
Scoliosis and Spinal Deformities
Warning: Undefined property: Em_Condition::$page in /nas/content/live/barrowneuroorg/wp-content/themes/barrow-2020/functions/em-post/class-em-condition.php on line 93
Warning: Attempt to read property "ID" on null in /nas/content/live/barrowneuroorg/wp-content/themes/barrow-2020/functions/em-post/class-em-condition.php on line 93
Warning: Undefined property: Em_Condition::$page in /nas/content/live/barrowneuroorg/wp-content/themes/barrow-2020/functions/em-post/class-em-condition.php on line 94
Warning: Attempt to read property "ID" on null in /nas/content/live/barrowneuroorg/wp-content/themes/barrow-2020/functions/em-post/class-em-condition.php on line 94
At a Glance
- Scoliosis is an abnormal sideways curvature of the spine.
- The exact cause is often unknown, but risk may be higher with a family history of scoliosis or conditions affecting the spine or muscles.
- In children, scoliosis usually develops during the growth spurt around puberty.
- In adults, scoliosis is more likely to cause back pain, stiffness, or fatigue.
- Many cases—especially mild scoliosis—do not require surgery and can be managed with monitoring and conservative treatment.
Overview
Scoliosis is a condition in which the spine curves sideways instead of remaining straight. When viewed from the front or back, a healthy spine appears straight. In people with scoliosis, the spine curves to the left or right and may form a “C” or “S” shape.
Experts classify scoliosis as a three-dimensional spinal deformity, meaning the spine may also rotate as it curves. Doctors diagnose scoliosis when a spinal curve measures 10 degrees or greater on an X-ray, using a measurement called the Cobb angle.
Many people with scoliosis have mild curves that cause few symptoms. In more severe cases, scoliosis can lead to changes in posture, pain, reduced mobility, or—in rare cases—breathing problems if the rib cage is affected.
Types of Scoliosis
Idiopathic Scoliosis
Idiopathic scoliosis accounts for about 80% of all cases. The exact cause is unknown, but genetics may play a role.
This form most commonly develops in adolescents between ages 9 and 15, often during growth spurts. Contrary to popular myths, poor posture or carrying heavy backpacks are not risk factors for scoliosis.
Degenerative Scoliosis
Degenerative scoliosis develops in older adults as the spine changes with age. Arthritis, disc degeneration, and other forms of spinal wear can lead to a gradual spinal curve.
This type is often associated with back pain, stiffness, or fatigue.
Congenital Scoliosis
Congenital scoliosis occurs when the vertebrae do not form properly before birth. Although present at birth, the spinal curve may become more noticeable as a child grows.
Neuromuscular Scoliosis
Neuromuscular scoliosis develops as a result of conditions that affect the nerves or muscles that support the spine, such as:
- Cerebral palsy
- Muscular dystrophy
- Spina bifida
- Spinal cord injury
Muscle weakness or imbalance allows the spine to gradually curve.
Secondary Scoliosis
In rare cases, scoliosis can develop after spinal trauma, infection, tumors, or other structural abnormalities affecting the spine.
Causes and Risk Factors
The causes of scoliosis vary depending on the type. In many cases—particularly idiopathic scoliosis—the exact cause is unknown. Researchers believe it may involve a combination of genetic, developmental, and biomechanical factors.
Risk factors include:
- Spinal injury or trauma
- Family history of scoliosis
- Rapid growth during adolescence
- Congenital spine abnormalities
- Neuromuscular conditions
- Age-related spinal degeneration
Symptoms
Symptoms depend on the severity of the curve and the patient’s age.
Symptoms in Children and Adolescents
Children with scoliosis often experience visible changes in posture rather than pain. Signs may include:
- Uneven shoulders
- One shoulder blade that sticks out more than the other
- Uneven hips or waistline
- Leaning slightly to one side
- Uneven rib cage
- Arms that hang unevenly when standing straight
These changes are often first noticed during school screenings or routine pediatric exams.
