Cavernous Malformation
At a Glance
- A cavernous malformation is a cluster of enlarged, thin-walled blood vessels that can leak or bleed into the brain or spinal cord.
- Symptoms typically begin when the lesion bleeds and vary depending on its size and location. They commonly include headaches, seizures, weakness, sensory changes, or vision issues.
- Management options include careful monitoring for low-risk, asymptomatic lesions or surgical removal for symptomatic lesions that bleed or grow.
Overview
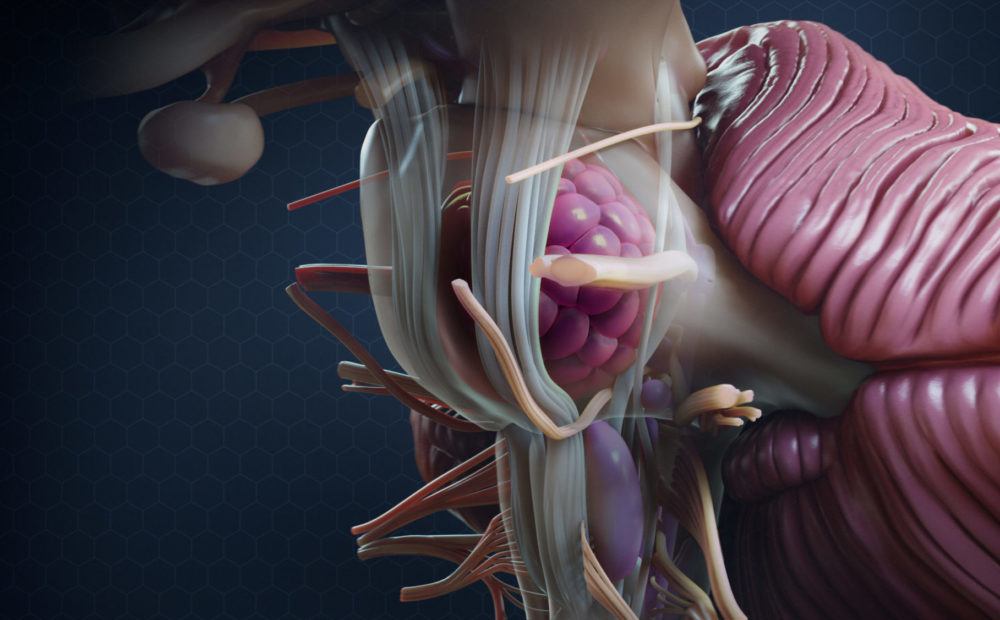
A cavernous malformation is a cluster of dilated blood vessels (capillaries) with an enlarged and irregular structure. The walls of these capillaries are thinner than normal, have loose junctions between cells, and are prone to leaking.
These abnormalities can occur anywhere in the body, but they are most likely to produce symptoms when they form in the brain or spinal cord. They can cause neurological symptoms when they bleed into the brain (hemorrhage).
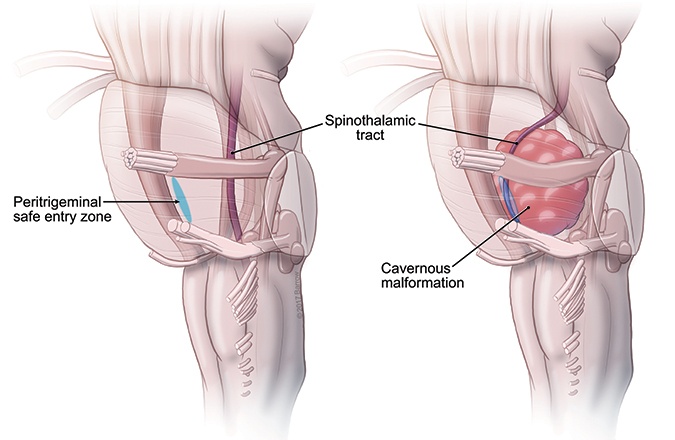
The severity of a cavernous malformation depends on two variables:
- Where it is located in the brain
- Its size, or how big it is
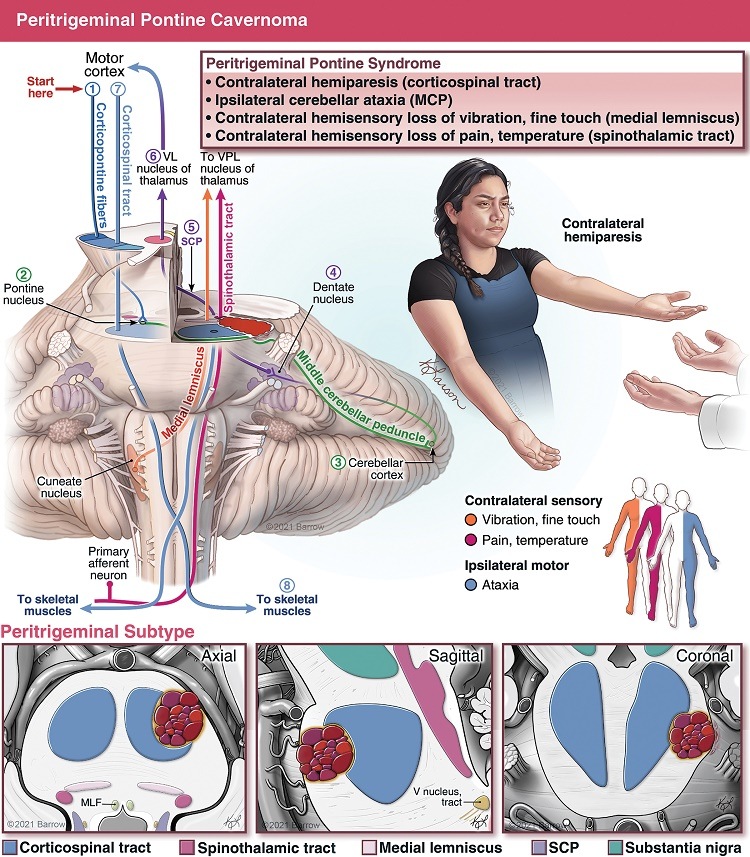
If it is in a critical spot, like the brainstem, a cavernous malformation is quite serious because any hemorrhage will impact a vital tract, nucleus, or circuit and can cause paralysis, breathing problems, or other neurological deficits. Large malformations are more likely to touch on an eloquent or critical structure. These can cause issues with speech, movement, or cognition.
