
Evaluation of EC-IC Bypass Grafts Using CT Angiography
Matthew T. Walker, MD*
Janak K. Acharya, MD
C. Roger Bird, MD
Shahram Partovi, MD
Division of Neuroradiology, Barrow Neurological Institute, St. Joseph’s Hospital and Medical Center, Phoenix, Arizona
*Current Address: Division of Neuroradiology, Northwestern Memorial Hospital, Chicago, Illinois
Abstract
Extracranial-to-intracranial (EC-IC) bypass can be applied in a variety of clinical scenarios including cerebrovascular occlusive disease, combined occlusion-bypass procedures for giant aneurysms, and bypass procedures for tumors. The standard preoperative assessment and postoperative evaluation of these patients are based on digital subtraction angiography (DSA). Although safe, the overall complication rate associated with DSA is considerable and ranges from groin hematomas to stroke. Computed tomographic (CT) angiography is a less invasive technique that also can be used to assess the carotid and cerebral vasculature. It has already been applied to aneurysm detection, postclipping evaluation, acute stroke, chronic steno-occlusive disease, and blunt neck trauma. In our experience, CT angiography is a viable alternative to DSA for the preoperative and postoperative evaluation of patients who receive EC-IC bypass grafts.
Key Words: angiography, bypass, computed tomography, extracranial, intracranial
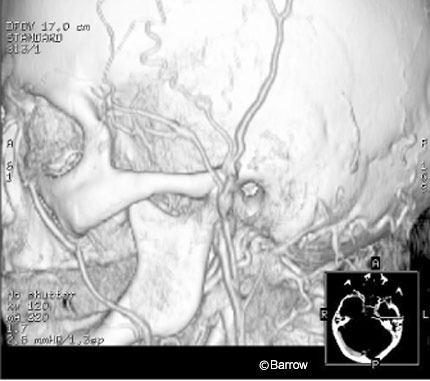
In 1985, the Cooperative Study of extracranial-intracranial arterial anastomosis (EC-IC Bypass Study) concluded that bypass revascularization did not reduce the risk of stroke in the subgroups studied.[16] However, the study was flawed by selection bias–a disproportionately high number of asymptomatic patients were included. This study also failed to analyze patients with conditions such as cerebral hypoperfusion, ischemic ocular syndromes, or moyamoya disease or to assess the use of EC-IC bypass as it relates to surgery for aneurysms or tumors.[2] Consequently, EC-IC bypass procedures remain important alternatives for the cerebral revascularization of patients with chronic steno-occlusive disease with hypoperfusion, moyamoya disease, and aneurysms that must be isolated. We have used computed tomographic (CT) angiography to evaluate the course and caliber of the superficial temporal artery (STA) to determine its suitability for bypass surgery and to assess the postoperative patency of bypass grafts.
Technical Considerations of CT Angiography
CT angiography is made possible by advances in slip-ring and helical acquisition technologies, multidetector scanners, and three-dimensional (3D) reconstruction software. Slip-ring technology refers to the ability of the gantry to rotate continuously 360 degrees around the patient. A helical acquisition is accomplished by patient translation through the gantry during data collection. Single-detector CT scanners have one detector for data collection whereas multidetector scanners have two or more. At our institution, we use a four-detector General Electric LightSpeed scanner (General Electric Company, Milwaukee, WI). The resultant subsecond scanning has revolutionized advanced CT applications.
CT angiography times a scan to an intravenous infusion of iodinated contrast media. An 18-gauge antecubital intravenous line is optimal. Scanning parameters include a field of view of 17 cm, 140 mA, and 250 kV. The mean scan delay is 9 to 16 seconds but varies depending on a patient’s hemodynamic status. Images are acquired from the skull base rostrally through the ventricles at a thickness of 2.5 mm and a spacing of 1.25 mm. Iodinated contrast media (40 to 80 ml) is infused during image acquisition. Multiplanar volume (sagittal, coronal, axial) reformatted (MPVR) images are created at a thickness of 1.25 mm and spacing of 0.6 mm. Axial source images and MPVRs are interactively reviewed on our picture archiving and communications system. If necessary, 3D software enables neurosurgeons to visualize the vasculature in familiar angiographic projections and to observe the osseous anatomy if relevant to the bypass procedure.
The risks of CT angiography include contrast extravasation into the arm and allergic reactions to the iodinated contrast. The pitfalls of CT angiography primarily involve technical failures such as suboptimal timing of the bolus (see CT Angiography and Stroke in this issue). Early scanning diminishes the degree of opacity of more proximally located vessels; late scanning creates too much venous opacification.
