
Biomechanical Analysis of Cranial Settling After Transoral Odontoidectomy
Sait Naderi, MD*
Neil R. Crawford, PhD
M. Stephen Melton, BS
Volker K.H. Sonntag, MD
Curtis A. Dickman, MD
Division of Neurological Surgery, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
*Current Address: Dokuz Eylül University Hospital, Department of Neurosurgery, Balcova, Izmir, Turkey
Abstract
We conducted a biomechanical study to determine whether C1-ring integrity is important in maintaining the normal separation between the occiput and C2, specifically when the C1 anterior arch is transected to provide access to the dens during an odontoidectomy procedure. Six human cadaveric occiput-C3 specimens were loaded under axial compression, and the bilateral horizontal separation of the C1 lateral masses and the vertical compression of the occiput relative to C2 were recorded. Specimens were first studied after odontoidectomy without C1-ring transection, then after C1 anterior arch transection, and finally after C1 lamina transection. With applied compressive load corresponding to three times the weight of the head, the C1 ring spread horizontally 1.57 mm ± 0.30 mm more when the anterior arch of C1 was transected than when left intact, resulting in 0.74 mm ± 0.44 mm collapse in the vertical separation between the occiput and C2. After laminar transection, the C1 ring spread 6.55 mm ± 2.29 mm more than when it was intact. The resultant vertical separation was a 3.37 mm ± 1.89 mm collapse in the occiput-C2. All changes in C1 spreading and the occiput-C2 collapse were statistically significant (p<0.05, paired Student’s t-tests). Continuity of the C1 ring prevents horizontal spreading caused by the wedging of C1 between the occiput and C2 and thus prevents cranial settling. To prevent the subsequent development of disease related to cranial settling, we recommend that surgeons resect part of C1 if necessary during odontoidectomy but avoid transecting C1.
Key Words: craniovertebral junction, dens, lateral mass offset, odontoidectomy
When they affect the craniovertebral junction (CVJ), various diseases such as rheumatoid arthritis, achondroplasia, Paget’s disease, congenital anomalies, and trauma can require spinal decompression surgery to be performed via a transoral odontoidectomy.
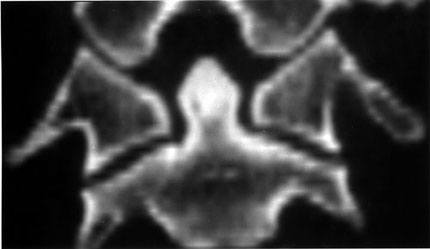
Results from clinical and in vitro studies have shown that an odontoidectomy creates a severe ligamentous instability.4,5 However, based on the bony morphology of the CVJ (Fig. 1) and the fact that the ring of C1 is often transected anteriorly to provide access to the dens, there also appears to be the potential for osseous instability of the CVJ after an odontoidectomy. The angled joint interfaces between the occiput-C1 and C1-C2 cause the C1 lateral masses to act as wedge spacers between the occiput and C2 and provide the means for transfer of compressive force outward radially to the ring of C1. Normally, this radial force should be inconsequential. Analysis of preliminary research, however, has indicated that with even a single break in the continuity of the C1 ring, the lateral force transferred from axial compression can cause the C1 ring to spread, allowing the occiput to migrate caudally toward C2 (i.e., cranial settling). Neurosurgeons are concerned with this biomechanical response to compression because gravitational effects on the head and muscle contraction cause axial compression to be the main mode of loading at the CVJ in the upright neutral position.
Spreading of C1 and subsequent cranial settling can cause serious complications. A decrease in the height of the upper cervical spine complex can cause the spinal cord to kink or fold within the spinal canal. This kinking may be associated with tethering of the spinal cord and medulla due to tension on the dentate ligaments15 and may explain some cases of deterioration after odontoidectomy or other upper cervical spine surgeries.1,7 Increased offset of the C1 lateral mass can also cause torsion of the vertebral arteries, which can contribute to neurological degradation.8,16
Although anterior transection of the ring of C1 during odontoidectomy is a common procedure, there is an alternative odontoidectomy procedure in which the anteroinferior C1 arch is partially resected to gain access to the dens.14 The ring of C1, however, is not disrupted. Whether this technique prevents C1 ring spreading or cranial settling is unknown.
