
Pituitary Microadenoma
At a Glance
- A pituitary microadenoma is a benign tumor of the pituitary gland measuring less than 10 mm.
- Many are asymptomatic, but they can cause tiredness, headaches, nausea, dizziness, vision problems, and symptoms related to hormone changes.
- For asymptomatic tumors, your doctor may recommend monitoring it with regular imaging. Symptomatic tumors may be treated with medications, surgery, radiation, or a combination of all three.
Overview
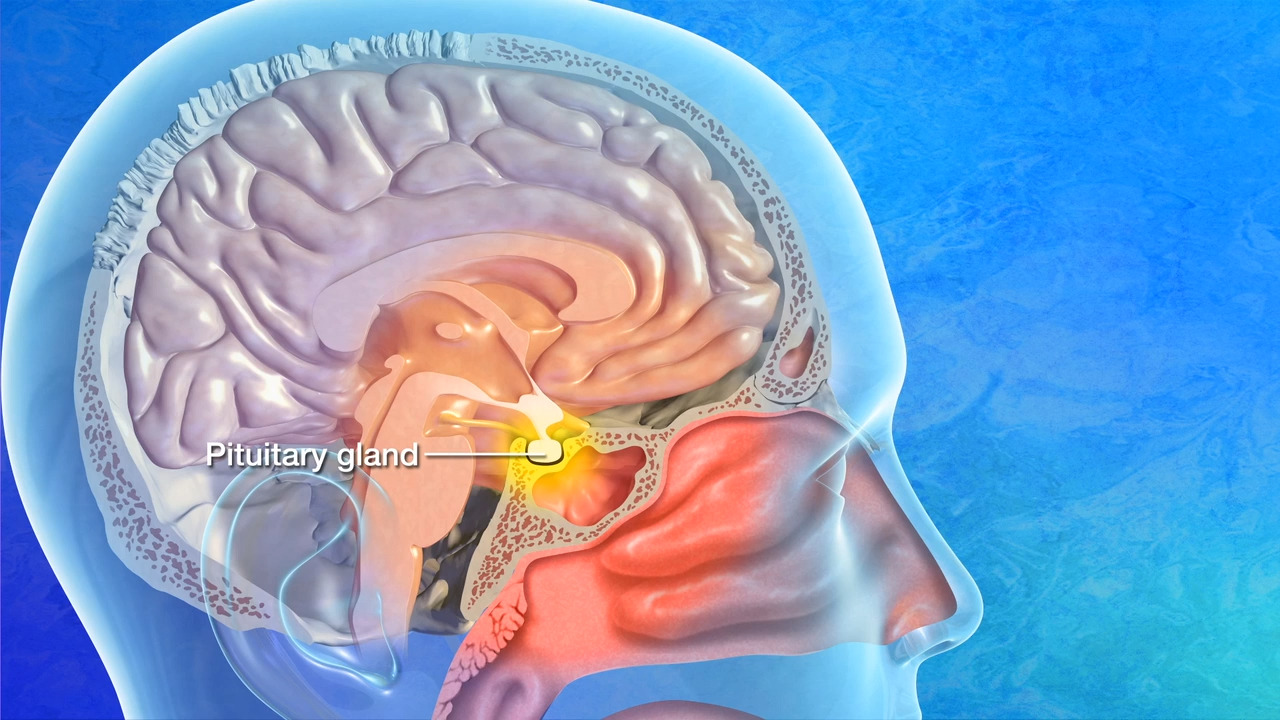
A pituitary microadenoma is a tiny, benign tumor on the pituitary gland that measures less than 10 millimeters (mm) or 1 centimeter. A critical pea-sized organ at the base of the brain, the pituitary gland is responsible for regulating growth, development, metabolism, and reproduction.
Pituitary microadenomas are the most common type of pituitary tumor, and doctors categorize them as functioning or nonfunctioning. Functioning microadenomas make hormones, while nonfunctioning adenomas don’t. Most pituitary tumors—including microadenomas—are benign, noncancerous, and nonfunctioning.
Pituitary microadenomas are a subset of pituitary adenomas, with pituitary macroadenomas describing tumors larger than 1 centimeter. Most adenomas grow slowly and rarely spread to other parts of the body.

What causes a pituitary microadenoma?
The precise cause of pituitary microadenoma is not well understood. We know that they develop when DNA mutations cause cells in the pituitary gland to grow and divide uncontrollably.
