
Deep Brain Stimulation & Focused Ultrasound
At a Glance: Our DBS and Focused Ultrasound Program
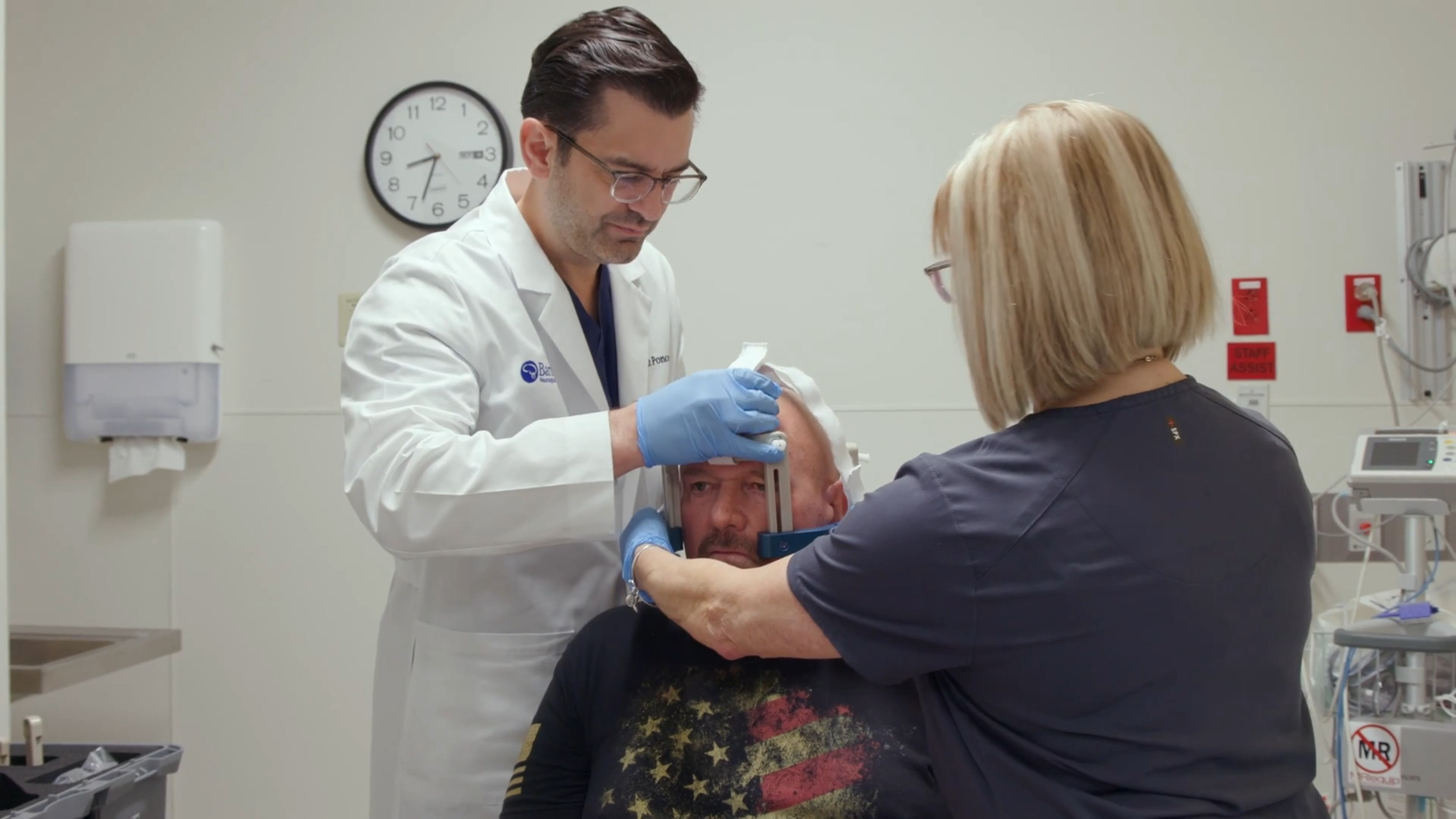
As an early adopter of and national leader in deep brain stimulation (DBS) and focused ultrasound, we offer treatment for tremor-dominant Parkinson’s disease, essential tremor, and dystonia. DBS involves placing an electrode in a targeted area of the brain to disrupt the neurons that cause these disorders, including epilepsy; meanwhile, focused ultrasound uses heat generated by sound waves to deactivate the neural circuits responsible for a smaller scope of movement disorders.
No matter the treatment you’re pursuing, our doctors and clinicians make it a priority to establish a lasting relationship; from your first encounter to before and after each procedure or clinic visit. At Barrow, we not only want to ensure a great outcome—we want a considerable improvement in your quality of life, too.
To learn more or schedule an appointment, please give us a call at (602) 406-3865.