The average size of a cavernous malformation is around one centimeter, or about half an inch. A cavernous malformation is considered giant if it is three centimeters or larger, or over an inch in diameter.
Synonyms for Cavernous Malformations
There are several other terms that describe cavernous malformations, including:
- Cerebral cavernous malformation (CCM)
- Cavernoma
- Cavernous angioma
- Cavernous hemangioma
Conversely, these lesions are not considered brain tumors.
A brain tumor is a neoplastic lesion where some cells divide and the mass is constantly growing, whereas cavernous malformations are an abnormal assembly of the normal vascular cells that can leak blood. This cluster of abnormally assembled cells will basically stay the same if left alone, and it only grows when it bleeds. The blood and fluid that accumulates can make it grow, but it is not the same as a tumor with cells that are dividing and growing in number.
Anatomy of the Cerebrovascular System
The cerebrovascular system is the network of blood vessels that supply your brain with oxygen and nutrients. The system includes the internal carotid arteries, vertebral arteries, and their branches, which bring blood into the brain, and the veins that carry blood out of the brain.
The carotid arteries are located in the neck and provide blood to the front part of the brain (known as the anterior circulation). The vertebral arteries are located at the back of the neck and provide blood to the back part of the brain (the posterior circulation). These arteries branch off into smaller blood vessels, which then supply different areas of the brain.