CT Angiographic Evaluation of Chronic Steno-Occlusive Disease
In adults, the signs and symptoms of cerebral ischemia are typically caused by thromboembolic events.[2,6] Although a minority, patients with carotid or cerebrovascular disease associated with cerebral hypoperfusion are an important subgroup. Cerebral hypoperfusion can be ascertained by cerebral blood flow studies such as stable xenon CT and CT or magnetic resonance (MR) perfusion imaging.[4] Paired flow studies with a vasodilator challenge (e.g., acetazolamide) help to determine the status of the microcirculation and to assess the patient’s autoregulatory reserve.[12]
For anterior circulation disease, the most commonly performed EC-IC anastomosis is the STA-to-ipsilateral middle cerebral artery (MCA) bypass.[14] Variations include STA-to-contralateral MCA bypass, STA-to-middle meningeal artery bypass, and various vein or prosthetic interposition grafts. EC-IC bypass procedures for posterior circulation disease are also eclectic and include STA-to-posterior cerebral artery (PCA), STA-to-superior cerebellar artery (SCA), STA-to-anterior inferior cerebellar artery (AICA), and STA-to-posterior inferior cerebellar artery (PICA) bypasses.[14] The occipital artery (OA) can be used to bypass the distributions of AICA or PICA.
The preoperative evaluation of bypass candidates includes assessing the extracranial vasculature for an adequate bypass vessel such as the STA or OA by the gold standard, digital subtraction angiography (DSA). DSA shows the caliber and course of the potential bypass graft but displays osseous structures less optimally. CT angiography shows the same features of a potential bypass vessel but is more effective than DSA at identifying the osseous relationships pertinent to the neurosurgeon who must harvest this small vessel (Fig. 1). Based on current advances in CT angiography, preoperative DSA for the sole purpose of road mapping the extracranial circulation is no longer indicated. CT angiography clearly depicts this anatomy with substantially less risk to the patients.
Often, however, preoperative DSA is not performed solely to visualize the extracranial circulation. Typically, it is part of a larger evaluation aimed at understanding the collateral circulation to the targeted bypass tissue. In this circumstance DSA offers advantages: Unlike CT angiography it can evaluate the dynamic blood flow to a region. However, combining preoperative CT angiography with preoperative CT perfusion imaging provides substantial additional information about the microcirculatory blood flow (see CT Perfusion Imaging, Illustrative Case 2, in this issue). This physiologic information is quantitative and may eventually supersede the need for dynamic but qualitative DSA flow studies. Alone, CT angiography may be insufficient to displace DSA as the gold standard for a broad evaluation of bypass patients. As a pair, however, CT angiography and CT perfusion imaging may provide complementary preoperative information that eliminates the need for DSA.
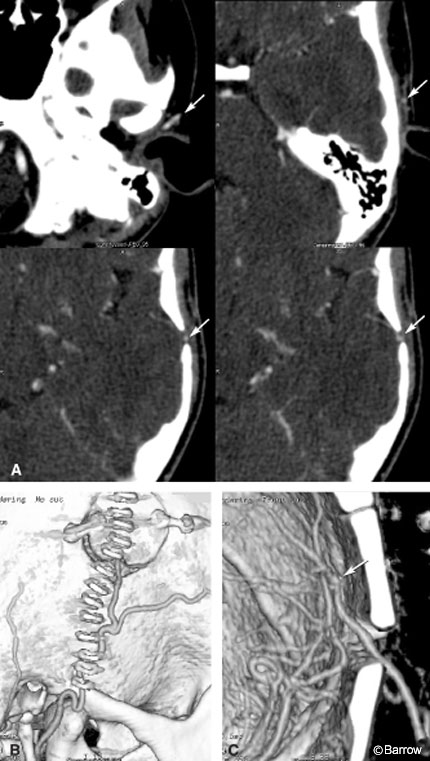
penetrating the recent craniotomy. (C) Cut-away 3D view of the same patient identifies a patent anastomosis between the STA and MCA (arrow).
