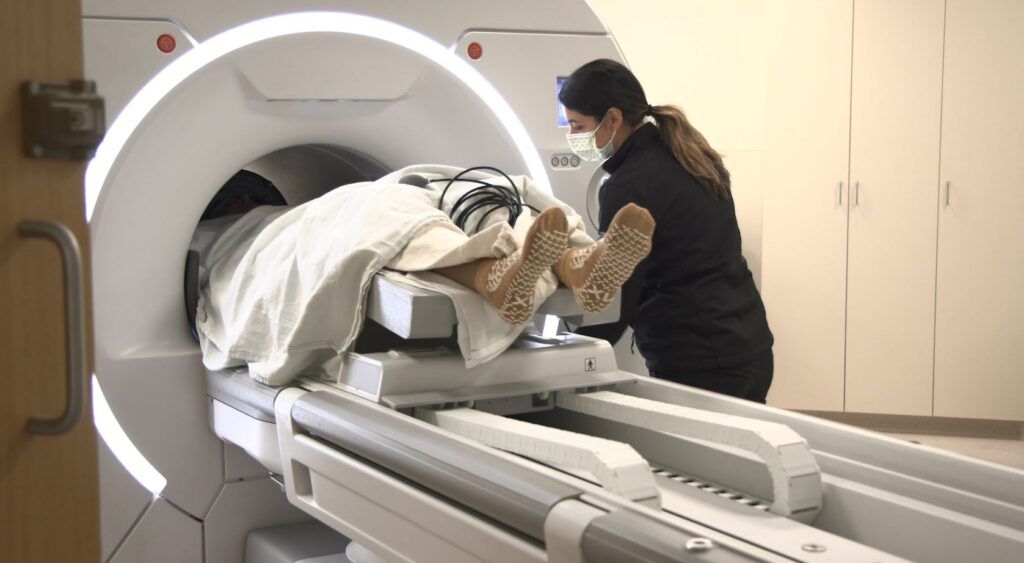
Preoperative Center Services
Once you are admitted to this department, various tests and examinations are performed:
- Blood is drawn unless you have been pretested or have copies of results from an outside laboratory.
- A nurse checks your vital signs (blood pressure, pulse, temperature). Procedures may be cancelled if you have a fever and other symptoms of illness.
Please notify your surgeon’s office if your temperature is higher than normal or if you have other symptoms of illness before the day of surgery. You may undergo x-rays, CT, or MRI studies before your procedure on the day of surgery or in the days leading up to it.
Before Surgery:
- You will change into a hospital gown.
- Your clothes will be given to your family.
- An identification bracelet will be placed on your arm. You will wear the bracelet until you are discharged from the hospital.
- You will be asked to sign registration and consent forms for your surgical procedure and for any tests, examinations, or consultations that your surgeon orders while you are in the hospital.
- You may be examined by a physician to assess your general health and to diagnose any unexpected illnesses.
- You will be asked to remove your eye glasses, contact lenses, and dentures. Your dentures may be placed back into your mouth in the recovery room when you are awake and alert.
- You will be asked to remove all jewelry.
- Hearing aids will not be removed until you have arrived at the operating room to ensure that you can communicate with the surgical team until you drift off to sleep.
Before Anesthesia:
- You and your family will be welcomed by your anesthesiologist and registered nurse from the operating room.
- You will have an opportunity to ask questions about the procedure and recovery process.
- An intravenous catheter may be placed in your arm to administer medication to relax you before you are taken to the operating room.
- The surgical site will be shaved if necessary once you are asleep in the operative suite. The amount of hair to be shaved is determined by the type of procedure and by your surgeon’s preference. For most cranial (head) surgeries, a small “strip” is shaved over the surgical site, rather than a full head shave.
During Surgery
While you are in surgery, your family may wait in the Neurosurgical Waiting Room. A hospital pager, which only functions on the hospital grounds, will be given to your family. The volunteer in this area will be notified if your family wishes to leave the premises in case a member of the surgical team wishes to speak with them. Personal cell phones can be used in this area if they are not analog phones that interfere with patient monitoring systems.
After the surgery is completed, a member of the surgical team will speak to your family. Children are welcome to visit once you have been admitted to the general nursing floor. Neurosurgical procedures tend to be longer than other procedures. The lengthy wait can be challenging for young children who require constant attention in the waiting room.
