Gigantism
Overview
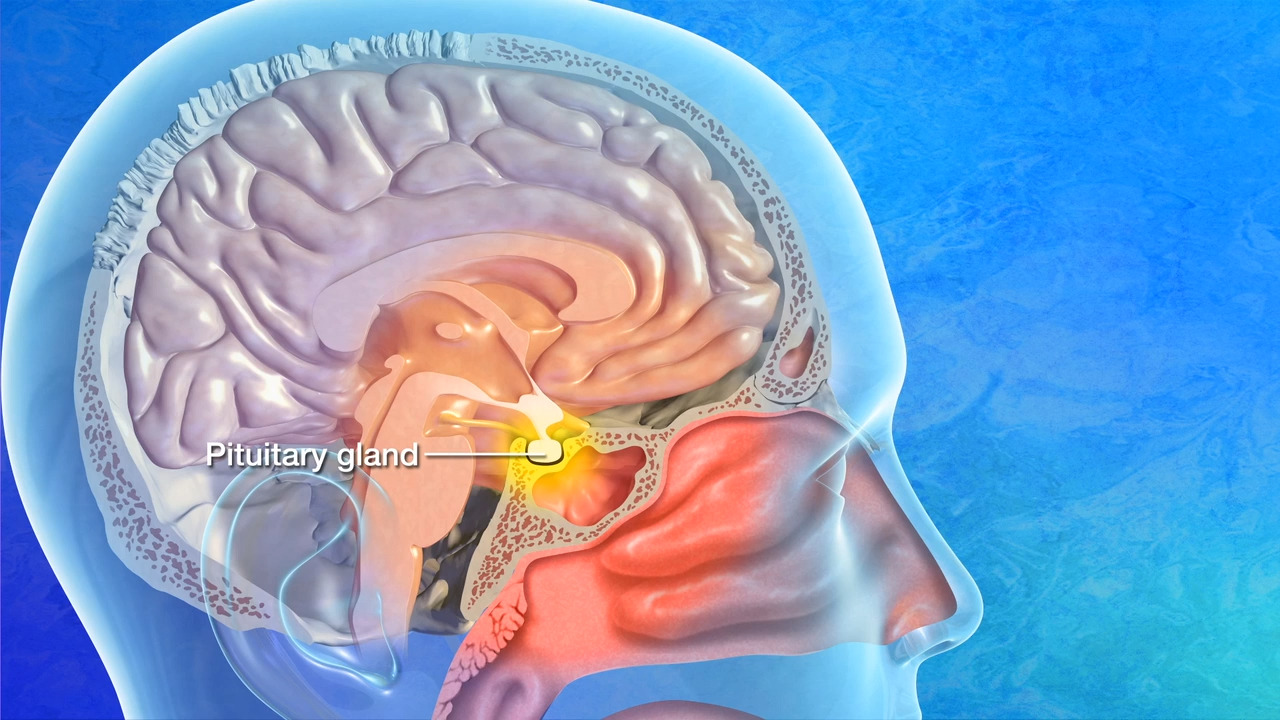
Gigantism is a rare condition in which your body produces too much GH, more than needed for your age. This happens because of a benign tumor on the small gland at the base of the brain called the pituitary gland.
Here are some symptoms you might notice if you or someone you know has gigantism:
- Unusually Rapid Growth: You may grow much taller than your peers in a short amount of time.
- Large Hands and Feet Your hands and feet might grow out of proportion with the rest of your body.
- Thickening of Facial Features: Your jaw, nose, and lips may become more pronounced.
- Joint Pain: You might experience unusual pain and discomfort in your joints because of their enlargement.
- Delayed Puberty: In some cases of gigantism, puberty can start later than usual.