Traditionally, postoperative bypass patency has been assessed with DSA.[11] The main question is whether blood flow in the graft can be assessed equally well by DSA and CT angiography. With DSA, multiple views are often necessary to profile the anastomosis. Prolonged catheterization and multiple contrast injections may be required. In contrast, once the CT angiographic images have been acquired, an infinite number of projections can be displayed to evaluate the anastomosis (Fig. 2). As in the preoperative condition, a qualitative assessment of dynamic flow distal to the anastomosis requires DSA. But again, the combination of CT angiography and CT perfusion could obviate the risks associated with DSA and provide similar information. In fact, the postoperative quantitative CT perfusion values could be compared with a patient’s preoperative values and used to assess the bypass graft at a physiologic level (see CT Perfusion Imaging, Illustrative Case 2 in this issue). Despite its higher procedural risk, DSA cannot offer clinicians this direct information.[3,7]
Evaluation of Moyamoya Disease
In 1969 Suzuki et al. first described moyamoya disease based on its angiographic appearance in Japanese children.[15] Progressive stenosis leading to complete occlusion of the supraclinoid internal carotid arteries (ICAs) results in exuberant collateral supply including an increase in the number and size of perforator branches. Stenosis of the proximal A1 segment of the anterior cerebral artery (ACA) and M1 segment of the MCA is common while involvement of the posterior circulation is unusual. Children are affected more than adults and become symptomatic with transient ischemic attacks and strokes.[5] Subarachnoid hemorrhage (SAH) is a common manifestation in adults. Prognosis depends upon the rapidity of flow through and the extent of collateral circulation.
In these patients EC-IC bypass procedures are an integral component of surgical revascularization and include direct and indirect techniques.[8,9] Direct techniques include STA-to-MCA anastomosis and saphenous vein grafting from the external carotid artery to the MCA. These techniques increase blood flow to the MCA territory but are less effective at increasing flow to the territory of the ACA, which also is affected in moyamoya disease. Indirect techniques are based on the principle of neovascularization between the extracranial circulation and intracranial circulation by placing vascular rich tissue directly on the surface of the brain. Encephalomyosynangiosis (EMS) is an indirect technique that is accomplished by the onlay of the temporalis muscle onto the brain surface. Encephaloduroarteriosynangiosis (EDAS) is a combination STA-MCA and temporalis onlay procedure. Other indirect methods include encephalogaleosynangiosis and omental onlay.
Moyamoya disease is usually diagnosed by DSA. Stenosis, occlusion of the supraclinoid ICAs, or both are hallmarks of this disease. A fine collateral supply of perforating arteries develops at the base of the brain, creating the classic “puff of smoke” appearance on DSA.[15] Other angiographic findings include EC-to-IC collateralization and leptomeningeal collateralization. CT angiography also can be used to diagnose moyamoya disease, primarily by identifying the intracranial stenoses-occlusions and the fine network of perforator collaterals at the base of the brain. Leptomeningeal and EC-IC collateralization can be inferred but are more challenging to interpret on CT angiography than on DSA.
As discussed, the disadvantages of DSA include risks associated with the procedure, such as stroke (1%), sedation (particularly in the pediatric population), and cost.[3,7] MR angiography has been suggested as an appropriate technique for evaluating the patency of bypass grafts.[1] Although MR angiography is noninvasive, its disadvantages include decreased sensitivity to slow blood flow or small vessels, patient tolerance, sedation, and cost. MR angiography has a long data acquisition time and is inferior to CT angiography for evaluating collateral circulation after EDAS.
Multidetector, helical CT angiography easily can assess the patency of a direct anastomosis such as an STA-MCA bypass.[10] This information is useful immediately after surgery and during follow up. If patency is the primary issue, follow-up CT angiography is less expensive, quicker, and less traumatic than DSA. Indirect techniques such as EMS and EDAS are more challenging to evaluate because the vessels that develop are typically at or below the resolution of imaging techniques. In that setting, cerebral blood flow studies such as CT perfusion, which are physiologic assessments of cerebral perfusion, would allow a more direct interrogation of the effectiveness of an indirect revascularization technique.
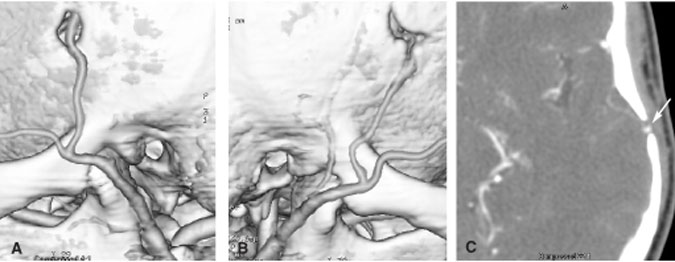
Illustrative Case 1
A 19-year-old female sought treatment for recurrent episodes of bilateral upper extremity weakness. The initial evaluation by DSA showed the classic findings of moyamoya disease. The supraclinoid segments of both ICAs were attenuated and normal MCAs could not be identified. A pre- and postdiamox challenge xenon CT examination revealed a decrease in blood flow reserve to both hemispheres. A bilateral EC-IC bypass was planned. Review of the patient’s preoperative DSA showed that the right STA was inadequate for the bypass, but the left STA was acceptable. The patient underwent an STA-to-MCA bypass on the left and a temporalis onlay was placed on the right side (Fig. 3).