To our knowledge, no studies have focused specifically on how the C1 ring contributes to the stability of the CVJ. This study therefore investigated the importance of the integrity of the C1 ring in maintaining the normal separation between the occiput and C2 in vitro. First, we examined whether an odontoidectomy that leaves the C1 ring mostly intact allows less vertical migration to occur than when the C1 anterior arch is transected. We also examined whether subsequent disruption of the C1 lamina further destabilizes the CVJ.
Materials and Methods
Cadaver Preparation
Seven human upper cervical spines (the occiput-C3) were obtained en bloc during routine autopsy procedures. Of these, one specimen (obtained from an 18-year-old male cadaver) was excluded because a congenital cleft in the posterior tubercle of C1 was found. The specimens, then, consisted of five males and one female (mean age at time of death, 63.8 years; range, 53 to 77 years). Examination of clinical reports and radiological studies revealed no disease affecting the bone and joint structure of the CVJ. These specimens had been used in a previous study to compare the biomechanical effects of different instrumentation methods after odontoidectomy-induced instability of the upper cervical spine.11 After this previous study, the specimens were mostly devoid of soft tissues, but the ring of C1 was continuous, and the atlantoaxial joint surfaces were intact. Because the current study was focused on bone deformation, the condition of the soft tissues was unimportant. Specimens were stored at -20°C and thawed in a saline solution at 25°C on the day of testing.
Biomechanical Testing
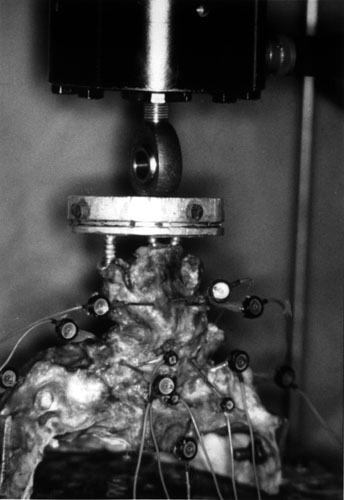
The C3 vertebra was potted in a cylindrical, aluminum, loading fixture in which wood screws were embedded in methylmethacrylate to provide a flat surface for loading. The skull base was inverted and affixed to the base of the loading apparatus by using an angle vise. The specimen was oriented in a position that directed gravitational preload axially along its neutral orientation. Specimens were tested mechanically with the skull base attached rigidly to the base of the apparatus while loads were applied to C3 (Fig. 2).
Because the primary loading modality used to induce cranial settling is axial compression, this is the loading mode we chose to study. Other loading modalities, such as loads that induce bending or twisting, would also be expected to induce horizontal spreading of C1 (especially during flexion). However, these loads and angular motions were not studied because their contribution specifically to cranial settling would be difficult to quantify and the response to these other modalities would be governed by a combination of osseous and ligamentous resistance rather than purely osseous resistance.
By using a servohydraulic test machine (Fig. 2), axial forces were applied to C3 through a nonfixed rounded interface. Three preconditioning cycles were applied where loads of 120 N were held for 60 sec. After allowing 60 sec for creep, data were recorded while loads were applied quasistatically between 0 and 120 N in 20-N increments. Each loading increment was held for 45 sec. A 40-N load was chosen to approximate the weight of the human head, and a 120-N load was used to approximate loads that might be present during muscle contraction.
During loading, three-dimensional spinal movement was measured using an optical tracking system (Optotrak 3020; Northern Digital, Waterloo, Ontario, Canada). Infrared-emitting diodes were rigidly attached to the ends of 1.25-mm end-threaded stainless steel surgical guide wires that had been inserted in three locations in the skull base and in three locations in the C2 vertebral body and cut to an average of 4 cm. Three infrared-emitting diodes were similarly attached to the left lateral mass of C1, as well as to the right lateral mass of C1 to track the two halves separately as two rigid bodies. By using a digitizing probe (an accessory to the Optotrak system), a Cartesian coordinate system was established at each spinal level with respect to its neutral orientation.2 The positive x-axis was oriented medially to left laterally, the positive y-axis caudally to cranially, and the positive z-axis posteriorly to anteriorly.
The linear displacement of a point on the medial midheight left lateral mass of C1 was established with the digitizing probe and tracked relative to the right lateral mass of C1. The digitizing probe was also used to identify a point on the anteroinferior margin of the foramen magnum and to track this point relative to C2. The results were given in terms of the C1 coordinate system.