In rare cases, pituitary tumors can be caused by genetics, as a small percentage of pituitary tumors run in families. For example, individuals diagnosed with Multiple Endocrine Neoplasia type 1 (MEN1) may be at an increased risk of developing pituitary tumors like microadenomas.
Other factors thought to contribute to microadenoma development:
- Age and gender: Pituitary microadenomas occur more commonly in adults and women, which suggests that hormones related to gender can influence the growth of functioning microadenomas, or tumors that make hormones.
- Hormonal imbalance: Abnormal hormone levels can overstimulate pituitary cell growth, leading to tumor growth. For example, an excess of growth hormone (GH) can promote the development of a growth hormone-secreting microadenoma.

Pituitary Microadenoma Symptoms
Most pituitary microadenomas don’t cause symptoms. They are often found incidentally during an imaging test, like an MRI, that is performed for an unrelated reason.
If a microadenoma is not causing symptoms, it typically doesn’t need treatment. However, pituitary microadenomas are more likely than macroadenomas to be functioning tumors, which can cause hormone imbalances that create several symptoms.
If you have a microadenoma, symptoms you might notice include:
- Tiredness: Fatigue is a frequent symptom, as microadenomas can cause hormone reduction and overproduction. This lack of hormones for energy regulation or an excess of a hormone like prolactin can lead to fatigue.
- Headaches: These can result from the microadenoma compressing pituitary tissue, causing changes in intracranial pressure, or triggering hormonal imbalances.
- Nausea and vomiting: Although small, microadenomas can cause a localized increase in pressure on the brain, which can cause nausea and vomiting.
- Dizziness: Pressure on nearby brain structures, hormonal imbalances, and secondary effects on blood pressure can all lead to dizziness.
- Vision problems: Due to pressure on the optic nerve, vision problems are common with microadenomas. Loss of peripheral vision can occur.
- Menstrual or breast changes: High levels of prolactin due to a functioning microadenoma can result in changes to the menstrual cycle and breast growth.
- Unexplained hair growth or loss: Lowered or heightened levels of certain hormones, like ACTH, can cause hair growth or loss.
It’s important to note that these symptoms can overlap with those caused by other conditions. If you’re feeling concerned by any of these, you should seek an appropriate diagnosis from your healthcare provider.
Pituitary Microadenoma Diagnosis
A pituitary microadenoma can be diagnosed through various tests and imaging studies, starting with a review of your personal and family medical history.
A microadenoma diagnosis often includes several of the following:
- Physical and neurological exam: First, your healthcare provider will ask about your overall health and symptoms that might suggest a pituitary microadenoma, like headaches, fatigue, menstrual irregularities, or other symptoms of hormone excess or deficiency. Next, they’ll complete an examination to assess your neurological function, including reflexes, coordination, strength, and sensation.
- Blood tests: Blood tests are done to measure hormone levels. They can check for excess or deficient levels of pituitary hormones and the hormones of glands regulated by the pituitary gland, like cortisol, thyroid, prolactin, and sex hormones.
- Magnetic Resonance Imaging (MRI): An MRI is the primary imaging test to diagnose pituitary tumors. It uses detailed images of the brain to identify the tumor’s location, size, and characteristics. An MRI can reliably detect a growth larger than four millimeters. More sensitive MRI machines may detect even smaller microadenomas.
- Computed Tomography (CT): Although an MRI is usually the first choice in neuroimaging, a CT scan can help evaluate tumor size and location by creating detailed cross-sectional brain images via X-ray images.
- Urine test: A urine test can help diagnose a microadenoma that’s producing too much of the hormone ACTH. This leads to excess cortisol in the body and causes Cushing’s disease.
- Visual field tests: A microadenoma can affect eyesight, especially peripheral vision, so a visual test to check how well you’re seeing can help your provider decide if you need other tests.
After collecting any of these tests or imaging results, your neurologist or endocrinologist will make their diagnosis and begin to develop a treatment plan.

Pituitary Microadenoma Treatment
Doctors have several options for treating a pituitary microadenoma: the tumor may be removed with surgery, controlled with radiation therapy, or managed with medicine. Your healthcare provider may suggest a combination of the following treatments. Also, because microadenomas are usually benign and slow-growing, your treatment may consist of ongoing observation.