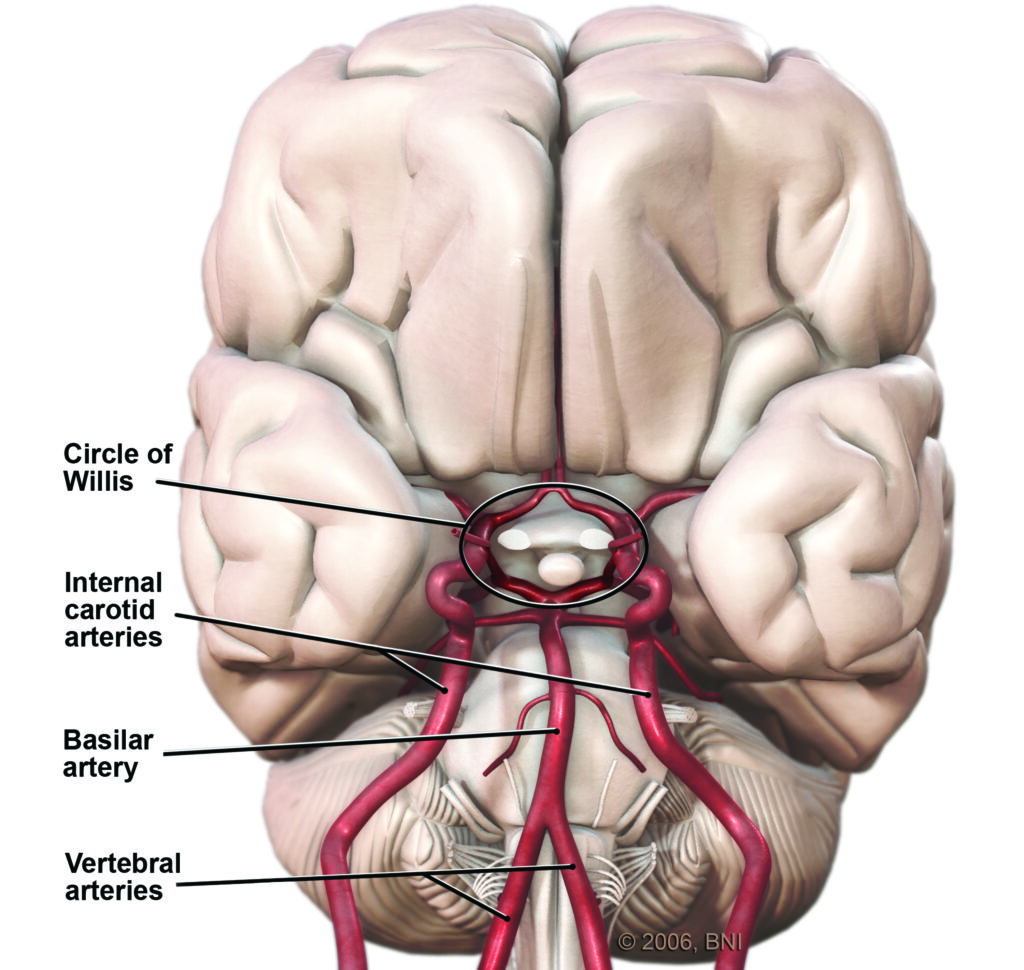
Within the brain, the smallest blood vessels are called capillaries, which have thin walls that allow for the exchange of oxygen and nutrients with brain cells. The capillaries then join together to form larger blood vessels called veins, which carry the blood back to the heart to be reoxygenated via the internal jugular veins. As mentioned above, cavernous malformations in the brain are part of this capillary network and contain dilated, enlarged, and weak vessels, that are prone to bleeding.
The cerebrovascular system is essential for the proper functioning of the brain. Any disruption of blood flow to the brain can cause serious health problems, such as stroke or cognitive impairment. Therefore, maintaining a healthy lifestyle and managing risk factors such as high blood pressure or diabetes is important for maintaining the health of the cerebrovascular system.

Cavernous Malformation Symptoms
When a cavernous malformation leaks, bleeding can be slow and intermittent or rapid, causing sudden symptom onset. Most people who develop neurological deficits after a hemorrhage improve dramatically over time. However, repeated hemorrhages may result in permanent neurological problems.
Symptoms of a cavernous malformation may include:
- Seizures
- Headaches
- Bleeding in the brain (hemorrhage)
- Hearing or vision changes
- Weakness, numbness, or paralysis
- Memory deficits
- Speech impairment
- Unsteadiness
It is not common for cerebral cavernous malformations to cause fatigue.
Cavernous Malformation Treatment
If you are diagnosed but not experiencing symptoms, your doctor may recommend observing the malformation over time with regular MRI scans.
Medications, such as anti-epileptic drugs, may be prescribed to control your seizures or other symptoms.
Surgery
If your symptoms are not responding to medication or there is repeated bleeding in the brain, removal via neurosurgery may be recommended.
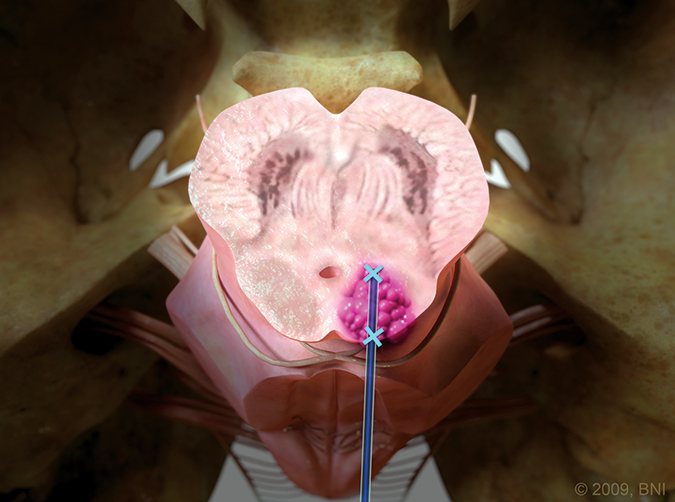
Not all cerebral cavernous malformations need to be removed surgically. If it has not bled before, then there is approximately a 1-4% chance each year that it will hemorrhage.