Symptoms in Adults
Adults with scoliosis are more likely to experience symptoms related to spinal degeneration or nerve compression, including:
- Back or neck pain
- Muscle fatigue
- Stiffness and reduced flexibility
- Difficulty bending or twisting
- Changes in posture or balance
- One leg appearing shorter than the other
- Numbness or weakness if nerves are compressed
- Pain that radiates down the leg (sciatica)
In rare and severe cases, spinal nerve compression can cause bowel or bladder problems, which require urgent medical evaluation.

Diagnosis
Doctors diagnose scoliosis using a physical exam and imaging tests.
- Medical history and neurological exam: Your healthcare provider will ask about symptoms, family history, and any underlying medical conditions.
- Physical examination: A common screening method is the Adams forward bend test, in which the patient bends forward while the provider looks for spinal asymmetry.
- X-Ray: X-rays confirm the diagnosis and allow doctors to measure the Cobb angle, which determines the severity of the spinal curve.
- Additional imaging: Your doctor may recommend additional imaging under some circumstances, including CT scans to evaluate bone structure and MRI scans to assess nerves and soft tissues.
Scoliosis Severity
Doctors classify scoliosis based on the Cobb angle:
| Severity | Cobb Angle |
|---|---|
| Mild | 10–24° |
| Moderate | 25–39° |
| Severe | 40° or greater |
Treatment recommendations depend on curve severity and whether the spine is still growing.
Treatment
Treatment depends on several factors, including:
- Age
- Curve severity
- Type of scoliosis
- Risk of progression
Many people with scoliosis live active, healthy lives with minimal treatment.
Non-Surgical Treatment
Observation
Neurosurgeons often monitor mild scoliosis with regular follow-up visits and periodic X-rays, particularly in children who are still growing.
