Kelly Laboratory
Laboratory Focus
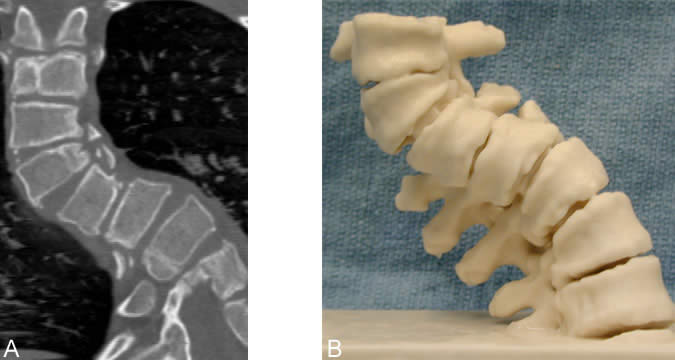
The personnel of the Spinal Biomechanics Laboratory study the mechanical behavior of the spine in its normal condition and after injury, disease, or surgical intervention. The lab works closely with clinical neurosurgeons in the Division of Neurosurgery. Neurosurgical residents, fellows, and Barrow staff perform experiments on specially prepared human cadaveric spines. Injuries that mimic those seen in patients are induced in the specimens, and surgical procedures identical to those in the operating room are performed.
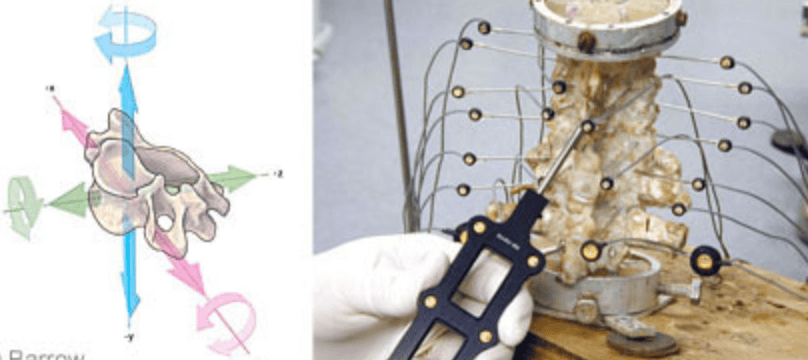
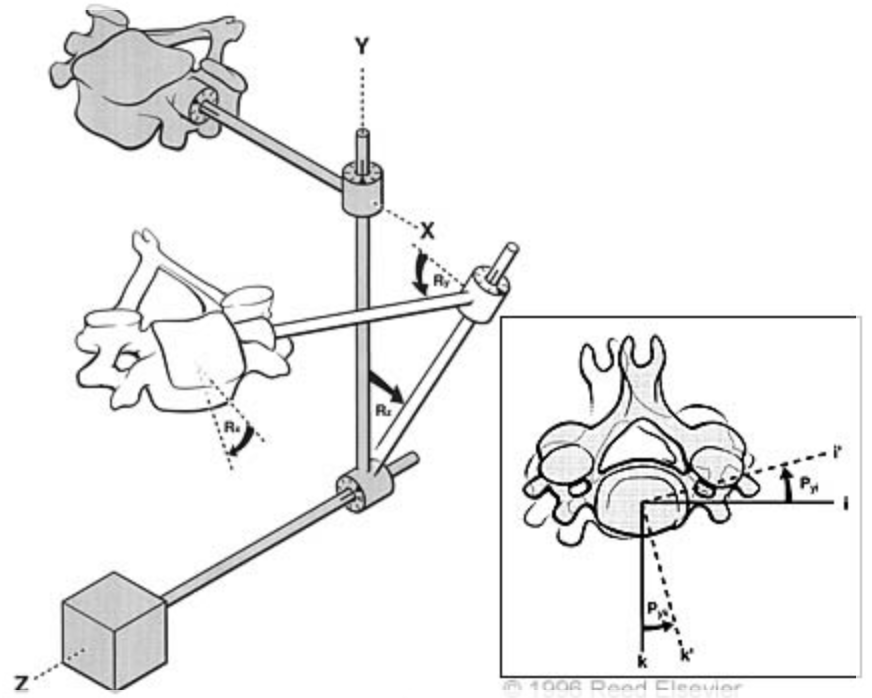
Before and after injuring or performing surgery on a cadaveric spine, the specimen is tested mechanically by applying carefully controlled loads through a system of cables and pulleys or belt, motor, and weights while measuring the three-dimensional motion using an optical system. The loads are similar to the maximum forces a person applies to the spine during daily activities.
The laboratory’s principal goal is to improve healthcare by investigating how different surgical procedures affect the mechanical response of the spine—particularly, what effect different procedures have on spinal stability. Studies like the ones performed in our laboratory are published to help surgeons decide how best to treat patients requiring spinal surgery; these studies may lead to new and better techniques or devices for spinal surgery.

Contact Information
Brian Kelly, PhD
Assistant Professor, Spinal Biomechanics
350 West Thomas Road
Phoenix, Arizona 85013
Brian.Kelly@DignityHealth.org