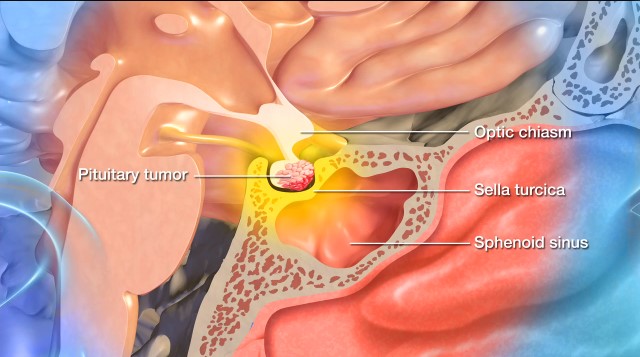
- Vision Problems: If the tumor on your pituitary gland presses against the optic nerves, it can cause visual impairment and occasionally blindness.
- Headaches: Due to pressure from the tumor, frequent and persistent headaches can occur.
- Excessive Sweating: Excessive GH can cause thick, coarse, oily skin, skin tags and sweating too much.
- Fatigue: Sleep apnea is common in people with gigantism and this can result in extreme fatigue and daytime sleepiness.
It’s important to address these symptoms early on. If you notice any of these symptoms, it’s a good idea to consult a doctor for further evaluation. With proper medical attention, like surgery or medication to control hormone levels, many of the effects of gigantism can be treated or effectively managed.
Gigantism Diagnosis
Gigantism can be challenging to diagnose because growth rates vary significantly from child to child, and, as a whole, the condition is exceptionally rare.
In general, gigantism may be indicated when a child’s height is three standard deviations above the average for their sex and age, plus two standard deviations above the adjusted average height of their biological parents. Elevated growth hormone (GH) levels and insulin-like growth factor-1 (IGF-1) in the blood can confirm the diagnosis. This is the most common diagnostic tool and typically involves two tests done together:
- IGF test. While levels of GH in the blood fluctuate throughout the day, a predictable way to track GH is by measuring the level of IGF-1 in the blood. In most cases, a high IGF-1 level will suggest a gigantism diagnosis.
- Oral glucose tolerance test. To confirm a gigantism diagnosis, an oral glucose tolerance test can be ordered. Your child will ingest a sugary liquid, and then a medical professional will test their blood every half hour for two hours to measure GH levels. Typically, the drink’s high sugar content will cause the GH levels to fall, but when too much GH is being made, these levels do not decrease appropriately, which confirms the diagnosis.
Once the diagnosis is confirmed, an MRI of the pituitary gland is used to determine the size and location of the tumor.

Gigantism Symptoms
Gigantism is a rare condition in which your body produces too much GH, more than needed for your age. This happens because of a benign tumor on the small gland at the base of the brain called the pituitary gland.
Here are some symptoms you might notice if you or someone you know has gigantism:
- Unusually Rapid Growth: You may grow much taller than your peers in a short amount of time.
- Large Hands and Feet Your hands and feet might grow out of proportion with the rest of your body.
- Thickening of Facial Features: Your jaw, nose, and lips may become more pronounced.
- Joint Pain: You might experience unusual pain and discomfort in your joints because of their enlargement.
- Delayed Puberty: In some cases of gigantism, puberty can start later than usual.
- Vision Problems: If the tumor on your pituitary gland presses against the optic nerves, it can cause visual impairment and occasionally blindness.
- Headaches: Due to pressure from the tumor, frequent and persistent headaches can occur.
- Excessive Sweating: Excessive GH can cause thick, coarse, oily skin, skin tags and sweating too much.
- Fatigue: Sleep apnea is common in people with gigantism and this can result in extreme fatigue and daytime sleepiness.
It’s important to address these symptoms early on. If you notice any of these symptoms, it’s a good idea to consult a doctor for further evaluation. With proper medical attention, like surgery or medication to control hormone levels, many of the effects of gigantism can be treated or effectively managed.
Gigantism Treatments
The goal of treatment for gigantism is to normalize GH and IGF-I levels to stop excessive growth and prevent further complications from gigantism.