Surgical Treatment
Surgery is the first line of treatment and the only method for reaching a true cure for microadenomas.
Your neurosurgeon will access your pituitary gland using the transsphenoidal approach, so named because it uses the sphenoid sinus behind the nose as a corridor to access the pituitary gland. Using special instruments, your neurosurgeon will enter the nasal cavity and create an opening in the sphenoid bone. Further openings will be made until a hole is created in the sella turcica, the bone that cradles and protects the pituitary gland.
Once the tumor appears in the operative field, your neurosurgeon will use high magnification to help distinguish it from normal pituitary tissue. Then, after removal of the microadenoma, the tumor cavity is cleaned and sealed off.
At Barrow Neurological Institute, our surgeons specialize in endoscopic pituitary surgery. This procedure uses a tiny camera to enter the nostrils and remove the tumor. It aims to minimize trauma to the tissue surrounding the pituitary gland while facilitating a speedy recovery. Our neurosurgeons do not make external incisions on the face, and bruising is uncommon. Most patients can return home the day after their surgery.

Nonsurgical Treatments
Your doctor might suggest these nonsurgical treatments on their own or in conjunction with surgery:
- Medication: Medication helps lower the amount of hormones the body makes due to a microadenoma, and some medicines can shrink certain pituitary tumors. For prolactin-secreting microadenomas, most patients will choose to take medication to shrink their tumor and block the hormone effects in the body. For microadenomas that cause Cushing’s disease and acromegaly, surgery is the preferred treatment, as it’s more effective than medication.
- Radiosurgery: This treatment method relies on radiation delivery systems to focus radiation at the site of the microadenoma while minimizing the radiation dose to the brain. Doctors often use radiosurgery for tumor recurrence or if surgery and medication do not seem to be working. The two most common forms are:
- Gamma Knife radiosurgery: This technique destroys abnormal tissue using precise and focused radiation beams and is only lethal to cells where the beams meet. It is an outpatient procedure that doesn’t involve incisions and requires only brief sedation under general anesthesia.
- CyberKnife radiosurgery: This technique uses targeted energy beams to destroy tumor tissue while sparing healthy tissue. It uses image-guided robotics to deliver surgically precise radiation to help destroy tumors like microadenomas.
Common Questions
How common are microadenomas?
Pituitary microadenomas are relatively common—studies suggest they may be present in up to 10 to 20% of the general population. Physicians often discover microadenomas during imaging studies done for unrelated reasons.
Most microadenomas don’t cause symptoms. When they do, common problems include hormonal imbalances in the form of Cushing’s disease, prolactinoma, acromegaly, or visual disturbances.
Who gets microadenomas?
Doctors most often diagnose microadenomas in adults between 30 and 50, and those with genetic predispositions like multiple endocrine neoplasia type 1 (MEN1) and familial isolated pituitary adenomas (FIPA).
Some types of microadenomas, like prolactinomas, are more common in women and are particularly noticeable in those of reproductive age. Other types of hormone-secreting microadenomas, such as those causing Cushing’s disease or acromegaly, do not appear to have a gender preference.
What is the prognosis for people diagnosed with microadenoma?
The prognosis for those diagnosed with pituitary microadenoma is excellent—microadenomas are noncancerous, meaning they won’t spread to other parts of the body. A specific prognosis depends on the type of microadenoma, its size, whether it secretes hormones, and how effectively it responds to treatment.
In most cases, neurosurgeons can cure a microadenoma with endoscopic transsphenoidal surgery, a procedure in which a neurosurgeon accesses the tumor through the nasal passages and sphenoid sinus.
Can microadenoma be prevented?
There are no known methods to prevent pituitary microadenomas.
That said, you can take the following precautions if you’re at a higher risk due to family history:
- Genetic counseling and testing: Genetic counseling and testing can benefit those with a family history of conditions like Multiple Endocrine Neoplasia type 1 (MEN1) or Familial Isolated Pituitary Adenomas (FIPA). Early detection of these genetic predispositions makes room for monitoring and early intervention if needed.
- Regular monitoring: Individuals known to be at higher risk should have regular check-ups and watch for early signs of pituitary abnormalities. Early detection of hormone imbalances or symptoms can prompt diagnosis and treatment.
Can a microadenoma cause weight gain?
Yes, a microadenoma can cause weight gain. This depends on how the tumor affects the pituitary gland and the function of the tumor itself.