Physical Therapy and Exercise
Exercise and physical therapy may help:
- Strengthen muscles that support the spine
- Improve posture
- Reduce discomfort
Bracing
Bracing can be beneficial for adolescents with curves between 25 and 40 degrees who are still growing.
Braces do not correct the curve but can help prevent it from worsening. People typically wear them for 16–23 hours per day until growth is complete.
Pain Management
Your care team may treat your pain with:
- Over-the-counter medications such as acetaminophen or ibuprofen
- Physical therapy
- Occasionally corticosteroid injections
Complementary Therapies
Some patients benefit from therapies such as:
- Massage therapy
- Acupuncture
- Yoga or Pilates
These approaches may improve flexibility and reduce muscle tension.
Surgical Treatment
Your doctor might recommend spinal neurosurgery when:
- The spinal curve is greater than 40–50 degrees
- The curve continues to worsen
- Symptoms such as significant pain or breathing problems occur
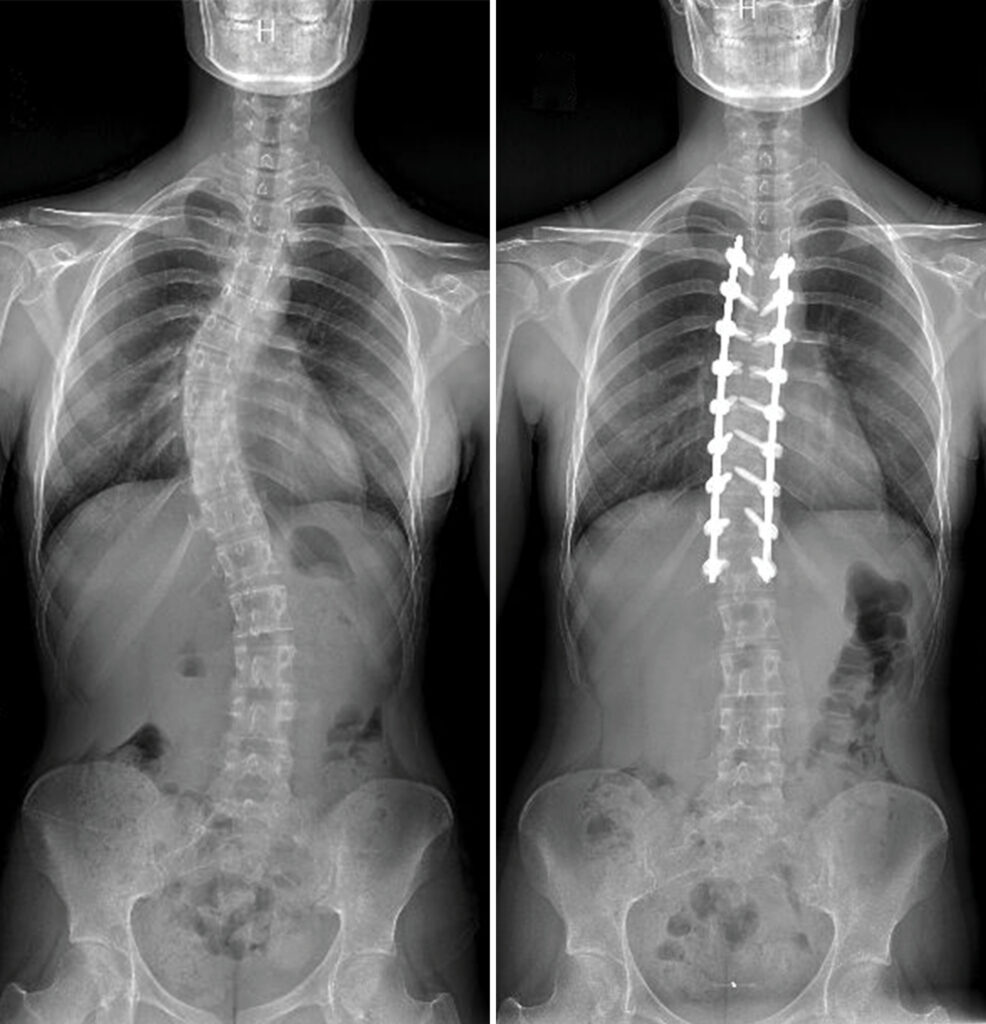
Spinal Fusion
Spinal fusion is the most common surgery for scoliosis. During this procedure, a neurosurgeon fuses two or more vertebrae using bone grafts and metal rods, screws, or hooks to stabilize the spine.
Growing Rods
Neurosurgeons sometimes use growing rods in children with severe scoliosis who are still growing. The rods are periodically lengthened to allow spinal growth while controlling the curve.
Vertebral Body Tethering (VBT)
VBT is a newer surgical technique that uses a flexible cord attached to screws along the spine to guide growth and gradually correct the curve
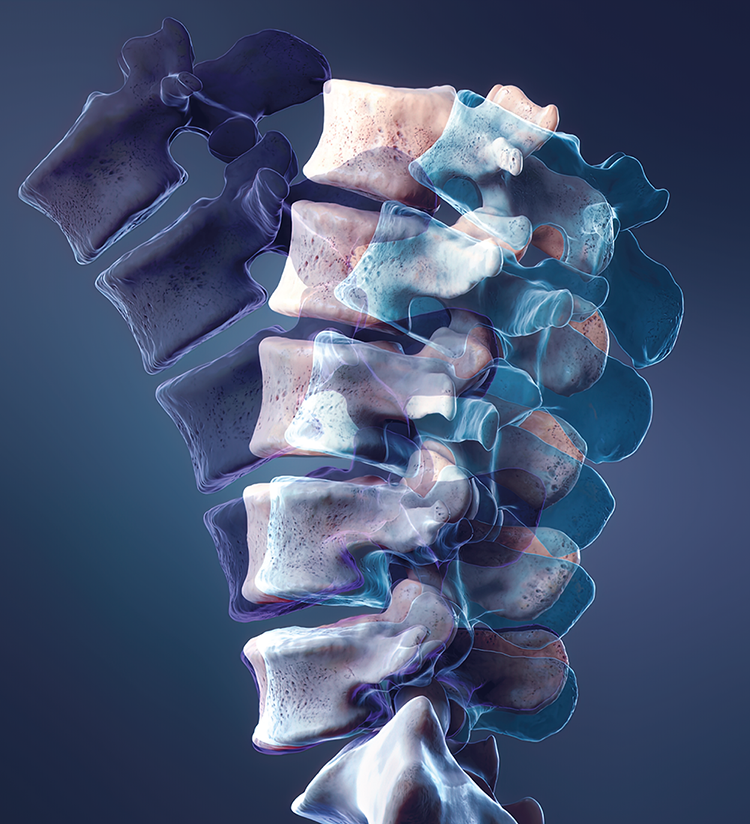
Outlook
The outlook for scoliosis depends on the severity of the curve and how early it is detected.