Surgery
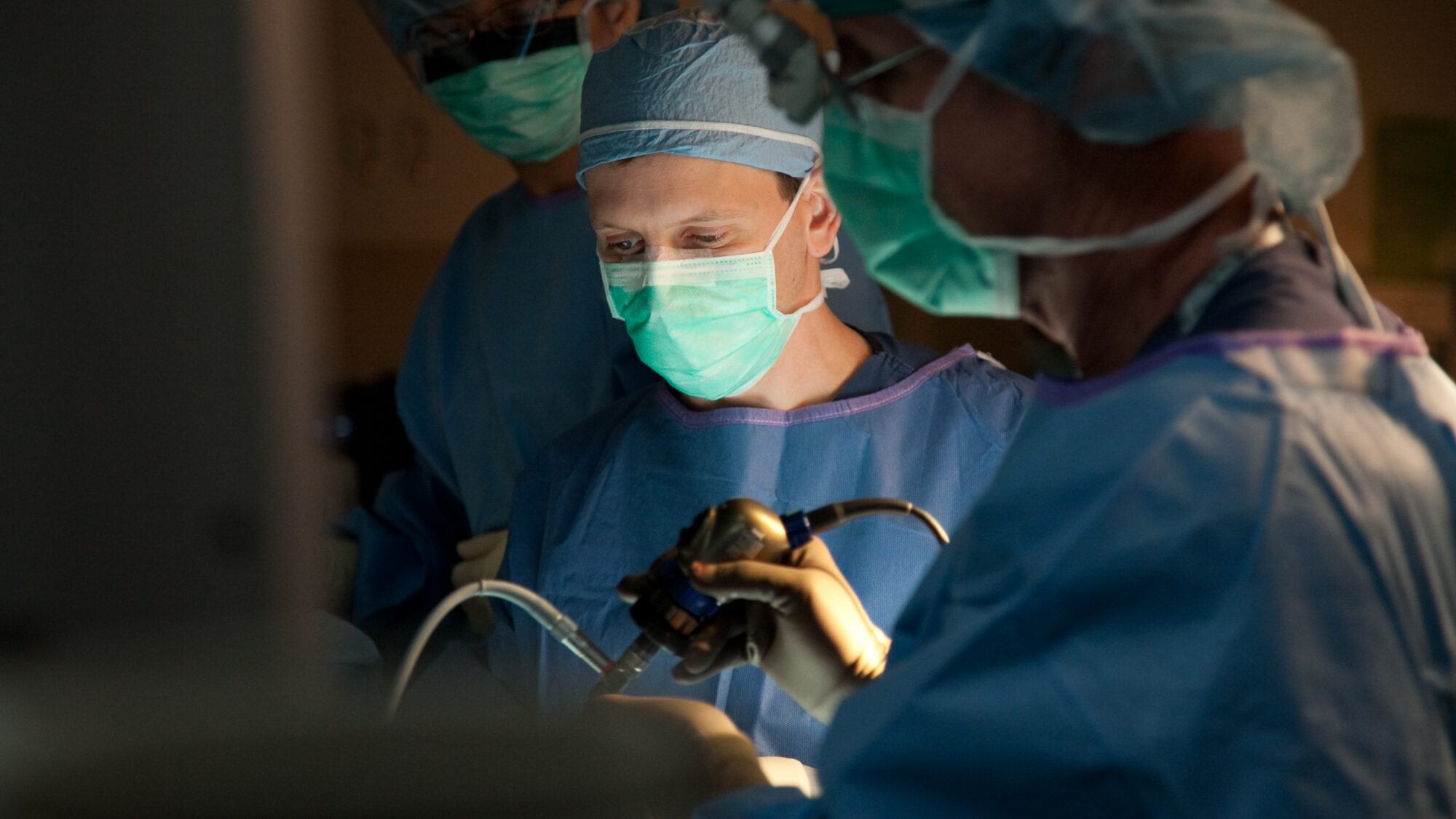
Surgery is the preferred, first line form of treatment and the only method for reaching a true cure for gigantism. Your neurosurgeon will access the pituitary gland using the transsphenoidal approach, so named because the surgeon uses the sphenoid sinus behind the nose for the procedure.