Conversely, cavernomas that have bled before have a higher chance of bleeding again in a given year. A cavernous malformation that shows behavior suggesting it is more likely to continue to bleed and cause harm should be removed. If a lesion is quiet and behaving well, then it is sometimes best left alone.
Cavernous malformations can be cured by complete surgical removal.
Common Questions
How common are cavernous malformations?
About one person in every 100 to 200 people has a cerebral cavernous malformation, but about 25% of people affected never have symptoms.
These lesions can affect children and adults. Most people who have symptoms are between 20 and 50 years old.
Most occur without any single identifiable cause, but in some cases they can be inherited genetically from your mother or father.
How are they diagnosed?
Cerebral cavernous malformations are mainly diagnosed by magnetic resonance imaging (MRI). They have a telltale characteristic appearance on MRI.
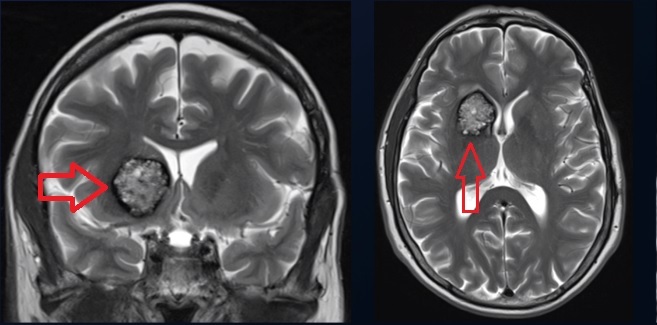
Are cavernous malformations life-threatening?
These lesions usually are not life-threatening, but repeated bleeds may cause permanent neurological deficits. Malformations in sensitive tissue like the brainstem and thalamus can be extremely disabling if they bleed.
Do they go away?
They do not go away without surgical removal. However, they may go dormant and stop bleeding. It is difficult to predict which lesions will bleed again and when.
Is a cavernous malformation a tumor?
These lesions are better described as abnormally formed blood vessels. They are not tumors in the sense of multiplying cells and growing tissue. They do not spread to other parts of the body and infiltrate organs like cancerous tumors.
Are they hereditary?
Most of cavernous malformations are classified as sporadic cavernous malformations, meaning there is no known family history of the disease. However, 15% are caused by inherited genetic mutations. There are known as familial cavernous malformations.
Can a cavernoma cause memory loss?
Yes, a cavernous malformation can cause memory loss if it is located in, or nearby, the part of the brain that controls memory.
What is the difference between a cavernous malformation and an aneurysm?
An aneurysm is a sac or balloon-like outpouching on the artery in the brain that can burst and result in high-pressure bleeding, whereas cavernous malformations are abnormally assembled capillaries and veins that have a low-pressure leakage, or ooze. An aneurysm is arterial; a cavernous malformation is capillary and venous, so they have a very different bleeding profile.
Can you take ibuprofen with a cavernous malformation?
Yes, you can take ibuprofen with a cavernous malformation. While ibuprofen is a blood thinner, it will not cause it to bleed, or make it bleed more frequently.
However, if a cavernous malformation were to bleed while a person is taking ibuprofen, it might bleed slightly more because the platelets (the cell fragments in your blood that promote clot formation) are slightly inhibited.
Can you drive with a cavernous malformation?
It is possible to drive if you have a cavernous malformation. However, some patients with a cavernous malformation have seizures. If you have experienced a seizure that has been reported to the department of motor vehicles (DMV) or a similar regulatory agency, your license usually will be suspended for six months. A person must show that they have been seizure free for six months before their driver’s license can be reinstated. Seizures can typically be controlled by taking an anticonvulsive medication.
By and large, seizure-producing cavernous malformations are located in the cerebrum. Cavernous malformations in the brainstem or cerebellum don’t produce seizures and tend not to be a driving risk.
Can you exercise with a cavernous malformation?
Yes, you can exercise with a cavernous malformation.
Are there activities you should avoid with a cavernous malformation?
No, there are no activities you should avoid if you have been diagnosed with a cavernous malformation. You may have been told that you shouldn’t lift heavy weights, as it somehow predisposes your cavernoma to bleeding, but there is no evidence for that.
Can some things make you more likely to have a cavernous malformation?
