
Halstead Impairment Index, Wechsler IQ, and the BNI Screen for Higher Cerebral Functions
Authors
George P. Prigatano, PhD
Blanca Palencia, MS
Division of Neurology, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
Abstract
Two independent groups of brain dysfunctional patients were administered the BNI Screen for Higher Cerebral Functions (BNIS). Group 1 (n=47) was also administered the Halstead-Reitan Neuropsychological Battery (HRB) and the Wechsler Adult Intelligence Scale, Revised form (WAIS-R). Group 2 (n=50) was administered only the WAIS-R. For Group 1, the BNIS total score also correlated –.61 with the Revised Halstead Impairment Index (HII) score and +.58 with Full Scale IQ. For Group 2, BNIS total score correlated +.53 with Full Scale IQ. These findings suggest that the brief BNIS is a valid neuropsychological test.
Key Words: higher cerebral functions, neuropsychology, psychological testing
The BNI Screen for Higher Cerebral Functions (BNIS) was designed to address many of the problems associated with traditional cognitive screeninginstruments.[9] It is brief and has good inter-rater and test-retest reliability.[20] When the total score obtained from the BNIS is used in conjunction with subtest scores, the instrument’s sensitivity is good and its specificity is promising.[12] Its seven subtests measure speech and language, visuospatial and visual problem solving, affect perception and expression, awareness, orientation, attention-concentration, and memory. Together, these subtests appear to discriminate right and left hemispheric dysfunction in some patients.[12] However, a persistent question with the BNIS and other screening tests of higher cerebral functioning is whether their summary information correlates with well-established, more extensive neuropsychological tests.
The Halstead-Reitan Neuropsychological Test Battery (HRB) is a clinically useful but lengthy assessment tool that is especially helpful for differentiating patients with brain dysfunction from those without.[7] A summary measure of the HRB, known as the revised Halstead Impairment Index (HII) score, reliably differentiates brain dysfunctional patients from normal controls[18,24] and nonpsychotic psychiatric patients.15 Initially, the HII correlated to the Wechsler-Bellevue intelligence quotient (IQ) in the range of –.50 for brain dysfunctional patients.[18] Other studies have documented significant correlations between performance on various Halstead tests and the Wechsler Adult Intelligence Scale(WAIS).[3,6,28] A significant correlation between the BNIS total score and the HII in brain dysfunctional patients would provide further evidence of the former’s concurrent validity and clinical utility.
Consequently, the present study examined the relationship between the BNIS total score and the revised HII and the WAIS-Revised IQ (WAIS-R). As observed by Reitan,[18] the HII score was predicted to correlate with the WAIS-R Verbal, Performance, and Full Scale IQ measures. Based on this assumption, the BNIS total score was predicted to correlate negatively and significantly with the HII score and positively and significantly with the WAIS-R Verbal, Performance, and Full Scale IQ measures in brain dysfunctional patients. To further the evaluation of the construct validity of the BNIS, the speech and language subtest of the BNIS was predicted to correlate significantly and positively with the Verbal but not with the Performance IQ measures from the WAIS-R. In contrast, the visuospatial subtest score of the BNIS was predicted to correlate positively with the WAIS-R Performance IQ but not with Verbal IQ. Finally, the Awareness subtest score was predicted to correlate with neither the HII nor any measure of IQ because these traditional neuropsychological tests do not sample this dimension.[11]
Method
Subjects
Two independent groups of brain dysfunctional patients participated in the study. All patients had documented brain disorders and had been referred to our Department of Clinical Neuropsychology for neuropsychological examination. Case selection was based on four inclusion criteria: (1) Patients had a medically documented brain disorder; (2) patients were not involved in litigation; (3) the neuropsychological test protocols were complete; and (4) there was no history of psychiatric disability.