After Surgery
Your family will be notified once you are transferred to the recovery room from the operating room and again when you are to be transferred to your room. Visitors may be permitted in the recovery room at the discretion of the recovery room staff. You will remain in the recovery room for about an hour while you are waking up from anesthesia.
The nurses monitor your neurological status and vital signs. You will be asked to state your name and to answer other questions to assess your mental status. You will be connected to a cardiac monitor, pulse oximetry machine (measures the oxygen in your blood), temperature gauge, and oxygen mask. Pain medication is available to you as ordered by your surgeon. Our team is strongly committed to pain management. Please notify your nurse if your pain is not adequately addressed. Because many patients feel nauseated after a surgical procedure, medications are given in the recovery room to help prevent this unpleasant side effect.
You may have a variety of intravenous and arterial lines, which may remain in place for a few days or until hospital discharge. Flexible catheters may be used to drain surgical sites, the bladder, and brain fluid called cerebrospinal fluid (this tubing may be located in your lower back or top of your head). These drains may remain in place for as long as 4 days and are removed at the discretion of your surgical team.
Sequential compression stockings are placed on your legs to assist blood flow to your heart during surgery and while you are immobile. Surgical dressings depend on the procedure and surgeon. Many cranial (head) surgeries do not warrant a dressing. Rather the site is kept clean and may be treated with antibiotic ointment.
Medication may be ordered to control your pain and to assist in your recovery process. Please ask for this medication when you feel uncomfortable, especially during the first few days after surgery. If you wait until the pain is extraordinarily strong, the medication ordered by your doctor may not be able to control your pain. If you are concerned about becoming dependent on narcotics, please discuss this fear with your surgeon before surgery. Non-narcotic medication is available and is often sufficient to control pain.
Intensive Care Units (ICU)
The hospital has many different ICU(s). You will be assigned to a specific ICU when you enter the recovery room. ICU(s) are available to patients who require close monitoring such as those recovering from a surgical procedure or who are critically ill. In this department there is usually one nurse for every two patients. Visiting hours vary among the different ICUs. Flowers and live plants are not permitted in these areas. Please check with your unit for specific policies.
In the ICU you will be encouraged to increase your activity level as tolerated to help avoid complications associated with temporary immobility such as gas pains, bed sores, decreased lung capacity, and blood clots. You will be asked to reposition your body, to take deep breaths, and to use an incentive spirometer to flush anesthetic agents from your lungs. Showers are permitted after your surgeon provides a written order. Your nurse assesses your neurological status at predetermined times to ensure that you recover as expected. Your assessment includes being asked various questions to test your alertness. You also may be asked to move specific parts of your body.
Food and liquids are introduced slowly, beginning with ice chips and advancing to more substantial foods as tolerated. Tests such as radiographic studies (MRI, CT) and laboratory tests may be performed in the days after your surgery. At this point, you may need treatment to assist with your recovery such as speech, occupational, and physician therapy. These services may continue throughout your hospital stay and after hospital discharge in an outpatient setting. Social work, case management, and pastoral services are available on request.