A cavernous malformation is a random event. While some cavernous malformations can be caused by a genetic disposition, most are sporadic and not caused by anything under your control.
Resources
Alliance to Cure Cavernous Malformation
American Association of Neurological Surgeons
National Organization for Rare Diseases (NORD)
National Library of Medicine – Medline Plus
National Institute of Neurological Disorders and Stroke (NINDS)
Videos
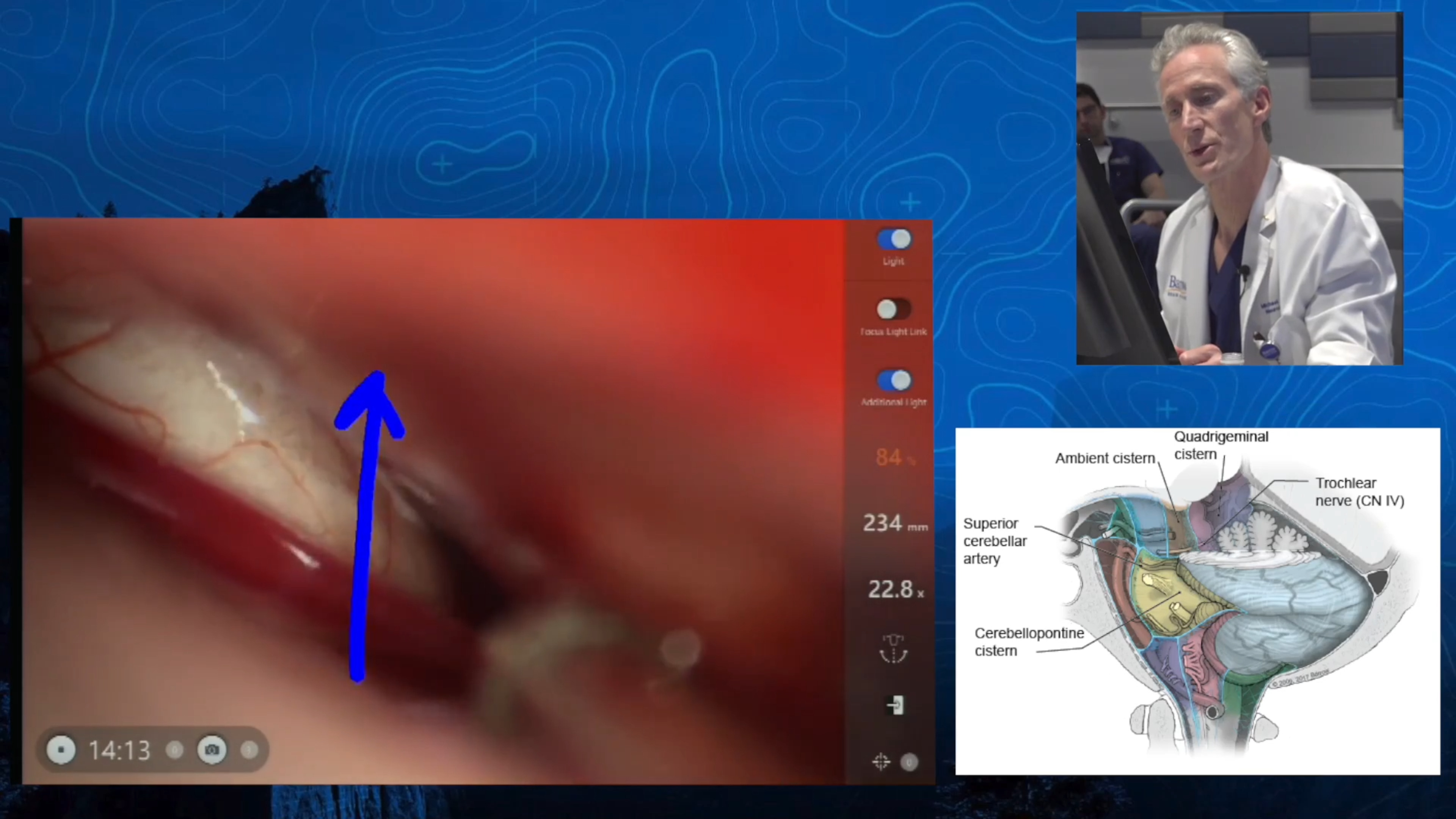
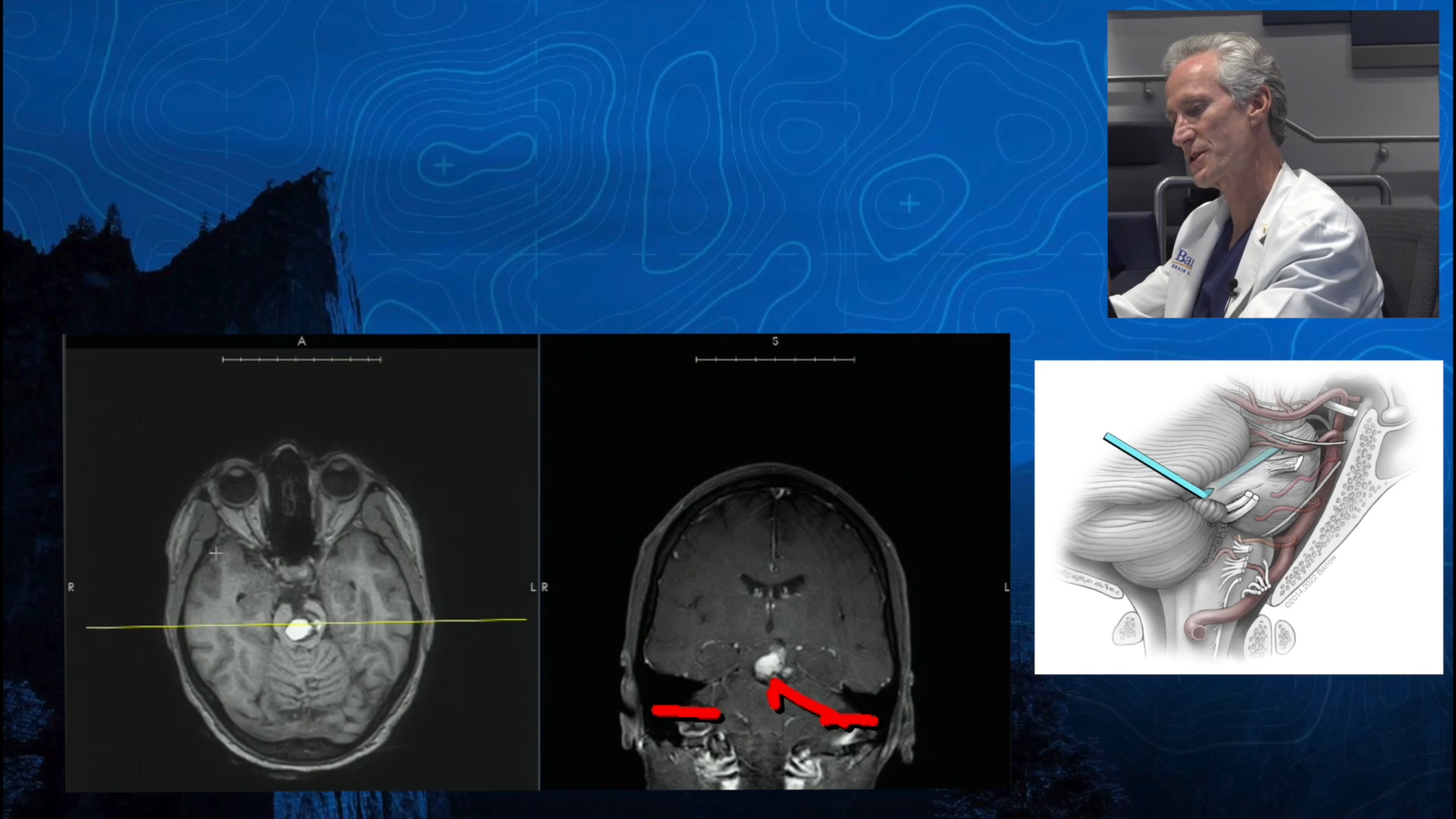
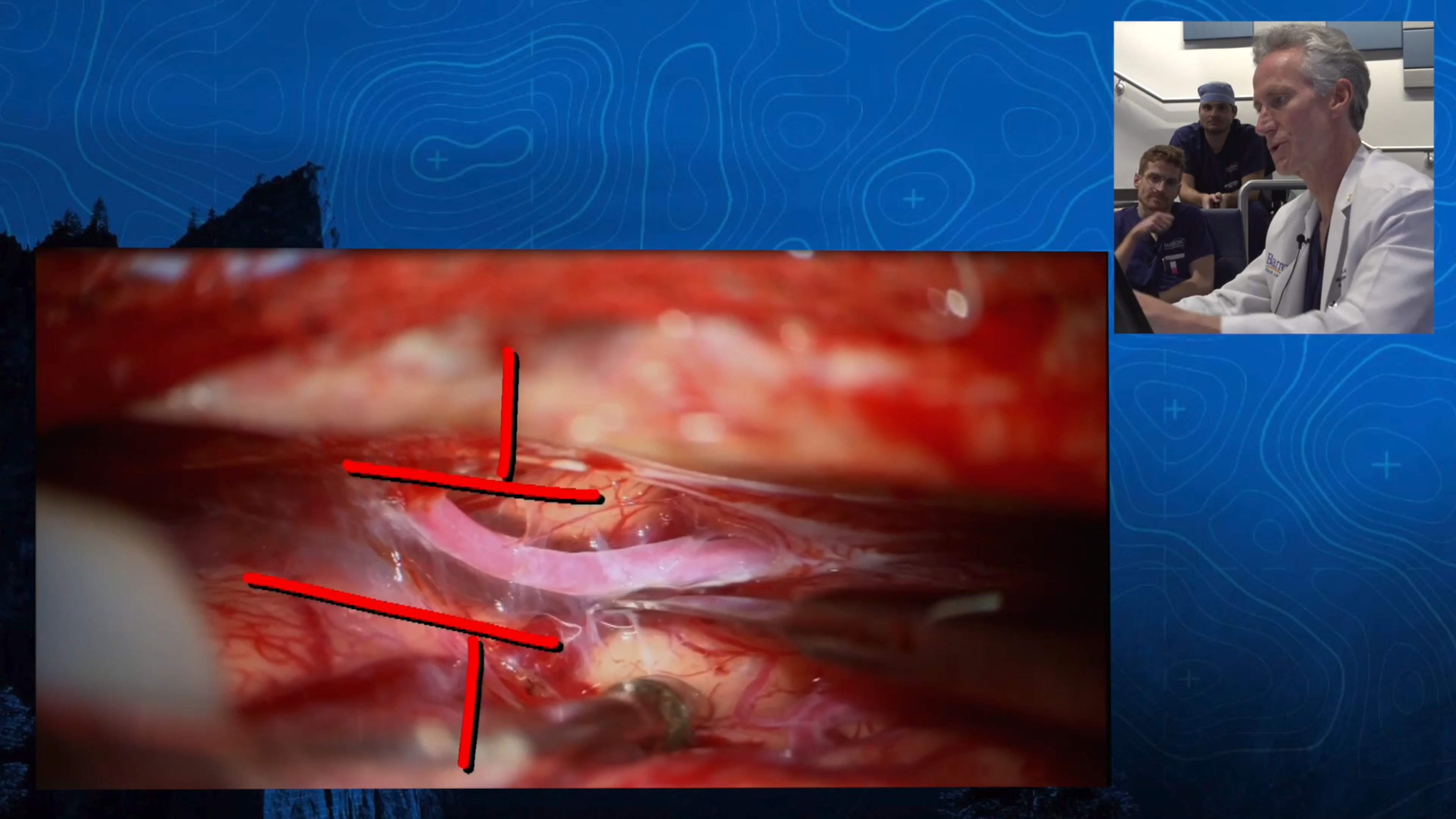