- Mild to moderate scoliosis: Often causes few long-term problems.
- Severe scoliosis: May lead to pain, posture changes, or breathing problems if untreated.
With early diagnosis and appropriate treatment, most people with scoliosis can lead full and active lives.
Prevention
Most cases of scoliosis—especially idiopathic scoliosis—cannot be prevented. However, maintaining good spinal health may help reduce complications.
This includes:
- Regular pediatric checkups
- Early scoliosis screening
- Maintaining a healthy weight
- Staying physically active
- Strengthening core muscles
- Avoiding smoking
Early detection allows healthcare providers to monitor the spine and intervene if the curve progresses. Treatment recommendations depend on curve severity and whether the spine is still growing.
Common Questions
How Common is Scoliosis?
Scoliosis affects about 2%-3% of the population, or roughly one in every 30-50 people.
In the United States, an estimated six to nine million people have scoliosis.
Adolescent idiopathic scoliosis is the most common form and is usually diagnosed between the ages of 9 and 15. Although boys and girls develop scoliosis at similar rates, girls are more likely to develop curves that require treatment.
Who gets scoliosis?
Idiopathic scoliosis is the most common type of scoliosis, and it tends to appear during an adolescent growth spurt, between ages 9 and 15.
Although scoliosis occurs at about the same rate for girls and boys, girls are more likely to have a severe spine curvature that requires some form of treatment. In fact, girls are eight times more likely to have a curve that progresses to the point where treatment is needed, leading scientists to posit whether the hormone estrogen plays a role.
Although idiopathic scoliosis can run in families, most children with scoliosis have no family history of the disease. Less common types of scoliosis may be caused by congenital disabilities, injuries, certain infections, tumors, or neuromuscular conditions, like cerebral palsy or muscular dystrophy.
Can scoliosis be prevented?
While scoliosis can’t be prevented, numerous steps can help manage or reduce the risk of scoliosis progression, depending on the type of scoliosis you’ve been diagnosed with. They include:
- Idiopathic scoliosis: Although this subtype has no clear cause, early detection through school screenings or routine physical exams can help monitor your spine’s curvature and make way for intervention treatments, like bracing, to prevent further progression.
- Congenital scoliosis: While congenital scoliosis is caused by abnormalities that develop before birth, it can be managed with early medical interventions to prevent the condition from worsening.
- Neuromuscular scoliosis: When scoliosis develops due to muscular dystrophy, cerebral palsy, or other neuromuscular disorders, managing the underlying condition with physical therapy and medical care can help slow its progression.
- Degenerative scoliosis: To reduce your risk of spinal degeneration due to age, it’s helpful to maintain a healthy weight to place less strain on your spine, exercise regularly and strengthen the core muscles that support your spine, practice good posture, avoid activities that put undue stress on your spine, and avoid smoking, as it can accelerate spinal disc degeneration.
Participating in contact sports or wearing gear like heavy backpacks doesn’t cause scoliosis. However, they can contribute to back or shoulder pain.
There are no guaranteed ways to prevent scoliosis, but maintaining good spinal health, seeking early detection, and implementing the appropriate interventions can greatly reduce the risk of progression.