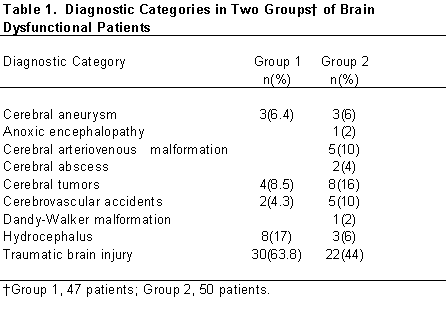
Group 1 consisted of 16 females and 31 males (mean age, 37.6 years; SD=12.3). Group 2 comprised 16 females and 34 males (mean age, 39.86 years; SD=12.42). The mean ages for the two groups were not significantly different (t=0.876, df=95, p=.38). The mean years of education for Group 1 was 14.46 (standard deviation [SD]=3.73) and 13.89 (SD=2.90) for Group 2; the mean difference was not significant (t=–0.839, df=95, p=.404). The chronicity of the brain lesion was defined as the months since onset of brain injury to time of testing. The mean months of chronicity was 32.57 (SD=81.23) for Group 1 and 38.99 (SD=107.62) for Group 2, but the mean difference was not significant (t=0.329, df=94, p=.743). The two groups of patients also did not differ significantly in terms of years of education or male-to-female ratio. Although the neuropathology of the two groups was heterogeneous (Table 1), the most common diagnosis in both groups was traumatic brain injury (Group 1=64%; Group 2=44%).
Materials and Procedures
The HRB and the WAIS-R were administered and scored according to standardized procedures.[17,19,26] The HRB includes the Halstead Category Test, the Tactual Performance Test, the Speech Perception Test, the Seashore Rhythm Test, and the Finger Tapping Test. An HII score was derived from these tests using Reitan’s procedures.[17] The WAIS-R consists of 11 subtests from which both a Verbal IQ and a Performance IQ are calculated. The various subscale scores are combined to calculate a Full Scale IQ.[26]
The BNIS materials consist of a laminated stimulus booklet, record form, and standard stopwatch. The BNIS requires 10 to 25 minutes to administer as described elsewhere.[9,12] The total score, the subscale scores, and individual items (Table 2) are also described elsewhere.[16,21] Higher scores indicate less impaired functioning. This study involved the total score and the subtest scores obtained on the Speech and Language subscale, the Visuospatial subscale, and the Awareness versus performance subscale.
All neuropsychological tests were administered by either a board-certified clinical neuropsychologist, a postdoctoral fellow in clinical neuropsychology, or a trained neuropsychology psychometrist. Group 1 was administered the BNIS, the entire HRB, and the WAIS-R as part of a comprehensive neuropsychological examination that required an average of 5 to 6 hours. Group 2 was administered the BNIS and the WAIS-R but not the HRB; their testing required about 2 hours. All patients were given the BNIS first, followed by other neuropsychological tests as their clinical situation demanded.

Data Analysis
All statistical analyses were performed with Systat Student Version. Descriptive statistics were calculated for both groups. Age, education, and chronicity of the lesion were compared by t-tests. Pearson correlation coefficients were calculated for the revised HII, for the Wechsler IQ scales, and for the BNIS total score versus the HII and the Wechsler IQ scales. The BNIS scores for the Speech and Language and Visuospatial subtests correlated with the Verbal and Performance IQs as outlined in the predictions. The Awareness versus performance subscale has only one item and provides a simple dichotomy (passed or not passed) score. Therefore, the Point Biserial correlation was used to relate performance on this subtest to the HII and the Wechsler IQ values.
Results
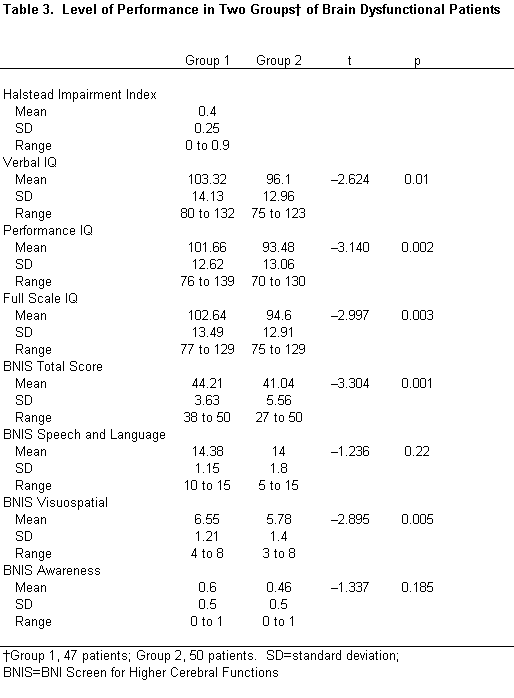
Group 2 patients consistently performed at a lower level than Group 1 patients (Table 3).
Replication of Reitan’s Findings
The present study replicated Reitan’s[18] earlier observations (Table 4). The magnitude and direction of the correlations were also similar to those reported by Reitan.[18] In the present study, the responses of the brain dysfunctional patients appeared consistent with well-known relationships. Thus, the findings obtained with the HII score and the BNIS score seem to be based on reliable test observations.