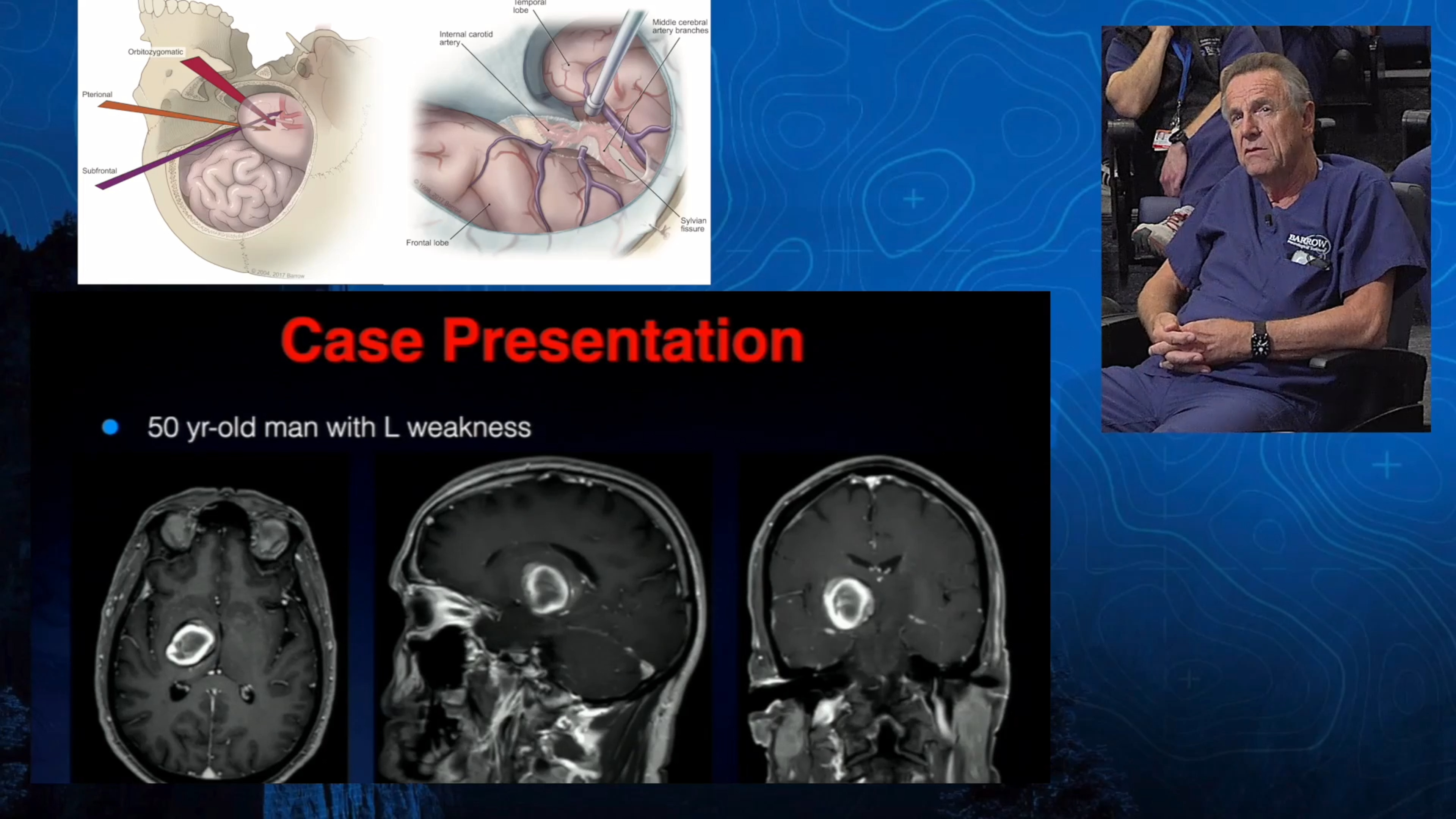
Note: These videos contain surgical footage. Viewer discretion is advised.
References
- Graffeo CS, Scherschinski L, Baranoski JF, Srinivasan VM, Lawton MT. Resection of Quadrigeminal Midbrain Cavernous Malformation Using the Supracollicular Safe Entry Zone. World Neurosurg. 2022 Nov 9;169:51. doi: 10.1016/j.wneu.2022.10.111. Epub ahead of print. PMID: 36334709.
- Catapano JS, Rumalla K, Srinivasan VM, Lawrence PM, Larson Keil K, Lawton MT. A taxonomy for brainstem cavernous malformations: subtypes of pontine lesions. Part 1: basilar, peritrigeminal, and middle peduncular. J Neurosurg. 