
Hypophysitis
Overview
Hypophysitis is a rare inflammatory condition affecting the pituitary gland, which can lead to hormone deficiencies (hypopituitarism) and other related symptoms. The inflammation can cause the pituitary gland to enlarge and potentially compress nearby structures like the optic nerves. Numerous conditions can trigger hypophysitis. The two main types of hypophysitis include:
- Primary hypophysitis: Within primary hypophysitis, there are two subtypes: Lymphocytic hypophysitis and granulomatous hypophysitis. Lymphocytic hypophysitis is the more common form, often occurring during or just after pregnancy and often in tandem with other autoimmune disorders. Meanwhile, granulomatous hypophysitis is less common and is defined by clusters of immune cells forming granulomas, which can mimic tumors on imaging studies.
- Secondary hypophysitis: This type of hypophysitis occurs when an external factor, such as an infection, causes pituitary inflammation. Immune checkpoint inhibitor therapy like ipilimumab, nivolumab, and pembrolizumab can also cause secondary hypophysitis in cancer patients receiving immunotherapy.
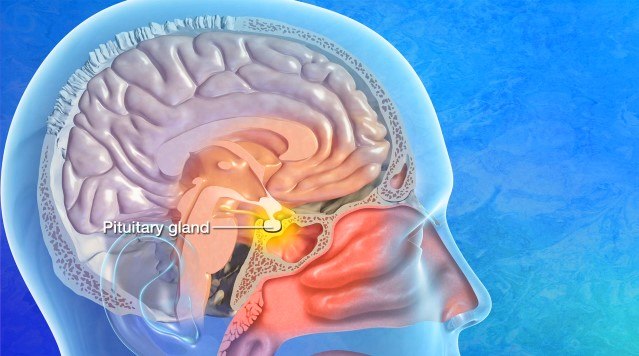
What causes hypophysitis?
Multiple conditions, like an autoimmune disorder, an infection, or even specific cancer treatments, can cause pituitary inflammation. The list of different hypophysitis causes can include:
- Autoimmune causes: As the most common cause, autoimmune cases develop when your immune system mistakenly attacks your pituitary gland. Lymphocytic hypophysitis is the most prevalent type of autoimmune hypophysitis, and it happens most often in women, especially during late pregnancy or just after giving birth.
- Cancer treatments: Some immune checkpoint inhibitors can also trigger hypophysitis as a side effect. Generally, these treatments boost the immune system to attack tumors. However, they can also attack healthy organs, including the pituitary gland.
- Cysts or tumors irritating the gland: Sometimes, a pituitary cyst or a benign tumor can leak fluid or become inflamed, triggering an immune reaction that inflames the pituitary gland.
- Infections or other illnesses: Rarely, a bacterial, fungal, or viral infection or a systemic disease, such as sarcoidosis or tuberculosis, can lead to hypophysitis. In these instances, the inflammation is secondary, meaning the infection comes first, then hypophysitis develops.
In some cases, doctors can’t find a cause for hypophysitis. This is called idiopathic hypophysitis.
Hypophysitis Symptoms
Hypophysitis symptoms can vary widely, depending on the inflammation present and which hormones are affected. Some symptoms come from “mass effect”—swelling of the pituitary gland that presses on nearby structures like the optic nerves—while others result from hormonal deficiencies caused by the damaged pituitary.
If you or someone you know has hypophysitis, you may experience a combination of the following symptoms:
- Headache: When the pituitary gland becomes inflamed, pressure increases in the small bony space at the base of the brain, producing headaches. These headaches are often centered behind the eyes or on the forehead and can feel dull and persistent.
- Vision problems: Pituitary gland swelling or a mass in the gland can press on the optic chiasm, where optic nerves cross. This affects peripheral vision, causing “tunnel vision.”
- Fatigue: Inflammation of the pituitary gland can lead to hypopituitarism that affects the hormone ACTH, which helps the body produce cortisol. When cortisol is low, exhaustion levels can quickly rise. Low thyroid hormone or low sex hormones can also cause fatigue.
- Nausea and vomiting: ACTH and cortisol regulate appetite and digestive symptoms. When their levels are low, the digestive system can become sluggish, leading to nausea or vomiting.
