
Lumbar Spinal Stenosis
Overview
Lumbar spinal stenosis, commonly referred to simply as lumbar stenosis, describes the narrowing of spaces within the spinal canal in the lower back. The spinal canal is made up of bones called vertebrae, which protect the spinal cord.
The lumbar spine consists of five vertebrae between the ribs and the pelvis. When the spinal canal narrows, it can put pressure on the segment of spinal nerves called the cauda equina. This may cause pain in the back or legs and bladder retention (problems with emptying your bladder completely).
People with lumbar spinal stenosis may walk in a stooped-over posture and feel better when leaning on a grocery cart. Another common sign of lumbar stenosis is feeling the need to stop walking because of pain in the legs or back, which is relieved by rest. This is also known as neurogenic claudication.
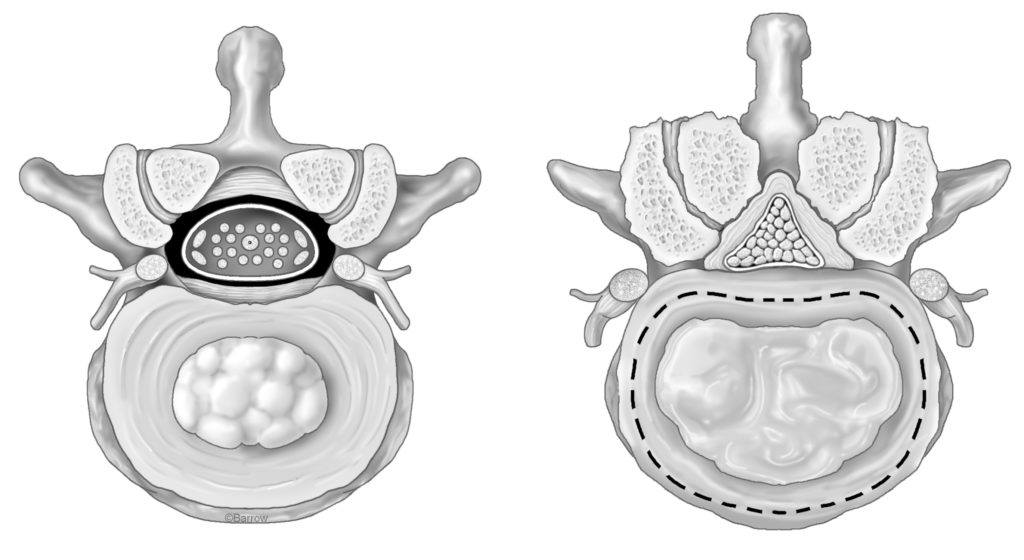
Spinal stenosis is common, present in over 50% of people over 60 years old. It is caused by wear-and-tear, arthritis of the joints, and thickening of the ligamentum flavum—a short, thick ligament that connects two vertebrae to each other. These changes usually occur gradually as you age.
Intervertebral discs, which provide a cushion between the vertebrae and enable movement in the spine, become less spongy with age. This can lead the bulging of hardened discs into the spinal canal (herniated discs), bone overgrowth (bone spurs), and thickening of ligaments—all of which can contribute to narrowing within the spinal canal.
Lumbar Stenosis Symptoms
Symptoms of lumbar stenosis usually appear gradually and may worsen over time. Some people may not notice any symptoms at all. Symptoms can include:
- Aching or burning feeling starting in the buttocks and radiating down into one leg or both legs (sciatic nerve pain)
- Symptoms of neuropathy or numbness in the feet
- Bowel and bladder dysfunction (in severe cases)
- Cramping in calves while walking (neurogenic claudication)
- Difficulty walking long distances without rest (neurogenic claudication)
- Lower back pain
- Pain in the back or legs that worsens with walking/standing and improves with bending forward or sitting (positive grocery cart sign)
- Weakness or numbness in the legs, feet, and/or buttocks
- Weakness in the foot that causes the foot to slap down when walking, known as “foot drop.” This can also present when people report catching their toes on the ground or carpet.
When to Contact a Physician Immediately
The following can be signs of damage to the nerves in and around your lumbar spine and should be addressed by a physician immediately:
- Abrupt onset of bowel or bladder incontinence
- Abrupt onset of a foot drop: inability to lift your foot or tap repeatedly while keeping your heel on the ground while sitting
- Unrelenting pain or inability to walk
Lumbar Stenosis Treatments
Conservative, Non-surgical Treatments for Lumbar Stenosis
Surgical treatment is the most definitive way to correct the narrowing of the spinal canal, but conservative treatments may help relieve pain and other symptoms. Conservative treatments for lumbar stenosis include:
- Anti-inflammatory medications to reduce swelling around nerves and relieve pain
- Epidural steroid injections to reduce swelling and relieve pain
- Physical therapy to stabilize the spine and increase strength and flexibility
Most insurance companies require you attempt physical therapy and epidural steroid injections within 12 months before they will approve a surgical procedure to correct lumbar stenosis. If you do not respond to these conservative therapies, and your pain is no longer tolerable, you may be a candidate for surgery.
Things to Consider before Lumbar Stenosis Surgery
Your doctor will also consider your overall health before recommending surgery. Some factors that can increase the risk of complications from spine surgery include:
- Obesity (body mass index greater than 35)
- Diabetes
- Smoking
- History of multiple medical problems
Although these risk factors do not automatically disqualify you for surgery, you should try to minimize them while you consider surgery.
Fortunately, with current technology, age is no longer a contraindication for surgery. People who are into their late 80s are still good candidates for surgery, assuming they are relatively healthy.
Surgical Options for Lumbar Stenosis
The most common surgical procedure for spinal stenosis is decompressive laminectomy, in which the roof at least one vertebra is removed to create more space for the affected nerves.
This procedure can frequently be accomplished using minimally invasive techniques, in which the muscles of the back are spread apart rather than cut.
Minimally invasive spine surgery reduces scar tissue, blood loss, recovery time, and pain.
A foraminotomy is performed during the same operation as the decompressive laminectomy. In this procedure, the holes through which the nerves exit the spine are widened. Some patients find it helpful to visualize this process as a “roto-rooter” around the spinal nerves.
Most patients can return to normal activity within three months after surgery, enjoying their favorite activities such as walking, golf, running, hiking, and anything that involves bending at the waist and lower back.
Some patients with spinal stenosis need stabilization in addition to the laminectomy. This procedure is known as spinal fusion surgery. Spinal fusion involves joining two or more vertebrae with screws and rods and may be recommended in some cases if spinal instability is present.
As with decompressive laminectomy and foraminotomy, spinal fusion can frequently be accomplished using minimally invasive techniques.
Common Questions
How common is lumbar stenosis?
Spinal stenosis is common. Almost 50% of those over the age of 65 have some form of spinal stenosis. The lumbar spine is the most common location for spinal stenosis to occur.
Who gets lumbar stenosis?
Because lumbar stenosis is most often caused by degenerative changes in the spine, it usually affects people over the age of 50. However, younger people may be at risk if they have any of the following conditions:
- Paget’s disease
- Rheumatoid arthritis
- Spinal deformity, such as scoliosis or being born with a narrow spinal canal
- Spinal injury
- Spinal tumor
How is lumbar stenosis diagnosed?
In addition to reviewing your medical history and performing a physical examination, your doctor may order one or more of the following imaging tests to diagnose lumbar stenosis:
- Computed tomography (CT)
- Electromyography (EMG)
- Magnetic resonance imaging (MRI)
- Myelogram
- X-ray