Correlation of BNIS Total Score with HII and WAIS-R IQ
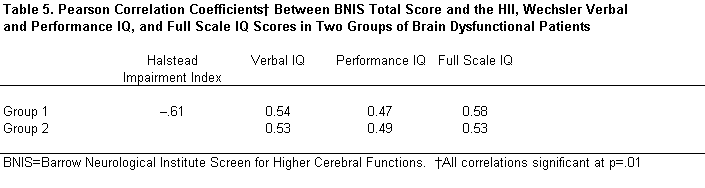
In Group 1, the correlation between the BNIS total score and the revised HII score was –.61 (p<.01, Table 5). The first prediction was therefore supported. The BNIS total score also significantly correlated with Verbal, Performance, and Full Scale IQ values obtained from the WAIS-R (Table 5). Thus, the second prediction was also supported.
BNIS Subtest Scores and Neuropsychological Test Findings
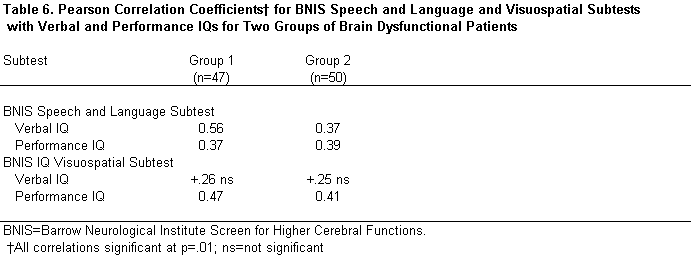
Contrary to prediction, scores on the BNIS Speech and Language subtest correlated with both WAIS-R Verbal and Performance IQ values in both Groups 1 and 2 (Table 6). However, as predicted, the BNIS Visuospatial Subtest Score correlated only with the WAIS-R Performance IQ value (Table 6).
The Point Biserial correlation of the Awareness versus the Performance item correlated with the HII in Group 1 (r=–.34, p<=.05) but with none of the IQ values (Verbal IQ versus Awareness, r=.07; Performance IQ versus Awareness, r=.06; Full Scale IQ versus Awareness, r=.08). In Group 2, however, Verbal IQ and Awareness did correlate with this BNIS subscale (r=.43, n=48, p<.05) as did Full Scale IQ and Awareness (r=.36, n=48, p=.05). In Group 2 as in Group 1, Performance IQ and Awareness were not significantly correlated (r=.23).
Discussion
Screening tests that adequately sample neuropsychological function are needed to help make differential diagnoses, to monitor patients’ recovery (or decline), and to provide objective information on which to base recommendations for patients’ management. Malloy and coworkers8 have noted that many brief screening instruments have good inter-rater reliability but “substantial false negative ratios,” particularly when used to assess patients with right hemisphere lesions or “mild diffuse impairment.” They have commented that an “ideal cognitive screen instrument” would require 5 to 15 minutes to administer and would sample “all major cognitive domains including orientation, attention-concentration, executive, language, spatial, and memory functions” (p. 140).
A persistent problem with screening tests of higher cerebral functions is that they seldom correlate strongly with more extensive measures of neuropsychological performance.[5] Yet, task forces of the American Academy of Neurology[1] and the American Neuropsychiatric Association8 have emphasized the need for clinically sensitive and cost-efficient methods for measuring disturbances in higher brain function. The present study documents that the total score obtained from the BNIS significantly correlates with the HII and the WAIS-R. These findings expand the existing validity studies on this instrument.[12,21]
A wide sample of behaviors must be observed repetitively before one can reliably conclude disturbances in brain function from psychological test performances.[19] The brief BNIS may relate significantly to more extensive measures of neuropsychological functioning because it samples a broad array of cognitive and affective disturbances, as mentioned earlier, known to be at high risk after various brain disorders. The total score, which takes 10 to 25 minutes to obtain, is based on all of these dimensions. Thus, the BNIS appears to be a comprehensive and valid measure.
Although not the focus of this report, the BNIS provides both qualitative and quantitative information, which experienced neurological clinicians have long recognized can be crucial to making accurate differential diagnoses and to managing patients. Both sources of information may be useful in determining which brain dysfunc[ti]onal patients will achieve inpatient neurorehabilitation goals soon after the onset of their brain lesion.[16] The abilities to predict memory performance (a possible measure of awareness) accurately and to show spontaneous affect were significantly related to successful rehabilitation outcomes. The need to explore both cognitive and affective disturbances has seldom been included in screening tests. This is one advantage of the BNIS.