The Barrow Difference
Ease of Becoming a Patient
Our neurosurgeons and neurologists have widespread experience that can be hard to find in the emerging field of neuromodulation, and as the recipient of generous donations, we’re able to keep innovating as we research even more uses for neuromodulation technology and continue our clinical trials.
Even better: You or your loved one can access the Barrow Deep Brain Stimulation and Focused Ultrasound Program at any point; whether you’re initially evaluating either procedure or if you’ve decided to undergo treatment and have completed the necessary medical preparation. Finally, we offer free weekly DBS and focused ultrasound education classes to patients considering either procedure in our community—you don’t have to be a patient with us to attend (individual and Spanish-speaking classes can also be arranged).

Surgery While You Sleep
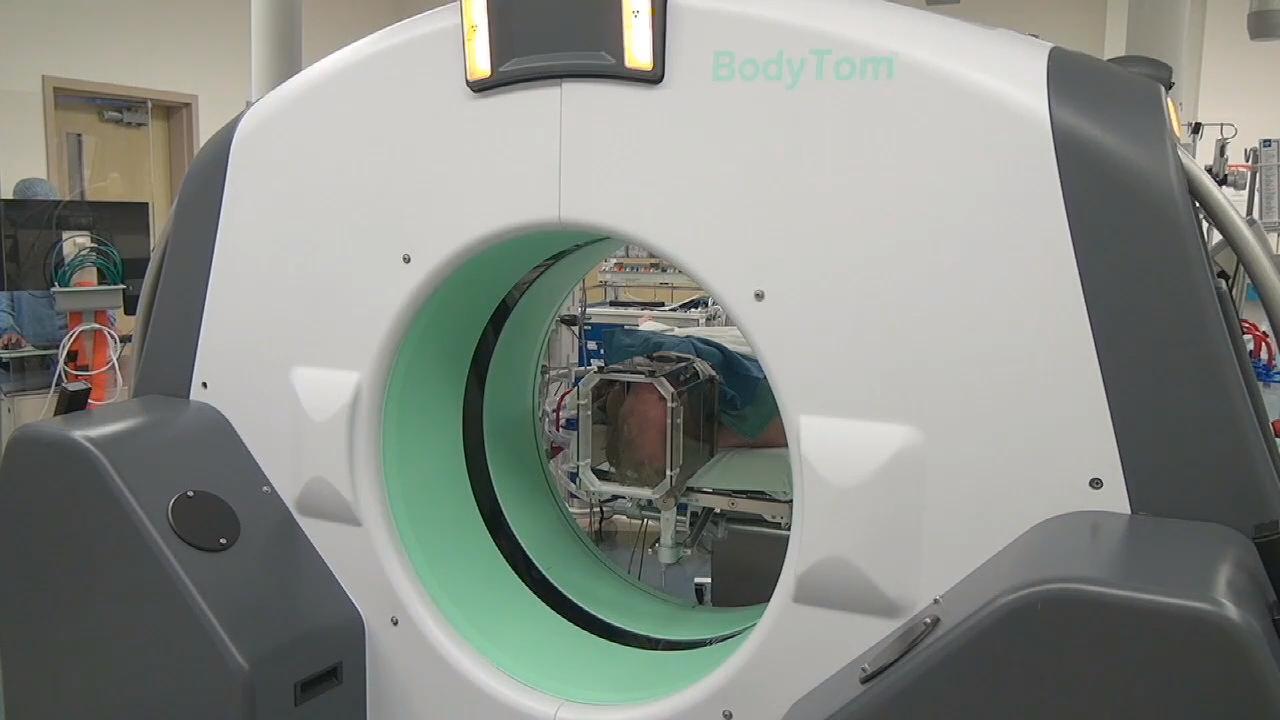
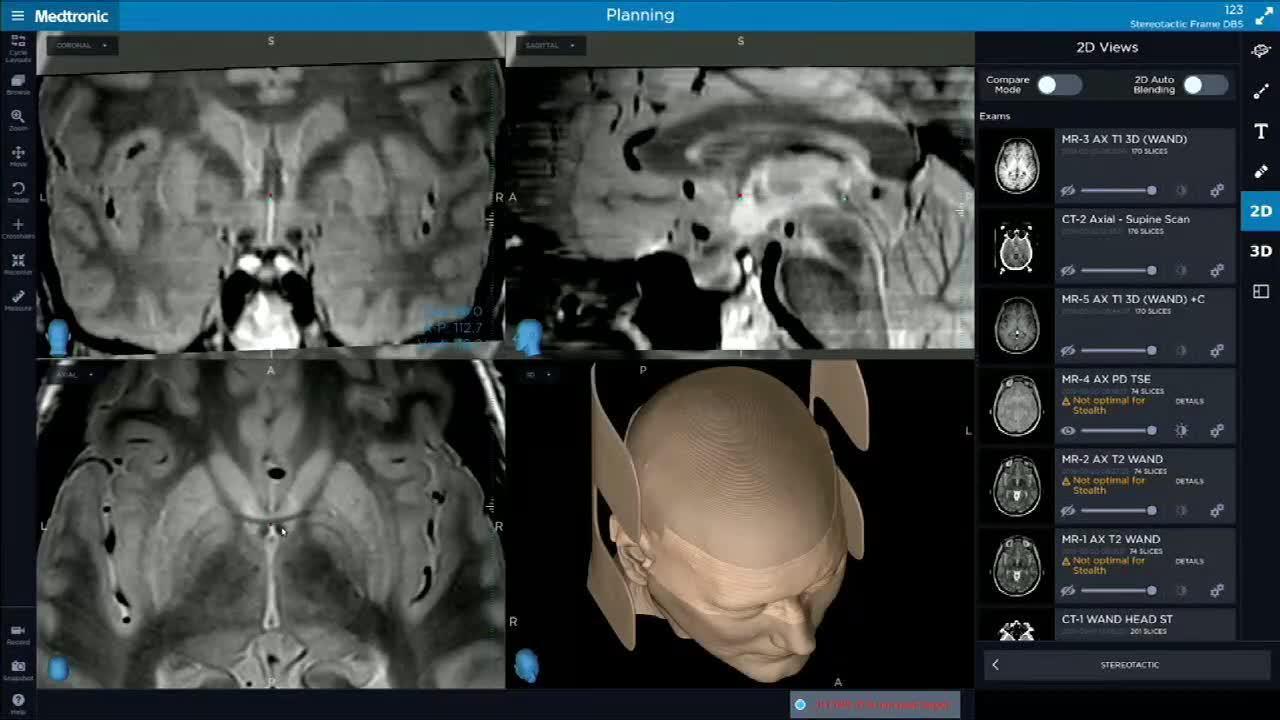
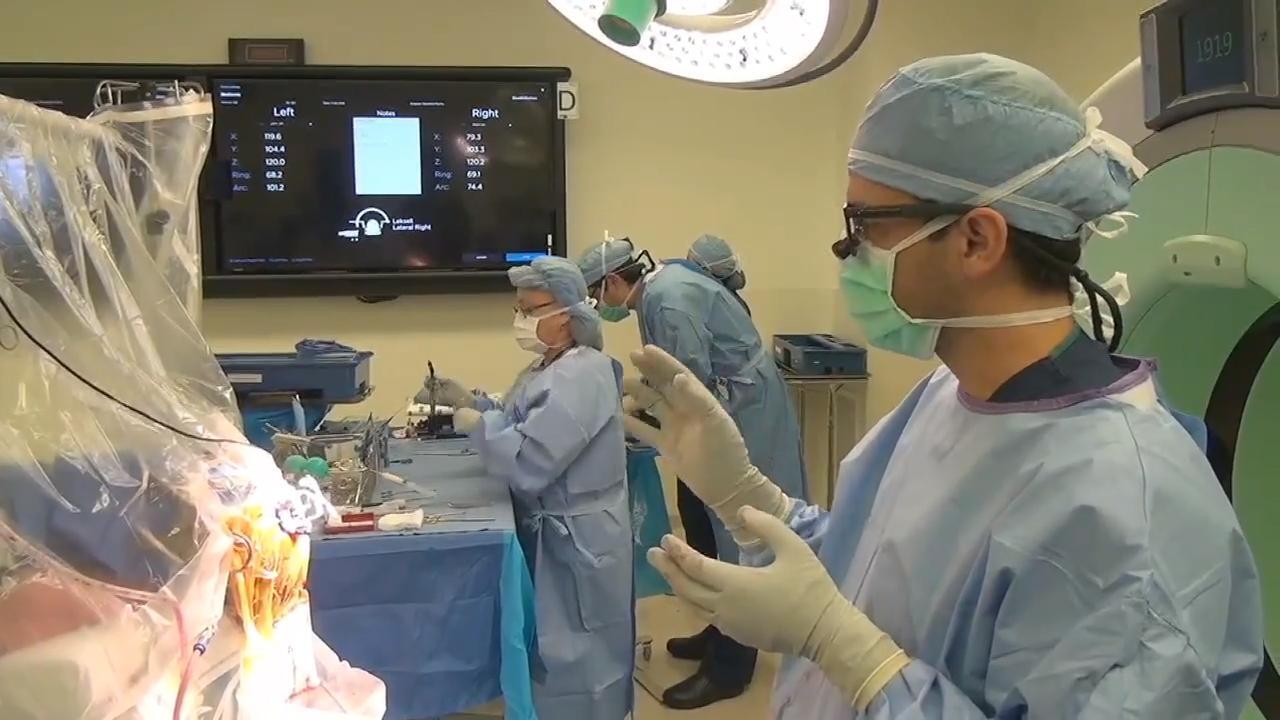
Advancements in imaging and computer-guided neurosurgery have made it possible to perform DBS surgery under general anesthesia. (Previously, patients had to remain awake, but sedated.) Asleep DBS surgery offers multiple benefits over traditional awake DBS surgery, including:
- Greater patient comfort
- No need to stop Parkinson’s medications before surgery
- Decreased duration of the surgical procedure
Navigating Travel and Accommodations
Given that many of our DBS and focused ultrasound patients come to us from beyond Arizona’s borders, our goal is to make your trips to Phoenix as efficient as possible. Our program coordinators assist you with all of the appointments needed for preoperative evaluation, surgery, follow-up care, and programming of your stimulator after surgery over a condensed timeframe.
Our Patient Connect Program
Our Patient Connect Program does exactly that: it connects people just like you who are considering surgery to those who have undergone DBS or focused ultrasound procedures. If you’re interested in joining this program, our coordinator will help link you up with patients who are eager to share their experiences.
To learn more or schedule an appointment, please give us a call at (602) 406-3865.
What We Treat
Dystonias
Epilepsy
Essential Tremor
Major Depressive Disorder
Parkinson's Disease