- Low blood pressure or dizziness, especially when standing: Maintaining normal blood pressure and fluid balance is also tied to cortisol levels, so when ACTH is low, blood pressure can drop and lead to dizziness or fainting, especially when standing up.
- Unexplained weight changes: Weight gain or loss that happens without a change in diet or activity level can be caused by low thyroid hormone, low ACTH and low cortisol, or adrenal insufficiency. Low estrogen or testosterone can also cause weight gain, especially around the belly.
- Mood and cognitive changes: An unshakeable brain fog, not being able to concentrate, or experiencing prolonged bouts of feeling down or periods of depression are often linked to low thyroid, low ACTH and low cortisol, or sex hormones.
- Cold intolerance: Feeling unusually cold or often needing extra layers outside of seasonally cold weather can be a symptom of low thyroid hormone.
- Irregular or missing periods: The pituitary glands make LH and FSH, hormones that control the ovaries. If these hormones drop, they disrupt the menstrual cycle, causing irregular periods or their total disappearance.
- Loss of libido or sexual dysfunction: Low LH and FSH also lower estrogen or testosterone levels, which affects libido, sexual function, and fertility in both women and men.
- Poor growth in children: If the pituitary gland isn’t making enough growth hormone (GH), children may grow more slowly or not reach their expected height. GH deficiency can also affect energy and body composition in adults.
- Increased urination and thirst: When the posterior part of the pituitary gland is affected, arginine vasopressin (AVP) deficiency (diabetes insipidus) can develop. This condition causes the body to struggle to hold onto water. It produces intense thirst and the need to urinate frequently, and if not managed, can lead to dehydration.
If you experience one or more of these symptoms, a healthcare professional must evaluate you. Early detection and treatment can prevent complications and improve outcomes.
Hypophysitis Diagnosis
Doctors typically diagnose hypophysitis by the symptoms experienced, hormonal blood tests showing pituitary dysfunction, MRI findings that suggest inflammation rather than a tumor, and whether or not you have a clinical history of autoimmune disease or immunotherapy use.
Diagnosing hypophysitis can be challenging because it often mimics other pituitary conditions. Often, a pituitary biopsy can confirm the condition.
Physicians may use the following exams and imaging tests to diagnose hypophysitis:
- Physical and neurological exam: First, your healthcare provider will ask specific questions about the type of symptoms you experienced, such as your energy levels, any vision or weight changes, menstrual history, and sexual function, as well as a history of cancer treatment, infections, autoimmune diseases, and pregnancy or postpartum history. Next, they’ll complete an examination to assess your neurological function, including reflexes, coordination, strength, and sensation.
- Magnetic Resonance Imaging (MRI): An MRI provides detailed images of the pituitary gland and its surrounding structures. In the case of hypophysitis, an MRI is highly effective at distinguishing inflammation, structural damage, or soft tissue characteristics of tumors and evaluating the size and shape of the pituitary gland and stalk.
- Blood tests: Blood tests are crucial in determining if your pituitary gland is underproducing hormones. Tests typically include ACTH and cortisol, TSH and free T4, LH, FSH, estradiol, testosterone, IGF-1, prolactin, and electrolyte levels. Low levels in multiple hormone systems raise suspicion of hypophysitis.
- Biopsy: In uncertain or severe hypophysitis cases, your doctor may suggest a biopsy. A biopsy establishes an exact diagnosis by removing a small tissue sample to confirm inflammation in a pathology laboratory. There, pathologists examine the tissue under a microscope to determine the type of cells present and other essential characteristics that may guide treatment decisions.
Depending on your symptoms and results, your doctor may also request visual field testing to determine if a possible pituitary tumor has damaged optic nerves and caused vision problems. Antibody testing to check for other autoimmune markers and AVP deficiency testing may also help.

Hypophysitis Treatment
Treatment for hypophysitis depends on the cause, severity, and how much it affects your hormone production or nearby structures like the optic nerves. Neuro-endocrinologists can usually manage hypophysitis without surgery, but it may be necessary in specific situations.
Nonsurgical Treatments
Nonsurgical treatments are the primary treatment for hypophysitis. Doctors treat most patients successfully with corticosteroids or hormone replacement therapy tailored to their specific hormone deficiencies.