All specimens were tested in three phases: (1) after an odontoidectomy procedure in which the entire odontoid process and the transverse ligament were removed and at least 50% of the inferior portion of the C1 anterior arch was left intact (that is, the control phase in which transections of C1 were not performed),14 (2) after transection of the C1 anterior arch to simulate the more radical odontoidectomy technique,3 and (3) after transection of the C1 lamina.
Statistical Analysis
In each phase of testing, we measured the linear vertical motion of the occiput relative to C2 and the offset of the C1 lateral masses. These results were analyzed using one-tailed paired Student’s t-tests to determine whether significantly more motion was present after transection. In all cases, p values less than 0.05 were considered statistically significant.
Results
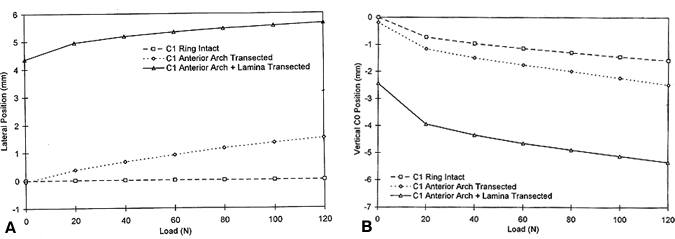
After transection of the anterior C1 arch, applied loads moderately increased the spreading of the C1 ring (Fig. 3). Subsequent transection of the lamina increased the spreading of the ring even more when loads were applied. The increases in ring spreading after one and two transections corresponded to moderate and large increases in vertical migration of the occiput relative to C2 (Fig. 3).

When compared at normal head weight (Fig. 4A, Table 1) and at maximum load (approximately three times the head weight; Fig. 4B, Table 1), the increases in both horizontal spreading and vertical compression from intact ring to anterior transection and from anterior transection to anterior and posterior transection were statistically significant (p <0.05).
 Both lateral spreading of the C1 ring and vertical compression demonstrated moderately linear responses after the first loading step, indicating constant stiffness (Fig. 3). With the ring of C1 intact, the mean stiffness of horizontal ring spreading was extreme (1600 ± 930 N/mm). The stiffness of vertical compression across the occiput-C2 was 130 ± 28 N/mm. After anterior transection of the C1 arch, the mean stiffness of horizontal ring spreading decreased significantly to 118 ± 33 N/mm. The mean stiffness of vertical compression decreased significantly to 82 ± 25 N/mm. Values for vertical and horizontal stiffness were significantly lower after anterior transection than those obtained when the ring was intact. After transection of the lamina, the stiffness of vertical compression changed little, averaging 82 ± 12 N/mm. After transection of the lamina, the stiffness of horizontal spreading increased significantly to a mean of 210 ± 67 N/mm.
Both lateral spreading of the C1 ring and vertical compression demonstrated moderately linear responses after the first loading step, indicating constant stiffness (Fig. 3). With the ring of C1 intact, the mean stiffness of horizontal ring spreading was extreme (1600 ± 930 N/mm). The stiffness of vertical compression across the occiput-C2 was 130 ± 28 N/mm. After anterior transection of the C1 arch, the mean stiffness of horizontal ring spreading decreased significantly to 118 ± 33 N/mm. The mean stiffness of vertical compression decreased significantly to 82 ± 25 N/mm. Values for vertical and horizontal stiffness were significantly lower after anterior transection than those obtained when the ring was intact. After transection of the lamina, the stiffness of vertical compression changed little, averaging 82 ± 12 N/mm. After transection of the lamina, the stiffness of horizontal spreading increased significantly to a mean of 210 ± 67 N/mm.
Discussion
C1 Wedge Behavior
The occurrence of the statistically significant C1 bilateral offset after C1 anterior arch transection and a further offset after C1 lamina transection can be understood by examining the coronal geometry and anatomy of the CVJ (Fig. 1). In the coronal plane, the occiput-C2 complex has an X-like configuration. Unlike the subaxial spine, the upper cervical spine does not possess intervertebral discs. Therefore, if the neck posture is such that the posterior arch of C1 does not make contact with the skull base or the C2 posterior elements, the entire compressive load across C1 is supported by the C1 lateral masses. The lateral force transferred from compression must be borne by the anterior and posterior arches of C1 and, likely to a lesser extent, by the transverse ligament. An odontoidectomy in which the C1 anterior arch is transected and the odontoid process and transverse ligament are removed destroys two of these three load-bearing horizontal structures. The posterior arch of C1, which has a thin cross-sectional area, must then alone resist the lateral force that vertical compression exerts.
