
Cervical Myelopathy from Dilated Epidural Veins: Case Report of Intracranial Outflow Obstruction Treated with a Sigmoid Sinus-to-Internal Jugular Vein Bypass
Authors
Arnold B. Vardiman, MD*
Curtis A. Dickman, MD
Robert F. Spetzler, MD
Joseph E. Heiserman, MD†
B. Gregory Thompson, MD‡
*Texas Neuroscience Institute, Department of Neurosurgery, San Antonio, Texas, Division of Neurological Surgery
† Division of Neuroradiology, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
‡Department of Neurosurgery, University of Utah Medical Center, Salt Lake City, Utah
Abstract
A 36-year-old hydrocephalic male became symptomatic with progressive cervical myelopathy caused by dilated epidural veins compressing the ventral surface of the upper cervical spinal cord. The veins were collaterals from the internal jugular veins, which were occluded bilaterally. The obstruction to venous outflow was treated with a sigmoid sinus-to-internal jugular vein bypass. The obstruction accounted for both the hydrocephalus and the myelopathy. The pathophysiology and treatment of this unique problem are reviewed.
Key Words : bypass, epidural veins, jugular vein, myelopathy, saphenous vein graft, sigmoid sinus
Symptomatic spinal cord compression caused by dilated epidural veins has rarely been reported.3 This article presents a patient whose spinal cord was compressed by dilated epidural venous collaterals. The dilation was the result of bilateral occlusion of the internal jugular veins.
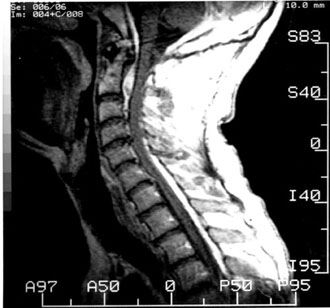
Figure 1. T1-weighted, gadolinium-enhanced magnetic resonance image.
A 36-year-old, right-handed male presented with a long history of hydrocephalus, cerebral palsy, and unstable left hemiparesis. He also had a 6-year history of insidious, progressive quadriparesis. He had undergone multiple shunt revisions but had never had a ventriculoatrial shunt placed. During these 6 years, his condition had deteriorated from his needing a cane to needing a walker and, finally, to needing a wheelchair. His motor function, particularly the fine motor skills of his right hand, had deteriorated gradually, exacerbating his left hemiparesis.
Examination
Motor examination revealed a dense left hemiparesis. Abduction of the left arm was limited and painful due to contractures. He was capable of limited coarse movements of the left hand but only with great effort. The strength of his left lower extremity was 3/5. The right upper and lower extremities could overcome some resistance (4/5), but the fine motor movement of his right hand was diminished. Bilaterally, pin prick sensation below the level of the nipple was slightly decreased. Joint position sense was impaired on the left but intact in the right lower extremity. He was hyperreflexic, somewhat more on the left than on the right. He exhibited bilateral Hoffmann’s signs, Babinski signs, and sustained clonus. At presentation, he was confined to a wheelchair. He retained bowel and bladder function. He was mildly dysarthric as a result of his cerebral palsy; however, his cranial nerve examination was normal.
Magnetic resonance (MR) imaging revealed an extradural mass with a high-intensity signal ventral to the cervical spinal cord. The mass extended from the occipitocervical junction down to the level of C4 (Fig. 1). No flow voids were present. Postmyelography computed tomography (CT) confirmed the presence of the mass (Fig. 2).
First Operation
The patient underwent a modified anterolateral retropharyngeal approach so the upper cervical spine could be accessed. A left-sided approach was chosen to avoid the shunt catheter within his right neck. A midline corpectomy of the inferior half of C2 and the entire body of C3 was performed.
After the vertebrectomy was completed, profuse bleeding from the epidural venous plexus was encountered. The bleeding was controlled with Gelfoam® (Upjohn, Kalamazoo, MI), but further access to the epidural space was precluded by the rapid blood loss. After hemostasis was obtained, an autologous iliac crest bone graft was harvested and fitted into the corpectomy defect.