- Hormone replacement therapy: Hormone replacement therapy can treat a range of hormone deficiencies to help stabilize your symptoms and prevent dangerous complications. These hormones can include hydrocortisone or prednisone for ACTH and cortisol, levothyroxine for thyroid hormone, estrogen and progesterone or testosterone for sex hormones, and desmopressin in the event of diabetes insipidus.
- High-dose glucocorticoids: Glucocorticoids are often the first treatment to reduce inflammation in autoimmune or immunotherapy-related hypophysitis. Prednisone and methylprednisolone are commonly prescribed in these cases and can improve pituitary gland swelling and changes to vision. Often, hormone deficiencies do not fully recover in immune-related hypophysitis, so long-term hormone replacement therapy is standard.
- Immunosuppressive therapy: In resistant or relapsing autoimmune cases, medications like azathioprine, methotrexate, or rituximab may be considered. This treatment is likely when hypophysitis is part of a larger autoimmune condition.
- Observation: When hypophysitis symptoms are mild and hormone levels are near normal, doctors may monitor the condition with repeat MRIs and blood tests.
Surgical Treatments
Generally, surgery is not helpful for hypophysitis because most types of hypophysitis are inflammatory rather than tumor-related, and doctors can treat the condition through hormone replacement therapy or high-dose corticosteroids.
However, if therapies don’t work, your symptoms worsen, severe pressure on the optic nerves causes vision loss, or your diagnosis remains uncertain, your doctor might consult a neurosurgeon. Deciding on surgical treatment depends on the type of hypophysitis, its location, and its impact on surrounding tissues, but most often, it includes a transsphenoidal approach done through the nose.
- Transsphenoidal surgery: The most common surgical approach for a pituitary tumor is transsphenoidal surgery. In this procedure, a neurosurgeon reaches and removes a tumor through the nasal passages and the sphenoid sinus using a small surgical instrument and an endoscope. Transsphenoidal surgery leaves no scar, minimizes the risk of complications, and offers a faster recovery.
One Central Location with Multiple Treatment Options
At Barrow Neurological Institute’s renowned Pituitary Center, we treat people with pituitary tumors and disorders in one robust location. And because our doctors and nurses treat more people with pituitary disorders than any other team in the Southwest U.S., you can rest assured that you’ll be in very experienced hands.
Common Questions
How common is hypophysitis?
Hypophysitis is a rare condition, although its recognition has increased in recent years due to the increasing use of immune checkpoint inhibitors in cancer therapy.
Historically, hypophysitis has been considered extremely rare, with an estimated incidence of 1 in 9 million people per year, but recent studies suggest this may be an underestimation.
Who gets hypophysitis?
Primary hypophysitis, or when the immune system attacks the pituitary gland, most commonly affects women between the ages of 20 and 40, often occurring during late pregnancy or in the postpartum period.
Secondary hypophysitis, or inflammation of the pituitary gland due to another disease, tends to occur equally in both sexes and usually in middle-aged to older adults. It is typically associated with systemic illnesses like tuberculosis or sarcoidosis.
Finally, drug-induced hypophysitis, which is common in cancer patients treated with immune checkpoint inhibitors, is slightly more prevalent in males and can happen at any age, depending on when cancer treatment begins.
What is the prognosis for someone with hypophysitis?
The prognosis for someone with hypophysitis typically depends on the underlying cause, how early it’s treated, and whether there’s lasting damage to the pituitary gland.
When appropriately treated, life expectancy and quality of life remain normal. Most people recover with a combination of hormone replacement and medication.
Beyond an early diagnosis and proper treatment, factors that can improve your prognosis include:
- Mild or partial hormone deficiencies at the time of diagnosis
- Good response to corticosteroids, mainly when caused by an autoimmune disorder
- No compression of nearby structures like the optic nerves
That said, some people will experience permanent loss of pituitary function and may require lifelong hormone therapy.
Can hypophysitis be prevented?
In most cases, hypophysitis can’t be prevented, especially when the condition is related to autoimmune disorders or necessary cancer treatments. Early recognition and close monitoring—especially in high-risk groups—remain key in improving outcomes and limiting permanent pituitary damage.
Pay attention to symptoms like unexplained fatigue, visual changes, or irregular menstrual periods, as prompt treatment with steroids or hormone replacements can minimize long-term complications. And if you’re receiving immunotherapy as a cancer treatment or you have an autoimmune disease, routine hormone testing can identify any problems before they worsen.