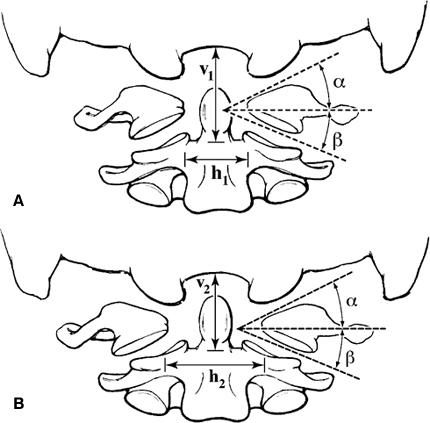
It is possible to estimate the lateral force and the potential increase in lateral mass offset distance (Fig. 5). This geometrical analysis has two angles of interest: the atlanto-occipital angle, a , which is 27.5° on average,13 and the atlantoaxial angle, b , which is 20.0° on average.5 Dimensions of interest are the increase in the lateral mass offset, D h , and the increased compression across occiput-C2, D v . These four terms are related by the following equation:
Dv = (Dh/2)(tan a + tan b)
For the average values of a and b, Dv = 0.44 Dh. For example, the increase in vertical compression across occiput-C2 would be 0.88 mm for horizontal C1 ring spreading of 2 mm.
In the six specimens studied, the joint angles average from direct goniometrical measurements were a = 31.8° and b = 22.7°. For the measured horizontal spreading of 1.56 mm at full compression, the predicted vertical compression increase was 0.81 mm, which is reasonably close to the observed mean of 0.70 mm. After transection of both the anterior and posterior arches of C1, the predicted increase in vertical compression for the measured horizontal spreading of 6.55 mm was 3.40 mm, which agrees well with the observed mean value of 3.37 mm.
Clinically, these angles and dimensions can be estimated by examining radiographs or computed tomographic scans. For a given amount of C1 lateral mass offset, combined a and b angles that are greater than normal predict greater than normal wedging action with greater potential vertical translation across the occiput-C2. For example, if both a and b are 5° greater than average, vertical translation for 2 mm of horizontal C1 ring spreading should be 1.10 mm instead of the previous value of 0.88 mm.
C1 Laminectomy
The increase in C1 lateral mass offset permitted a significant concomitant increase in vertical compression across the occiput-C2 after odontoidectomy in which the C1 anterior arch was transected and a further increase in vertical compression after C1 lamina transection. As the integrity of the C1 ring decreased, vertical compression increased. This further increase reflected the left and right halves of C1 becoming completely independent masses, the motions of which were limited only by the remaining soft tissues. The stiffness of ring spreading increased because the posterior tubercle could no longer act as a pivot point for the ring spreading. Instead of swinging open like a mouth, the separation of the two halves was more linear.
Clinical Recommendations
The integrity of the C1 ring should be considered during preoperative planning for a transoral odontoidectomy, particularly in patients who have undergone a prior C1 laminectomy. In such cases, surgeons should try to avoid complete transection of the anterior arch of C1. Congenital anomalies that interfere with C1 integrity, such as that found in the specimen with the cleft posterior tubercle excluded from this study, can be diagnosed easily by computerized tomography of the CVJ or other radiographic means.6 Surgeons should inspect radiographs carefully for any anomaly that could affect the integrity of C1.
After odontoidectomy, fusion can be performed by using a variety of occipitocervical plate and rod constructs9 or transarticular screw fixation techniques combined with C1-C2 tension-band techniques.10 When the anterior arch of C1 has been transected, the center of rotation for the mouthing action, which occurs when C1 spreads, is near the region in which posterior hardware would be applied. Hence, posterior fixation would be expected to provide little resistance against separation of the C1 lateral mass and would stabilize only the posterior column. Theoretically, in such a case, C1 spreading and cranial settling could still occur by the same mechanism even after fixation. Transarticular screw fixation would most likely be the preferred procedure because the buttress created by transarticular screws should limit horizontal translation of the lateral masses and concomitant vertical migration. Further research is needed regarding the best method for obtaining fixation in patients who have undergone odontoidectomy with and without C1 transection.