Subtest Performance on the BNIS
In two independent samples of brain dysfunctional patients who varied in their level of neuropsychological impairment, the BNIS visuospatial subtest score correlated with the WAIS Performance IQ score but not with the Verbal IQ score as predicted. The BNIS visuospatial and WAIS-R Performance IQ scores appear to share about 25% of the test variance. Wass[25] reported a Pearson correlation coefficient of +.44 between the WAIS-R Block Design and the visuospatial subtest score of the BNIS. Collectively, these observations strengthen the construct validity of the BNIS subtests, which may indeed be sensitive to dysfunction often associated with the right cerebral hemisphere.[7] This feature is a decided advantage compared to other screening tests.
The BNIS Speech and Language subtest correlated with both Verbal and Performance IQ. The Speech and Language subtest of the BNIS also correlates with a variety of verbal and nonverbal problem-solving skills.[25] This subtest of the BNIS may be related to several complex problem-solving skills. Although the BNIS Speech and Language subtest and the WAIS Verbal IQ shared approximately 35% of the variance,25 this subtest shares variability with many nonverbal problem-solving skills. Left hemisphere lesions seldom, if ever, impair language function in isolation from other cognitive deficits,[10,22] perhaps explaining why the subtest did not relate in a simple fashion to the WAIS Verbal IQ.
The Awareness subtest of the BNIS correlated significantly with the HII but showed no consistent relationship to IQ measures in the two groups of brain dysfunctional patients. Brain dysfunctional patients who demonstrate what might broadly be called denial of disability or impaired self-awareness seldom differ from other patients on Wechsler IQ measures.[11,27] Measures of impaired awareness obtained from patients several months after traumatic brain injury (TBI) relate modestly (about r=–.39) to admitting scores on the Glasgow Coma Scale (GCS).[14,23] Dikmen and coworkers4 have also reported a dose-response relationship between the HII and GCS scores after TBI. One year after injury, however, correlations between disturbances of consciousness and later neuropsychological impairment, as reflected on a variety of measures, range between +.40 and +.50. Perhaps severity of initial brain injury affects awareness and measures such as the HII in a similar but also different manner and accounts for the modest relationship observed between the Awareness subtest score and the HII in Group 1 (r=–.34). The magnitude of the correlation is substantially greater when several higher cerebral functions are measured as reflected by the correlation of –.61 between the BNIS total score and the HII.
Impaired awareness may disrupt both cognitive and affective functioning.[10] Therefore, existing neuropsychological measures seldom correlate in a robust way with disturbances of awareness. That the BNIS attempts to sample this important dimension is an added advantage compared to many existing screening tests.
Study Limitations
The present study did not specifically address how different types of brain disorders actually affect performance on the BNIS. For example, different types of neuropathological lesions differentially affect neuropsychological performance.[2] Clinically, we have observed that different patterns of injury are associated with different neuropathological conditions. However, further studies are needed to explore this important dimension when interpreting the findings from the BNIS.
The present study did not address the sensitivity and specificity of the BNIS. In the standardization sample of 500 brain dysfunctional patients and 200 normal controls,[13] the sensitivity of the total score was 92% but its specificity was only 48%. The specificity, however, was 93% for the ability to recall three words with distraction (one of the items on the BNIS). The total score from any screening instrument may well be sensitive but lack specificity. Therefore, clinicians must consider measures other than the BNIS total score to increase estimates of specificity in large groups of individuals screened for higher cerebral dysfunction.
Conclusions
The BNIS appears to be a promising screening test for higher cerebral dysfunction. The total score obtained from this measure correlated with both the HII and the Wechsler IQ. Relationships between specific BNIS subtests and Verbal and Performance IQ measures of the WAIS-R were consistent with earlier findings. The data from these two independent samples of brain dysfunctional patients suggest that the BNIS is a useful measure for clinical practice and research.