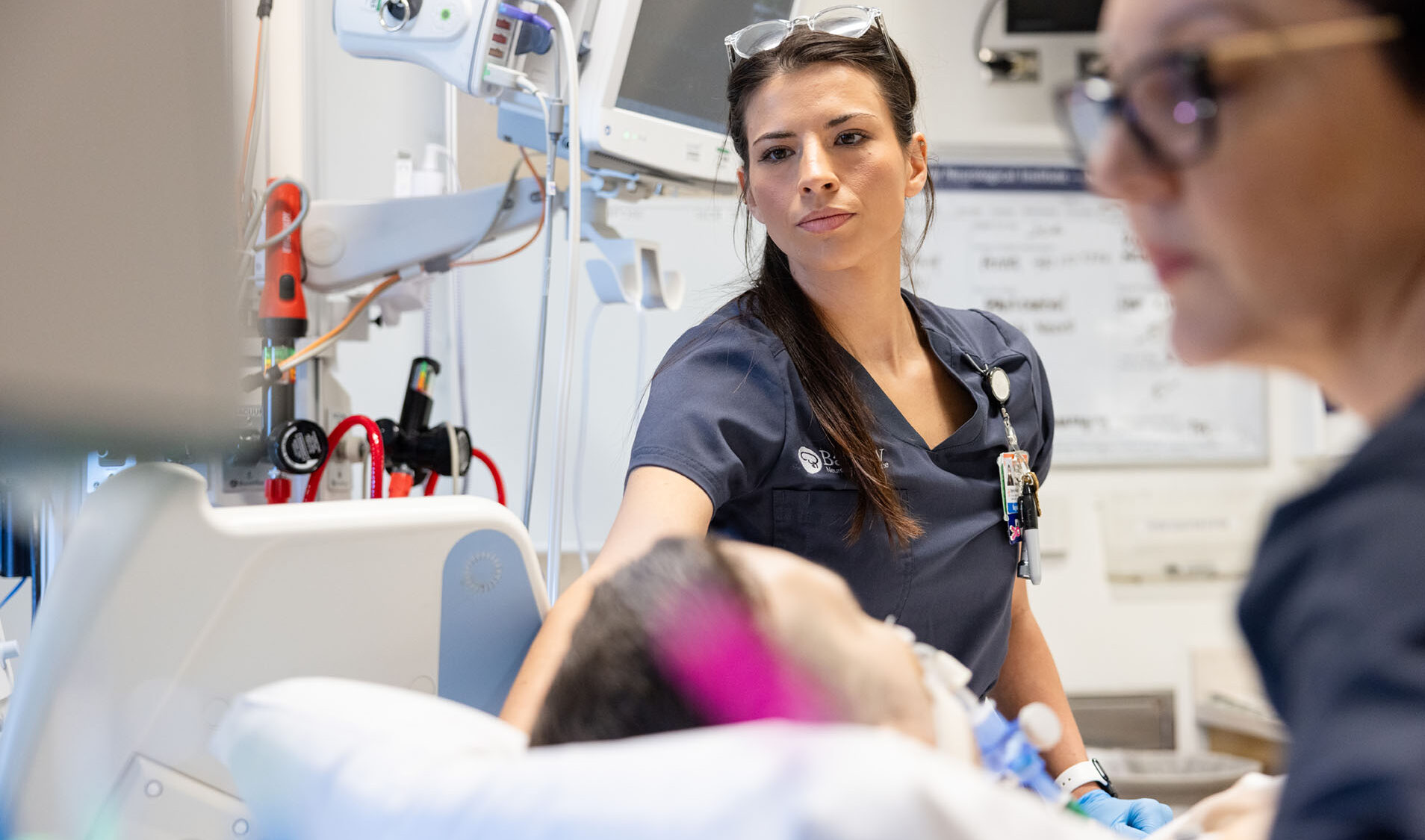
General Nursing Units
Once close monitoring is no longer required, you will be transferred to the general nursing floor. Private and double rooms are available in these areas.
On General Nursing Floors:
- Diet is advanced as tolerated. Small, frequent, balanced meals will help you heal faster and regain your normal energy level.
- Your activity will be increased to avoid muscle weakness and other complications of immobility. Some patients are out of bed the same day as surgery.
- Services such as physical therapy, speech therapy, and rehabilitation may be provided.
- As your level of activity increases, your discomfort may also increase.
- At this point pain, medication is usually taken orally rather than through an intravenous line.
Your Hospital Stay
The Barrow neuroscience inpatient tower is located on 3rd Avenue, just north of Thomas road in Phoenix. It is about a 20-minute cab ride from Sky Harbor Airport and about a 30-minute drive from Scottsdale’s private airport. In the event of a prolonged visit, air-conditioned Valley Metro buses make it easy for patients and families to travel around town.
Most outpatient services, including the Barrow physician offices, are located in buildings adjacent to the patient Neuroscience Tower. Visitors can park in the 3rd Avenue Garage or the 6th Avenue Garage, both located just a block north of Thomas Road and an easy walking distance from most inpatient and outpatient services. Trolleys and wheelchairs are available to patients and visitors who need help moving about the hospital campus.
Insurance
Although the hospital and the Barrow physicians accept most insurance, patients are advised to check with their insurance company before their visit to determine which hospital and professional diagnostic and treatment services will be covered. However, patients are advised to check with their treating physician’s office to verify insurance coverage. Patients who plan to receive elective services but who lack health insurance must make payment arrangements with the hospital and physician before treatment is provided. The physician’s billing office provides the necessary forms and hospital contact information.