In planning an odontoidectomy followed by transarticular screw fixation, surgeons should also consider a nonbiomechanical issue. When transarticular screws are inserted, the C1 anterior arch is typically used to establish the drill trajectory from a lateral fluoroscopic radiograph. If the C1 anterior arch is removed during odontoidectomy, the location of the anterior arch must be estimated or an alternate landmark must be used. This point should further motivate surgeons to perform an odontoidectomy that spares the anterior C1 arch when placing transarticular screws.
Study Limitations
This study did not investigate the contribution of muscles to the stability of the CVJ. As described by Panjabi,12 however, muscles are an important part of the spine stabilizing system. The presence of active muscles surrounding C1 would probably have prevented some spreading of C1 and thus some vertical compression. Furthermore, no instrumentation systems were tested to determine the best method for fixating C1. Although different devices have been tested to determine their performance during bending and rotation, the devices have not been compared in terms of their ability to prevent spreading of the C1 ring. Finally, the optoelectronically measured changes in the occiput-C2 separation were not correlated to radiographically measured changes. Therefore, how precisely clinicians can measure in patients the C1 spreading and cranial settling quantified in this study is unknown.
Conclusions
The integrity of the C1 ring is critical to the stability of the CVJ. When the C1 ring is transected, the lateral masses displace laterally, causing cranial settling and overt spinal instability. The structural and mechanical abnormalities create a high risk of neurological sequelae. When possible, the C1 ring should be resected only partially during an odontoidectomy. Transection should be avoided. When the C1 anterior arch must be transected, transarticular screw fixation or occipitocervical fixation is recommended.
From Naderi S, Crawford NR, Melton MS, Sonntag VKH, Dickman CA: Biomechanical analysis of cranial settling after transoral odontoidectomy. Neurosurg Focus 6:Article 7, 1999. Adapted with permission from Neurosurgical Focus.
References
- Boden SD, Dodge LD, Bohlman HH, et al: Rheumatoid arthritis of the cervical spine. A long-term analysis with predictors of paralysis and recovery. J Bone Joint Surg Am 75:1282-1297, 1993
- Crawford NR, Dickman CA: Construction of local vertebral coordinate systems using a digitizing probe. Technical note. Spine 22:559-563, 1997
- Crockard HA, Pozo JL, Ransford AO, et al: Transoral decompression and posterior fusion for rheumatoid atlanto-axial subluxation. J Bone Joint Surg Br 68:350-356, 1986
- Dickman CA, Crawford NR, Brantley AGU, et al: Biomechanical effects of transoral odontoidectomy. Neurosurgery 36:1146-1153, 1995
- Dickman CA, Locantro J, Fessler RG: The influence of transoral odontoid resection on stability of the craniovertebral junction. J Neurosurg 77:525-530, 1992
- Dorne HL, Just N, Lander PH: CT recognition of anomalies of the posterior arch of the atlas vertebra: Differentiation from fracture. AJNR 7:176-177, 1986
- Fielding JW, Tuul A, Hawkins RJ: “Ondine’s curse.” A complication of upper cervical-spine surgery. J Bone Joint Surg Am 57:1000-1001, 1975
- Jones MW, Kaufmann JCE: Vertebrobasilar artery insufficiency in rheumatoid atlantoaxial subluxation. J Neurol Neurosurg Psychiatry 39:122-128, 1976
- Klein G, Vaccaro AR, Kramer DL, et al: Instrumentation for occipitocervical fusion. Semin Spine Surg 9:227-232, 1997
- Marcotte P, Dickman CA, Sonntag VKH, et al: Posterior atlantoaxial facet screw fixation. J Neurosurg 79:234-237, 1993
- Naderi S, Crawford NR, Song GS, et al: Biomechanical comparison of C1-C2 posterior fixations. Cable, graft, and screw combinations. Spine 23:1946-1956, 1998
- Panjabi MM: The stabilizing system of the spine. Part I. Function, dysfunction, adaptation, and enhancement. J Spinal Disord 5:383-389, 1992
- Smoker WRK: Craniovertebral junction: Normal anatomy, craniometry, and congenital anomalies. Radiographics 14:255-277, 1994
- Spetzler RF, Dickman CA, Sonntag VKH: The transoral approach to the anterior cervical spine. Contemp Neurosurg 13:1-6, 1991
- Stoltmann HF, Blackwood W: An anatomical study of the role of the dentate ligaments in the cervical spinal canal. J Neurosurg 24:43-46, 1966
- Webb FW, Hickman JA, Brew DS: Death from vertebral artery thrombosis in rheumatoid arthritis. Br Med J 2:537-538, 1968