2022 Mar 25:1-15. doi: 10.3171/2022.1.JNS212690. Epub ahead of print. PMID: 35334459.
- Catapano JS, Rutledge C, Rumalla K, Raygor KP, Srinivasan VM, Koester SW, Kimata AR, Ma KL, Labib MA, Spetzler RF, Lawton MT. External validation of the Lawton brainstem cavernous malformation grading system in a cohort of 277 microsurgical patients. J Neurosurg. 2021 Oct 1:1-9. doi: 10.3171/2021.3.JNS204291. Epub ahead of print. PMID: 34598133.
- Lawton MT, Lang MJ. The future of open vascular neurosurgery: perspectives on cavernous malformations, AVMs, and bypasses for complex aneurysms. J Neurosurg. 2019 May 1;130(5):1409-1425. doi: 10.3171/2019.1.JNS182156. PMID: 31042667.
- Walcott BP, Choudhri O, Lawton MT. Brainstem cavernous malformations: Natural history versus surgical management. J Clin Neurosci. 2016 Oct;32:164-5. doi: 10.1016/j.jocn.2016.03.021. Epub 2016 Jun 16. PMID: 27320373; PMCID: PMC5011020.
- Davies JM, Kim H, Lawton MT. Surgical treatment of cerebral cavernous malformations. J Neurosurg Sci. 2015 Sep;59(3):255-70. Epub 2015 Apr 17. PMID: 25881653.