Going Home
You will probably be discharged from the hospital by 11:00 a.m. If possible, you should arrange transportation before discharge. Prescriptions for pain control and other medications are provided at discharge. You may not feel that it is necessary to have these prescriptions filled right away, but it is important that your medications be available if the need arises. Discuss the possible interactions between various medications that you are taking with your physicians. Avoid drinking alcohol, driving, and operating heavy machinery while taking medication for pain.
Be mindful of your physical limitations. Allow sufficient time to recover before you resume normal daily activities. Ask your surgeon for specific limitations on lifting weight based on the procedure that you had. Exercise gradually with activities such as walking rather than aggressive gym activities. Discuss this process with your surgeon.
Baths and swimming are discouraged until your sutures are removed, typically 7 to 14 days after surgery. Wound care is prescribed by your surgeon.
Small frequent meals, including foods rich in protein, are encouraged to promote healing. Smoking inhibits the healing process by hindering blood flow to your organs and tissues and should be avoided.
The hospital’s case management department and social workers are available to help you identify needs that you may have after discharge from the hospital. These needs may range from renting wheelchairs to arranging home health care and outpatient therapies. Please ask to speak to one of these individuals before the day of discharge.
Remember to take all of your belongings with you and to tell your friends and family that you have been discharged from the hospital.
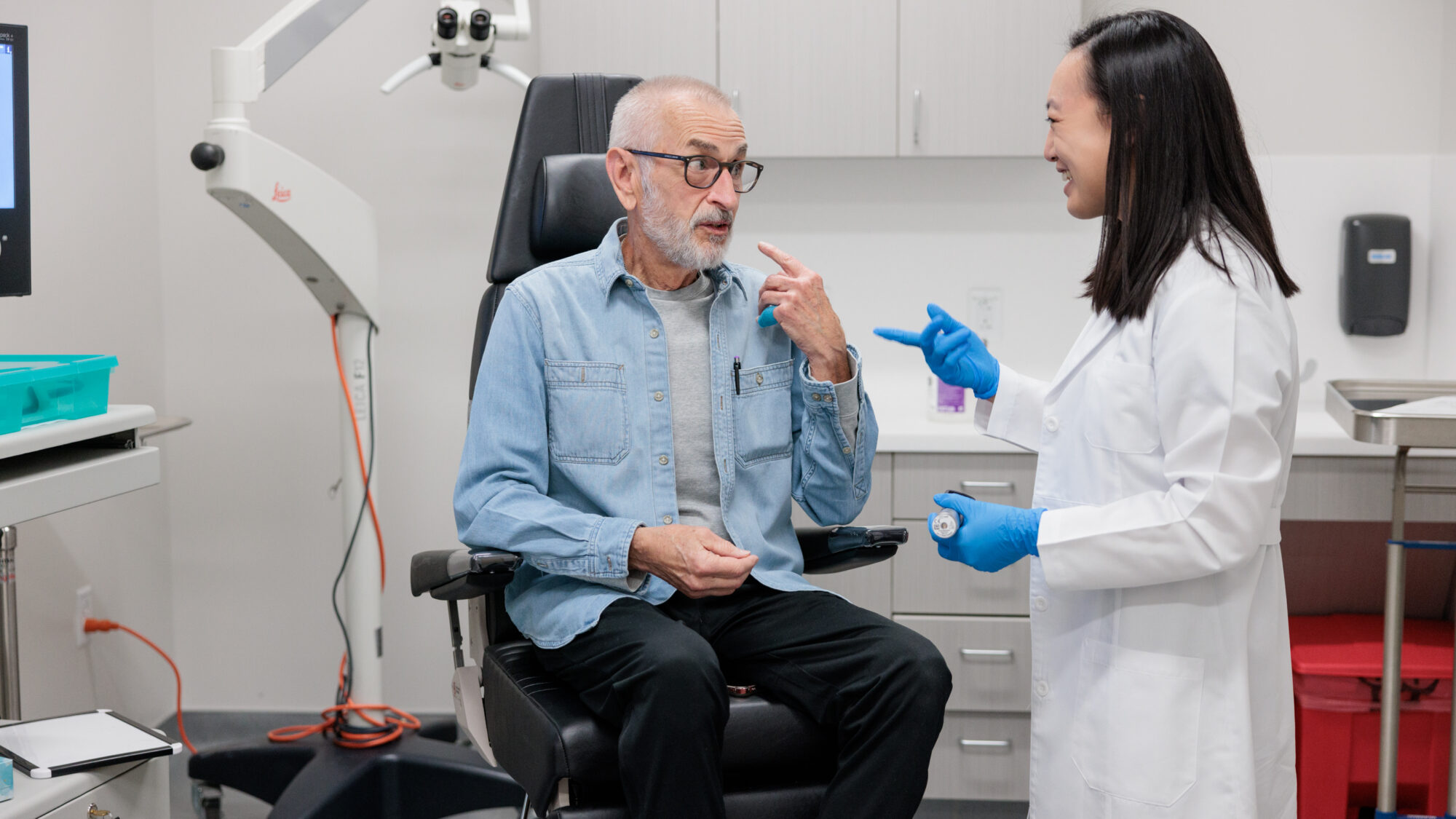
Follow Up With Your Doctor
On the day that you are cleared to go home from the hospital, be sure to call your surgeon’s office to schedule a follow-up appointment for 7-10 days after your surgery. This visit is an opportunity for your surgeon to examine your surgical site and to assess your recovery.
Before the appointment write down any questions you may have to ensure that all of your concerns are addressed. Special accommodations can be made for patients traveling from out of state. Write down any instructions that your physician gives you such as the need for an annual check-up, future x-rays, or other time-sensitive tests.
St. Joseph’s Hospital and Medical Center
Contacting Patients in the Hospital
Family and friends can call the hospital 24 hours a day at (602) 406-3000 to reach a patient who has been admitted. Because of governmental regulations, information about a patient’s condition can be shared with no one but direct relations (i.e., spouse, sibling, parent, or child) or other legally designated individuals. Patients can contact friends and family by phone from their room or via the Care Pages e-mail system provided by the hospital. Care Pages is a virtual “gathering place” that provides emotional support, patient updates, pictures and messages using a personal and secure program that is web-based.