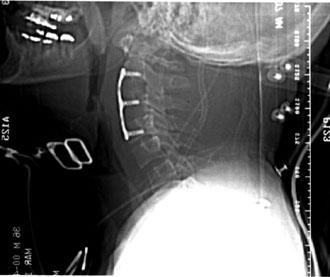
A Synthes (Synthes Spine, Paoli, PA) locking plate spanning C2-C4 was placed, and the wound was closed over a Jackson Pratt drain (Fig. 3). The patient’s intraoperative somatosensory evoked potentials were stable. Intraoperative fluoroscopy confirmed appropriate placement of the graft and plate. Analysis of a biopsy specimen revealed nondiagnostic fibrous tissue.
Postoperative Course
Upon waking, the only neurological deficit exhibited by the patient was the expected left hypoglossal palsy. MR angiography revealed complete bilateral obstruction of the internal jugular veins just caudal to the jugular bulb. The venous outflow was reconstituted through the epidural venous plexus and confirmed by conventional arteriography (Fig. 4). Detailed venography of the superior vena cava and external jugular system was performed to search for venous pathology in the neck and to identify recipient vessels for a bypass.
The patient underwent a sigmoid sinus-to-internal jugular vein bypass with a saphenous vein interposition graft 8 days after the first operation. The patient was placed in the supine position with his head turned to the left and secured in position with the Mayfield (Codman, Raynham, MA) headholder. The patient’s right suboccipital area and right neck were prepared, and his right thigh and leg were prepared for the saphenous vein harvest.
A linear retroauricular incision was extended vertically to the mastoid tip. The suboccipital musculature was reflected off the subocciput to expose the junction of the temporal mastoid and occipital bones. The asterion was identified; the mastoid emissary vein followed its usual course through that point. After the bony landmarks were identified, the courses of the transverse and sigmoid sinuses and their junction were plotted. The Midas Rex® (Midas Rex Pneumatic Tools, Inc., Fort Worth, TX) drill was used to skeletonize the sinuses and the junction, thereby exposing the pre- and retrosigmoid dura.
Next, a hockey-stick incision was made along the anterior border of the sternocleidomastoid muscle arcing posterosuperiorly toward the mastoid process. The initial plan to use the external jugular vein as the recipient for the graft was aborted when only a small atretic vessel was found. Anterior and medial to the sternocleidomastoid muscle was a robust internal jugular vein that had been reconstituted below the jugular foramen. Vessel loops were placed on the proximal and distal internal jugular vein to isolate this vessel for the bypass.


Figure 5. Sigmoid and transverse sinus-to-internal jugular vein saphenous interposition graft.
The superficial saphenous vein graft was harvested with minimal manipulation, and 4-0 sutures were placed across all major tributary veins. The harvested vein was gently placed in a heparin-papaverine solution and irrigated with the solution to a pressure of 8 cm H2 O to identify any potential occult leaks. Meticulous hemostasis of the wound was obtained before it was closed.
The sigmoid sinus pressure, as measured by direct puncture (27 G needle and H2O manometry), was 22 cm H2O, and the internal jugular vein pressure was 4 cm H2O. The dura was incised on either side of the venous sinus so the junction of the sigmoid and transverse sinuses could be isolated with temporary clips. A 6-mm linear incision was made at the junction, and the superficial femoral vein was anastomosed to the junction of the sinuses, end-to-side, with 10-0 Prolene (Ethicon, Johnson & Johnson Professional, Inc., Somerville, NJ) suture under direct microscopic vision. A chest tube trocar was used to fashion a retroauricular subcutaneous tunnel between the cranial and cervical exposures. Ample room was provided to allow the graft to “float” in its tunnel. The superficial saphenous vein graft was then delivered through this space while great care was exercised to avoid kinking or twisting the graft. After the graft was tunneled, the unimpeded flow of venous blood was verified before proceeding further.