Twelve months later, postoperative CT angiography confirmed continued patency of the left STA-to-MCA bypass. The right onlay could not be evaluated adequately by CT angiography. CT perfusion imaging performed at the same time as the CT angiography revealed excellent blood flow to both MCA territories. Some hypoperfused areas appeared to persist. Given the asymmetric techniques used for bypass in this patient, this case is a potent example of how CT can play a significant and relatively noninvasive role in the postoperative follow up of such young patients. On the left side, the actual anastomotic site of the STA-to-MCA bypass was clearly shown on the follow-up CT angiogram. Patency was confirmed without the need for DSA. A small, but calculable risk of stroke, was thus avoided in this young patient. The addition of CT perfusion imaging to evaluate the left hemisphere exceeded what could have been achieved by DSA alone. We not only assessed the macroanastomosis but also quantitatively evaluated the underlying microcirculation.
In the right hemisphere, no unique anastomotic site existed and neither CT angiography nor DSA would have been useful in that regard. Traditionally, DSA would have been performed to evaluate parenchymal staining qualitatively as an indirect measure of effectiveness. With CT perfusion imaging, the effectiveness of the onlay could be evaluated directly and at a physiologically meaningful level.
Evaluation of Aneurysms and Tumors
The treatment of aneurysms is based on the principle of isolating the lesion from the remainder of the arterial system, typically by surgical clipping or endovascular coiling. Some aneurysms are candidates for neither clipping nor endovascular obliteration because of their size (giant), location (cavernous), or shape (fusiform). Giant aneurysms of the cavernous sinus are examples of lesions that can be treated with combined isolation and bypass procedures. Skull base tumors that compromise the arterial circulation also can be treated effectively by isolating the affected arterial segment and by performing a bypass procedure.
The types of bypass procedures used to treat unclippable aneurysms vary according to their location. Intracavernous aneurysms can be treated by combining ICA occlusion with an STA-to-MCA bypass or with a venous interposition graft that connects the petrous ICA to a major vessel distally (e.g., MCA).[13] In the posterior circulation, bypass procedures can involve the STA, OA, or a venous interposition graft.[14]
The adequacy of aneurysm isolation and the patency of the graft can be confirmed by DSA or CT angiography. Both techniques can demonstrate patency or thrombosis of the graft (Fig. 4). STA-to-MCA bypasses can take several days to mature and may not demonstrate exuberant blood flow immediately after surgery. These patients may need to undergo a second imaging study several days later to confirm maturity of the graft. In this setting CT angiography, which is quicker, cheaper, and safer than DSA, is a viable option. CT angiography and DSA both assess the adequacy of aneurysm obliteration.
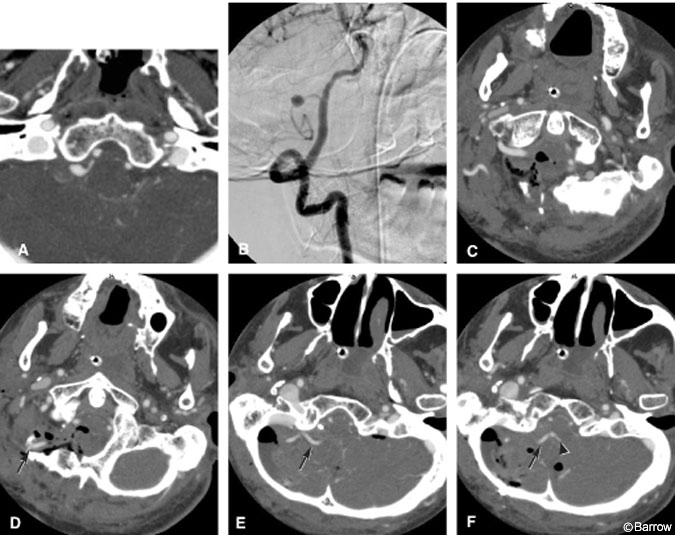
Illustrative Case 2
A 42-year-old male experienced the sudden onset of a severe headache followed by a decreased level of consciousness. Initial head CT showed an SAH in the posterior fossa. CT angiography performed immediately after the basic head CT showed a 7-mm aneurysm on the right PICA arising 1-cm distal to the origin of the vessel (Fig. 5A). Preoperative DSA confirmed the presence of the lesion and its location (Fig. 5B). No other aneurysms were seen on DSA.