"When they pulled me out of the MRI, I was laughing. I was clapping my hands. That was it, a miracle."

"It changed our lives just having that first DBS surgery because he was able to feed himself. He was able to button his own clothes and take care of himself."

"With Parkinson’s, you have everything taken away from you. DBS surgery opened a whole new door. It gave me back a lot of my life."

“It’s been an amazing experience. From the time we started all the way through surgery, it went as planned."
Tests, Treatments & Procedures
Deep Brain Stimulation (DBS) Surgery
Focused Ultrasound for Parkinson's and Essential Tremor
Laser Interstitial Thermal Therapy (LITT)
Responsive Neurostimulation (RNS)
Stereoelectroencephalography (SEEG)
Stereotactic Laser Ablation
Vagus Nerve Stimulation (VNS)
Specialists
Location

Support & Wellness
Videos

Geoff Oldfather: Focused Ultrasound for Essential Tremor

Patrick Scott - DBS for Essential Tremor

Barrow Patient John Wagner on DBS Surgery
Nancy: I'm Thankful for Beating Essential Tremor
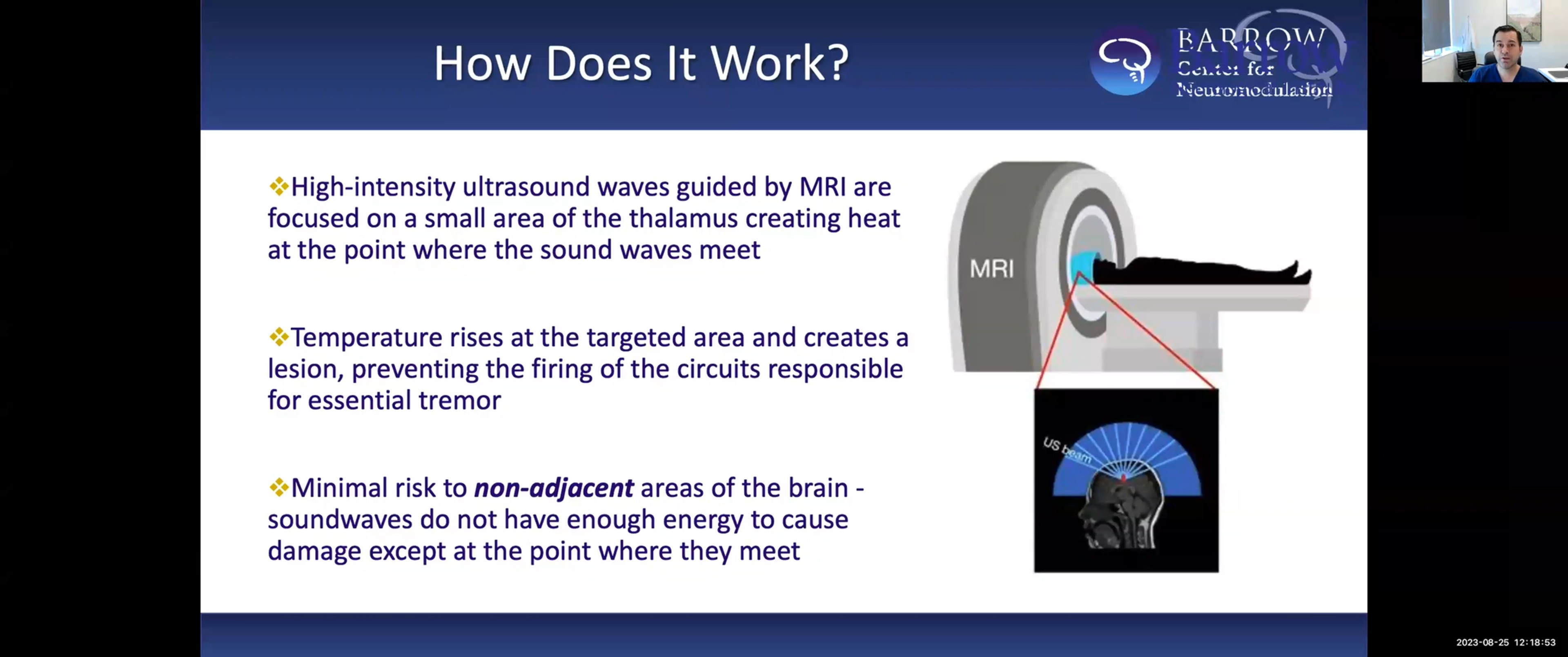
Focused Ultrasound for Essential Tremor and Tremor-Dominant Parkinson's Disease
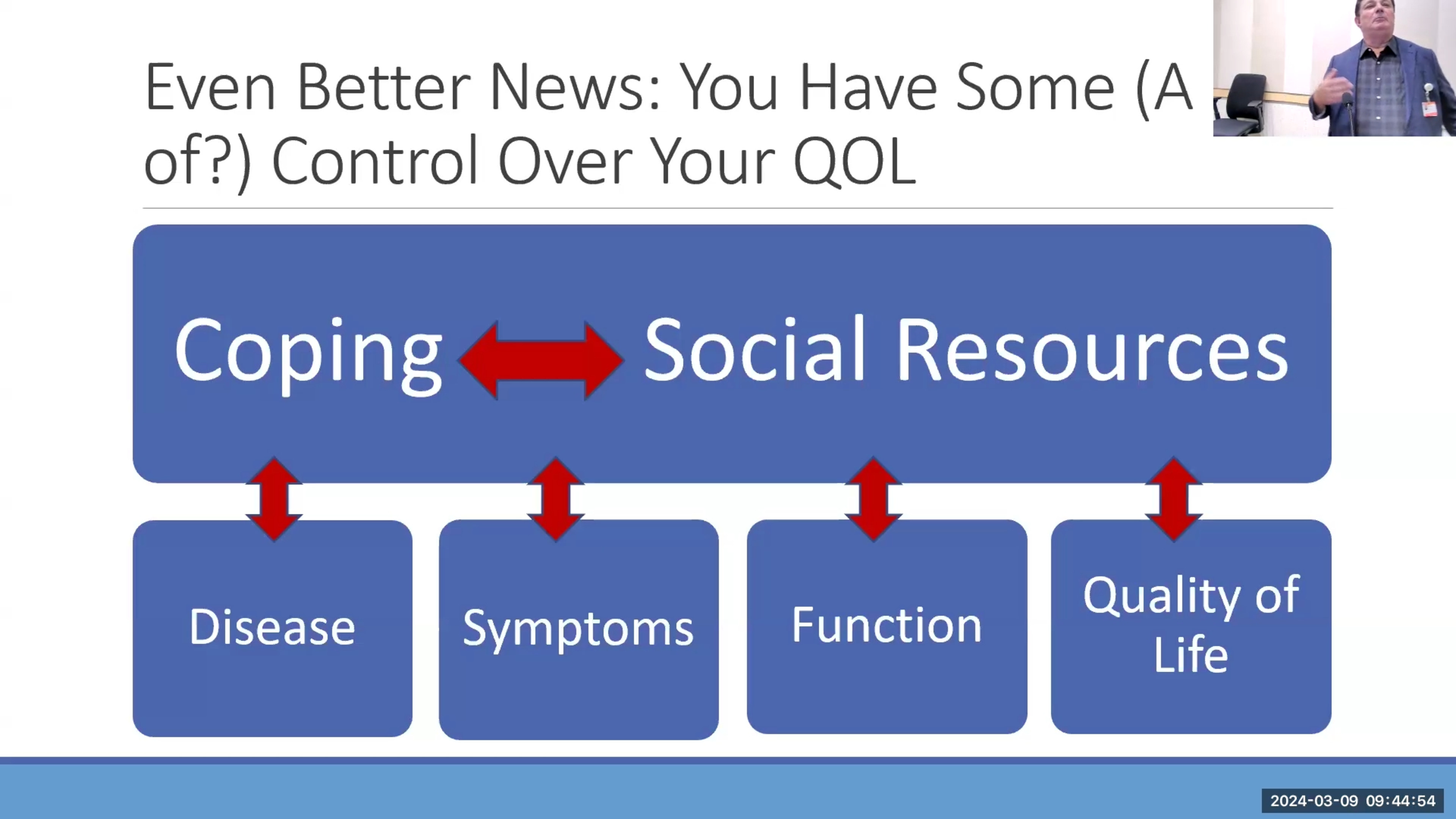
Essential Tremor Conference 2024

Dr. Holly Shill - Programming a Neurostimulator

Asleep DBS Part 1: Frame Placement

Asleep DBS Part 2: Incision Planning

Asleep DBS Part 3: Lead Placement

Asleep DBS Part 4: Verification

Minding What Matters Most®




