The internal jugular vein was isolated, and temporary clips were applied proximally and distally to the site of anastomosis. The vein graft was anastomosed to the internal jugular vein, end-to-side, using 10-0 Prolene suture (Fig. 5). The patency of the graft was demonstrated by intraoperative Doppler ultrasonography. The patient was administered an intravenous load of heparin (7500 U) after the retroauricular tunneling was completed. The wound was closed after hemostasis was obtained to avoid compressing the graft.
Postoperative Course
The patient was maintained on heparin (1000 U/hr) for 4 days after surgery and then on aspirin. Dysphagia resolved within 3 weeks, and no new postoperative deficits developed. A postoperative angiogram demonstrated patency of the bypass graft. Three months after surgery, the patient’s neurological condition had improved, but he was not ambulatory.
Discussion
One previous case of symptomatic spinal cord compression from dilated epidural veins has been reported.3 That patient presented with progressive cervical myelopathy caused by a plexus of thrombosed dilated epidural veins dorsal to the cervicothoracic junction. The epidural venous plexus was successfully resected through a cervical laminectomy, and the patient’s neurological condition improved. Otherwise, only scattered reports have documented symptomatic compression of the lumbosacral nerve root by epidural varicose veins,1,6,13,14,19,20 which appear to have an incidence between 1.5 and 1.3%. When, however, epidural compression is considered as a contributing factor along with herniated nucleus pulposus, the incidence of compression may be higher.6,19
On T1-weighted MR imaging, the normal epidural venous plexus sometimes appears as a thin layer of contrast enhancement along the ventral aspect of the upper cervical spinal canal and within the neural foramina.4 The thick rind of nonspecific enhancement on our patient’s MR images raises the issue of differential diagnostic imaging of an epidural mass. Besides vascular lesions, including the rare cervical epidural hemangioma,5 neoplastic16 and infectious etiologies15 must be considered. Variceal enlargement of the epidural plexus is another possibility. Our patient’s T1-weighted MR images showed areas of mixed signal intensity as well as a slight enhancement of the ventral epidural mass on T2-weighted images. These findings, however, are not pathognomonic of this lesion.
Both congenital and acquired factors have been implicated in the evolution of epidural varicosities.6,8,19 In our patient, however, the mechanism underlying the development of the robust ventral epidural venous plexus with consequent spinal cord compression appears to be unique. Four-vessel cerebral and aortic arch angiography and extensive venography performed after the first operation documented complete occlusion of both internal jugular veins just caudal to the jugular foramen. On digital subtraction angiography, significant venous return through the epidural venous plexus was also visible. The epidural venous plexus provided collateral venous return in the presence of bilateral occlusion of the internal jugular vein.
The exact pathophysiology of our patient’s myelopathy is not entirely clear. It is tempting to hypothesize that the bilateral occlusion of the internal jugular vein caused the blood to be shunted progressively through the epidural venous plexus. However, venous hypertension, direct compression of the spinal cord, or both could have caused the myelopathy. Yet, experienced angiographers have recorded the reflux of contrast media into the intradural venous plexus during epidural venography.9 Transmitted elevated venous pressure might therefore be partially responsible for continued spinal cord insult, as is the case with spinal dural arteriovenous malformations.12
After the initial attempt at surgical treatment, a direct surgical attack was untenable in this patient. Furthermore, interrupting the epidural venous plexus would have destroyed a major route for the egress of intracranial venous blood. The other treatment option was to attempt to approach the pathology directly by providing an alternative, low-resistance circuit for the return of intracranial venous blood to the systemic circulation—a consideration not without precedent.2,10,11 Options cited for internal jugular vein reconstruction have included the use of saphenous vein interposition grafts, the so-called “spiral saphenous vein graft,” and the use of synthetic (e.g., polytetrafluoroethylene) graft materials with and without endothelial sodding.7,17,18
Given the pressure and flow variations anticipated within such a graft, we elected to proceed with a simple saphenous interposition graft using an end-to-side technique at both the proximal and distal anastomotic sites. The frailty of such constructs is well known, and the head-and-neck literature suggests that a pressure differential is required to maintain graft patency.2 Clearly, serial Doppler ultrasonographic and angiographic follow-up is indicated for this patient, who continues to receive aspirin therapy as an outpatient.