Using precise instruments, your neurosurgeon will enter your nostrils and create an opening in the sphenoid bone. Further openings will be made until a hole is created in the sella turcica, the bone that cradles and protects the pituitary gland.
Once the tumor appears in the operative field, careful removal occurs. Your neurosurgeon will use high magnification to help distinguish the tumor from normal pituitary tissue. When the tumor has been removed, the tumor cavity is cleaned and sealed off. Barrow neurosurgeons do not make external facial incisions on your face, and our patients do not experience bruising. In fact, most patients can return home the day after their surgery.
Our pituitary neurosurgeons specialize in endoscopic pituitary surgery. Endoscopic pituitary surgery uses a tiny camera to enter the nostrils to remove the tumor. The surgery aims to minimize trauma to the tissue surrounding the pituitary gland while facilitating a speedy recovery with as little discomfort or pain as possible.
Pharmacological Treatment and Hormone Therapy
Treatment with prescription medication is possible if surgery does not cause remission in your child’s gigantism or if surgery is not recommended due to other reasons specific to your child. Medicines are also sometimes prescribed prior to surgery to improve the likelihood of a good outcome.
- Octreotide or lanreotide are the two synthetic forms of the hormone somatostatin that stops GH release. These medications are often effective for the long-term control of gigantism, but can only be administered by a large injection every four weeks. Due to the side effects of these drugs as well as their expense, surgery is generally preferred.
- Bromocriptine and cabergoline are from a class of drugs called dopamine agonists. They can lower IGF-1 and GH levels in close to a third of the people treated with them—although symptoms could improve even if IGF-1 and GH levels do not decrease. Although not as effective as the synthetic hormones octreotide and lanreotide, they’re less expensive and more convenient to administer, as no injection is required. They can be combined with octreotide in some children with no adverse long-term health effects.
- Pegvisomant is a drug that blocks the action of GH at the level of GH receptors in various parts of the body, thereby lowering IGF-1 levels. It must be administered daily by subcutaneous or beneath-the-skin injection. Pegvisomant is an option if your child doesn’t respond to surgery or other medications.
Radiosurgery
Gamma Knife radiosurgery is a kind of radiation therapy that achieves results similar to those in the traditional surgical techniques described above. The ‘knife’ in this surgery is made up of many small beams of radiation focused on a very specific single point at the base of the skull where the pituitary gland resides. Each beam is too weak to damage healthy tissue, but at the point where the beams converge, they deliver a dose of radiation that’s lethal to the tumor. Gamma Knife is an outpatient procedure, does not involve any incisions, and requires only brief sedation under general anesthetic. However, it can take several years for GH levels to return to normal with Gamma Knife rather than days or weeks with traditional surgery. As a result, it’s often a last resort treatment after surgery and medications. Also, there are additional considerations for pediatric Gamma Knife surgery.
Common Questions
How common is gigantism?
Gigantism is an extremely rare condition that only occurs in children and adolescents. Around 100 cases have been reported in the United States, and they occur at a male-to-female ratio of two-to-one.
What is the difference between gigantism and acromegaly?
Gigantism and acromegaly are both conditions that are a direct result of excess GH. The difference between the two conditions is who they affect: children and adolescents who are still growing develop gigantism, while adults who have finished growing and have their growth plates fused develop acromegaly.
Gigantism is much less common than acromegaly.
What is the prognosis for those diagnosed with gigantism?
Generally speaking, those diagnosed later in life—e.g., adults with acromegaly—tend to experience more complications than those who are diagnosed at a younger age. This could be a result of a longer exposure to excessive GH and IGF-1.
The outlook for children and adolescents diagnosed with gigantism depends on how early or late they’re diagnosed and how effective their treatments are at managing excessive GH levels. If you’re noticing unexpected or unusual changes in your child’s growth or physical features, it’s critical you seek out your child’s healthcare professional as soon as possible.
Can gigantism be prevented?
While early diagnosis is crucial, there aren’t any preventative options. That said, prompt treatment can prevent or slow the excessive growth changes that gigantism can cause.