Many patients choose to identify a contact person who can provide family and friends with updates about the patient’s condition. Several locations in the hospital have wireless internet access for family members and visitors to use.
Visiting Guidelines and Hours
Temporary Visitor Policies
Hospital patients will be allowed to have one support companion visit per day during limited visiting hours each day. This change excludes COVID-19 units. The support companion will receive a temperature check and screening upon arrival. They will be required to be masked throughout their visit.
Visitation hours are from 10:00 AM to 8:00 PM daily.
This policy will be reviewed and changed as COVID-19 conditions in the community change.
Patient Safety
In the interest of safety for our patients, anyone who has symptoms of a cold, including a runny nose, fever, sneezing, and coughing, should not visit hospitalized patients. If you wish to visit a patient while you have a respiratory illness, you are requested to discuss with the caregiver actions to reduce the risk to the hospitalized patient (hand hygiene and wearing a mask).
International Patients
The International Patient Program is committed to making your treatment at St. Joseph’s Hospital and Medical Center and Barrow Neurological Institute® as easy and stress-free as possible. While we offer significant expertise in neurology and neurosurgery, including Gamma Knife and CyberKnife radiosurgery treatment, we respect and value medical expertise in other parts of the world.
When a medical issue requires you to travel far from home, you might feel overwhelmed. Our first priority is to take away your stress—to go beyond your expectations to ensure that you and your family are comfortable and relaxed—so you can focus on your treatment and recovery. St. Joseph’s International Patient Program provides the highest level of service in a compassionate, discreet and respectful environment. The international team will serve as your personal guide to St. Joseph’s world-class medicine.
During your stay at St. Joseph’s, we will seamlessly blend your medical needs, individual preferences and cultural, linguistic and religious expectations into a tailored experience that makes St. Joseph’s feel as close to home as possible. Our team is here to help you before, during and after your treatment.
Our team can help you:
- schedule clinic appointments and diagnostic tests
- make hotel or lodging arrangements
- assist with hospital admission and insurance verification
- assist with financial estimates and payments
- communicate with hospital physicians and staff before and after your stay
- find a local worship/religious center