References
- American Academy of Neurology: Assessment: Neuropsychological testing of adults. Considerations for neurologists. Neurology 47:592-599, 1996
- Anderson SW, Damasio H, Tranel D: Neuropsychological impairments associated with lesions caused by tumor or stroke. Arch Neurol 47:397-405, 1990
- Chelune GJ: A reexamination of the relationship between the Luria-Nebraska and Halstead-Reitan batteries: Overlap with the WAIS. J Consult Clin Psychol 50:578-580, 1982
- Dikmen SS, Machamer JE, Winn HR, et al: Neuropsychological outcome at 1-year post head injury. Neuropsychology 9:80-90, 1995
- Feher EP, Mahurin RK, Doody RS, et al: Establishing the limits of the mini-mental state. Examination of ‘subtests’. Arch Neurol 49:87-92, 1992
- Golden CJ, Kane R, Sweet J, et al: Relationships of the Halstead-Reitan neuropsychological battery to the Luria-Nebraska neuropsychological battery. J Consult Clin Psychol 49:410-417, 1981
- Lezak MD: Neuropsychological Assessment. New York: Oxford University, 1995
- Malloy PF, Cummings JL, Coffey CE, et al: Cognitive screening instruments in neuropsychiatry: A report of the Committee on Research of the American Neuropsychiatric Association. J Neuropsychiatry Clin Neurosci 9:189-197, 1997
- Prigatano GP: BNI Screen for Higher Cerebral Functions: Rationale and initial validation. BNI Quarterly 7(1):2-9, 1991
- Prigatano GP: Principles of Neuropsychological Rehabilitation. New York: Oxford University, 1999
- Prigatano GP, Altman IM: Impaired awareness of behavioral limitations after traumatic brain injury. Arch Phys Med Rehabil 71:1058-1063, 1990
- Prigatano GP, Amin K, Rosenstein LD: Validity studies on the BNI Screen for Higher Cerebral Functions. BNI Quarterly 9(1):2-9, 1992
- Prigatano GP, Amin K, Rosenstein LD: Manual for the BNI Screen for Higher Cerebral Functions. Phoenix: Barrow Neurological Institute, 1995
- Prigatano GP, Bruna O, Mataro M, et al: Initial disturbances of consciousness and resultant impaired awareness in Spanish patients with traumatic brain injury. J Head Trauma Rehabil 13:29-38, 1998
- Prigatano GP, Parsons OA: Relationship of age and education to Halstead Test performance in different patient populations. J Consult Clin Psychol 44:527-533, 1976
- Prigatano GP, Wong JL: Cognitive and affective improvement in brain dysfunctional patients who achieve inpatient rehabilitation goals. Arch Phys Med Rehabil 80:77-84, 1999
- Reitan RM: Manual for Administration of Neuropsychological Test Batteries for Adults and Children. Tucson, AZ: Reitan Neuropsychology Laboratories, 1955
- Reitan RM: Investigation of relationships between “psychometric” intelligence and “biological” intelligence. J Nerv Ment Dis 123:536-541, 1956
- Reitan RM: Theoretical and methodological bases of the Halstead-Reitan Neuropsychological Test Battery, in Grant I, Adams KM (eds): Neuropsychological Assessment of Neuropsychiatric Disorders. New York: Oxford University, 1986, pp 3-30
- Rosenstein LD, Prigatano GP, Amin K: Reliability studies for the BNI Screen for Higher Cerebral Functions. BNI Quarterly 8(3):24-28, 1992
- Rosenstein LD, Prigatano GP, Nayak M: Differentiating patients with higher cerebral dysfunction from patients with psychiatric or acute medical illness using the BNI Screen for Higher Cerebral Functions. Neuropsychiatry Neuropsychol Behav Neurol 10 :113-119, 1997
- Satz P: Specific and nonspecific effect of brain lesions in man. J Abnorm Psychol 71:65-70, 1966
- Sherer M, Boake C, Levin E, et al: Characteristics of impaired awareness after traumatic brain injury. J Int Neuropsychol Soc 4:380-387, 1998
- Vega A, Jr., Parsons OA: Cross-validation of the Halstead-Reitan tests for brain damage. J Consult Psychol 31:619-625, 1967
- Wass PJ: An analysis of the construct-related and ecological validity of the Barrow Neurological Institute Screen for Higher Cerebral Functions. Ph.D. diss., University of Windsor, Windsor, Ontario, 1997
- Wechsler D: Wechsler Adult Intelligence Scale-Revised. San Antonio, TX: The Psychological Corporation, 1981
- Weinstein EA, Kahn RL: Denial of Illness. Symbolic and Physiological Aspects. Springfield, IL: Charles C Thomas, 1955
- Zillmer EA, Fowler PC, Newman AC, et al: Relationships between the WAIS and neuropsychological measures for neuropsychiatric inpatients. Arch Clin Neuropsychol 3:33-45, 1988