The patient underwent a posterior fossa craniotomy and clip occlusion of the PICA proximal to the aneurysm. To restore distal PICA flow, the right OA was used for a concomitant bypass to the distal PICA. Postoperatively, CT angiography (Fig. 5C-F) showed excellent opacification of the distal PICA, confirming patency of the bypass. No postoperative PICA territory infarction was seen on follow-up MR imaging.
This case illustrates the comprehensive solution CT angiography can offer in assessing such vascular conditions. The aneurysm was diagnosed by CT angiography at the time of the initial head CT. It is debatable whether the preoperative DSA was necessary (see CT Angiography: A Tool for Managing Cerebral Aneurysms? in this issue). We would not have routinely performed CT angiography to assess the aneurysm clip, but the modality offered a relatively noninvasive method to confirm the patency of the bypass graft.
Conclusions
Advances in technology have significantly expanded the clinical applications of traditional CT scanners. CT angiography has benefited from subsecond scanning that permits data acquisition during bolus tracking techniques. MPVRs can produce an infinite number of projections of the volume of interest, and advanced 3D software packages produce angiographic-like images of the neck and intracranial vasculature. CT angiography can provide information similar to DSA with less risk and less cost and should be considered a viable diagnostic option. When combined with CT perfusion imaging, CT–as a modality–offers a comprehensive tool for evaluating bypass patients.
References
- Aoki T, Matsuzawa H, Houkin K, et al: Usefulness and limitation of MR imaging and MR angiography in diagnosis of juvenile moyamoya disease [Japanese]. No Shinkei Geka 21 :305-311, 1993
- Awad IA, Spetzler RF: Extracranial-intracranial bypass surgery: A critical analysis in light of the International Cooperative Study. Neurosurgery 19:655-664, 1986
- Berteloot D, LeClerc X, Leys D, et al: Cerebral angiography: A study of complications in 450 procedures [French]. J Radiol 80:843-848, 1999
- Derdeyn CP, Grubb RL, Jr., Powers WJ: Cerebral hemodynamic impairment: Methods of measurement and association with stroke risk. Neurology 53:251-259, 1999
- Ferrera PC, Curran CB, Swanson H: Etiology of pediatric ischemic stroke. Am J Emerg Med 15:671-679, 1997
- Hadley MN, Spetzler RF: Contemporary application of the extracranial-intracranial bypass for cerebral revascularization. Contemp Neurosurg 9:1-6, 1988
- Heiserman JE, Dean BL, Hodak JL, et al: Neurologic complications of cerebral angiography. AJNR Am J Neuroradiol 15:1381-1383, 1994
- Houkin K, Kamiyama H, Takahashi A, et al: Combined revascularization surgery for childhood moyamoya disease: STA-MCA and encephalo-duro-arterio-myo-synangiosis. Childs Nerv Syst 13:24-29, 1997
- Karasawa J, Kikuchi H, Furuse S, et al: Treatment of moyamoya disease with STA-MCA anastomosis. J Neurosurg 49:679-688, 1978
- Kikuchi M, Asato M, Sugahara S, et al: Evaluation of surgically formed collateral circulation in moyamoya disease with 3D-CT angiography? Comparison with MR angiography and X-ray angiography. Neuropediatrics 27:45-49, 1996
- Lewis BD, Kwan E, Enzmann DR: DSA evaluation of the STA-MCA bypass. Neuroradiology 26:209-212, 1984
- Rogg J, Rutigliano M, Yonas H, et al: The acetazolamide challenge: Imaging techniques designed to evaluate cerebral blood flow reserve. AJR Am J Roentgenol 153:605-612, 1989
- Spetzler RF, Carter LP: Revascularization and aneurysm surgery: Current status. Neurosurgery 16:111-116, 1985
- Spetzler RF, Hadley MN: Extracranial-intracranial bypass grafting: An update, in Wilkins R, Rengachary SS (eds): Neurosurgery. New York: McGraw-Hill, 1996, pp 2157-2168
- Suzuki J, Takaku A: Cerebrovascular “moyamoya” disease. Disease showing net-like vessels in base of brain. Arch Neurol 20:288-299, 1969
- The EC/IC Bypass Study Group: Failure of extracranial-intracranial arterial bypass to reduce the risk of ischemic stroke. Results of an international randomized trial. N Engl J Med 313:1191-1200, 1985