Summary
We have presented a patient with progressive cervical myelopathy as a consequence of dilated epidural venous channels at the craniocervical junction. The obstruction of normal routes of venous outflow from bilateral jugular vein occlusion directed the venous return into the epidural venous plexus. Only the initial surgical approach yielded the diagnosis, which was not apparent from the patient’s preoperative MR imaging and CT studies. Angiography delineated the vascular anatomy and allowed treatment by creating an alternative, low-resistance circuit for venous egress.
References
- Bücheler E, Frommhold H: Angiographic examinations of spinal vascular abnormalities [German]. Fortschr Geb Roentgenstr Nuklearmed 117:262-269, 1972
- Comerota AJ, Harwick RD, White JV: Jugular venous reconstruction: A technique to minimize morbidity of bilateral radical neck dissection. J Vasc Surg 3(2):322-329, 1986
- Dickman CA, Zabramski JM, Sonntag VKH, et al: Myelopathy due to epidural varicose veins of the cervicothoracic junction. Case report. J Neurosurg 69:940-941, 1988
- Flannigan BD, Lufkin RB, McGlade C, et al: MR imaging of the cervical spine: Neurovascular anatomy. AJR 148:785-790, 1987
- Golwyn DH, Cardenas CA, Murtagh FR, et al: MRI of a cervical extradural cavernous hemangioma. Neuroradiology 34:68-69, 1992
- Gümbel U, Pia HW, Vogelsang H: Lumbosacral vascular anomalies as the cause of ischialgia [German]. Acta Neurochir (Wien) 20:131-151, 1969
- Herring MB: Endothelial cell seeding (review). J Vasc Surg 13(5):731-732, 1991
- Ivanovici F: Urine retention: An isolated sign in some spinal cord disorders. J Urol 104:284-286, 1970
- Lasjaunias P, Berenstein A: Surgical Neuroangiography 3. Functional Vascular Anatomy of Brain, Spinal Cord and Spine. Berlin: Springer-Verlag: 1990
- Leafstedt SW, Rubenstein RB, Pallanch JF, et al: Spiral saphenous vein graft for replacement of internal jugular vein: A series of case reports. Angiology 36(11):827-831, 1985
- McGovern PJ, Jr., Swan KG: Management of bilateral internal jugular venous injuries. Injury 16(4):259-260, 1985
- Oldfield EH: Spinal arteriovenous malformations, in Wilkins RH, Rengechary SS (eds): Neurosurgery Update II. New York: McGraw-Hill, 1991, pp 186-196
- Oliver RJ, Greenwood RC, Smith D, et al: Spinal varicosities complicated by pregnancy. Case report. Am J Obstet Gynecol 94:258-260, 1966
- Rosenfeld M: Sciatica caused by epidural venous anomalies. A case of L5-S1 sciatica 9 years after operation [French]. Rev Rhum Mal Osteoartic 39:47-49, 1972
- Sandhu FS, Dillon WP: Spinal epidural abscess: Evaluation with contrast-enhanced MR imaging. AJNR 12(6):1087-1093, 1991
- Sze G, Krol G, Zimmerman RD, et al: Malignant extradural spinal tumors: MR imaging with Gd-DTPA. Radiology 167:217-223, 1988
- Welch M, Durrans D, Carr HM, et al: Endothelial cell seeding: A review (review). Ann Vasc Surg 6(5):473-484, 1992
- Williams SK, Carter T, Park PK, et al: Formation of a multilayer cellular lining on a polyurethane vascular graft following endothelial cell sodding. J Biomed Mater Res 26(1):103-117, 1992
- Zarski S, Styczynski T: Varicosity of the lower part of the vertebral canal [Polish]. Neurol Neurochir Pol 12:67-72, 1978
- Zimmerman GA, Weingarten K, Lavyne MH: Symptomatic lumbar epidural varices. Report of two cases. J Neurosurg 80:914-918, 1994
