Neuro-Rehabilitation Robotics & Technology
Overview
After an injury to the brain or spinal cord, your body begins a complex process of healing, adapting, and rewiring.
Although neurons aren’t regenerated the same way that skin or bone is, the brain and spine can reorganize and form new connections to work around an injury, a process known as neuroplasticity. Neuro-rehabilitation can enhance these changes by tapping into the power of neuroplasticity—your body’s ability to form and update the connections between neurons.
As a global leader in the use of robotics for neuro-rehabilitation, highly ranked by U.S. News and World Report, our Neuro-Rehabilitation Center can bolster your recovery and help you return to activities with a level of function and independence you didn’t know was possible. We’re able to measure, support, and challenge your abilities with robotics and technologies that complement conventional therapy to get the most out of your experience as you move through the entire neuro-rehabilitation continuum.
Robotics and Technology in the Neuro-Rehabilitation Continuum
From the earliest stages of recovery in the hospital to after you return home, robotics and technology play an essential role in neuro-rehabilitation.
- In the hospital, robotic devices can help patients begin moving safely—sometimes even within days of an injury or surgery—helping to prevent complications and stimulate the nervous system’s natural healing.
- During inpatient neuro-rehabilitation, robotic walking systems, upper-limb devices, and virtual reality programs allow patients to practice movement and balance with precision and repetition that speed recovery and build confidence.
- In outpatient neuro-rehabilitation, these technologies continue to track progress and challenge patients as they regain strength and independence.
- After you return home, wearable sensors, tele-rehabilitation platforms, and mobile apps can help you stay active and connected to your care teams and support networks.
Across the entire continuum of care, robotics and technology empower patients to engage more fully in their recovery and help therapists deliver highly personalized, effective treatment. Keep scrolling to learn about some of the tools and technologies available to our patients.
AlterG Anti-Gravity Treadmill
The AlterG® is a revolutionary treadmill that uses differential air pressure technology—originally developed by NASA—to reduce a user’s effective body weight while walking or running. Patients wear specialized shorts that zip into a pressurized chamber, which lifts the lower body and decreases the impact on joints.
This technology allows for low-impact neuro-rehabilitation after injuries or surgeries and safe early mobility for patients with neurological conditions. Therapists and trainers also use it for injury prevention and athletic performance training. It is a versatile tool for restoring strength, confidence, and mobility in a controlled environment.

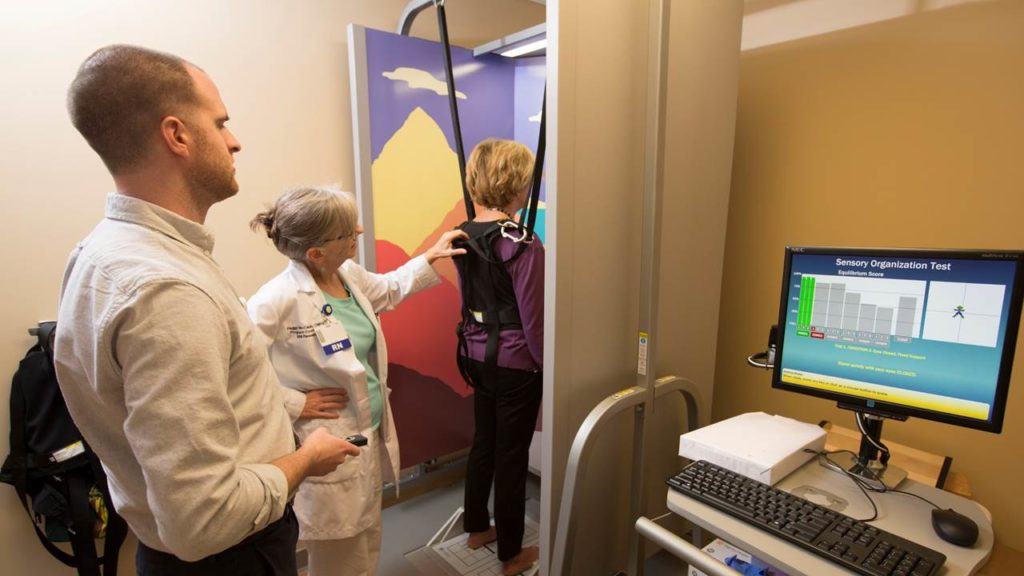
Bertec Computerized Dynamic Posturography (CDP)
The Bertec Computerized Dynamic Posturography (CDP) system combines a dual-balance force plate with immersive virtual reality to assess and treat balance, dizziness, and motion sensitivity problems.
By altering the visual environment and support surfaces, CDP evaluates how your eyes, inner ear, and body work together to maintain stability. This data helps clinicians identify the sensory impairments contributing to your balance difficulties.
CDP also provides engaging rehabilitation by immersing patients in virtual training environments. This type of therapy increases motivation, adaptability, and variability, all of which play an important role in recovery. With customized training protocols, the Bertec system delivers targeted therapy that helps patients regain confidence and independence in daily movement.

Bioness Integrated Therapy System (BITS)
The Bioness Integrated Therapy System (BITS) is an interactive touchscreen technology used in neuro-rehabilitation to assess and improve visual, cognitive, motor, and balance abilities in patients with neurologic conditions. Through engaging games and standardized assessments, BITS helps patients enhance hand-eye coordination, reaction time, memory, and overall brain function, while providing therapists with quantitative data to track progress and improve outcomes.
The system addresses a wide range of issues, including motor retraining, visual field deficits, visual scanning problems, and cognitive impairments such as memory and sequencing issues.
Bioness Vector
The Bioness Vector® is a ceiling-mounted dynamic body-weight support system that accelerates neuro-rehabilitation for patients with impaired balance or walking ability. It aids in recovery from conditions such as stroke, traumatic brain injury (TBI), spinal cord injury, brain tumor resection, or limb amputation.
The system combines a supportive harness with a robotic trolley on an overhead rail, allowing therapists to offload a precise percentage of body weight during training. Patients can safely practice walking, strengthening, and balance exercises with a reduced risk of falling. By providing both fall protection and dynamic weight unloading, the Vector enables patients to confidently push their limits, promoting motor learning and functional recovery.

BIONIK Inmotion Arm/Hand
The BIONIK InMotion® Arm/Hand is an advanced neuro-rehabilitation device designed to help restore arm and hand function after a stroke, brain injury, or spinal cord injury. It uses highly repetitive, robot-assisted movements to retrain the brain and muscles, supporting recovery and reducing movement deficits.
During treatment, therapists place the patient’s arm and hand in a comfortable grip attached to a robotic arm. Depending on your needs, the device can provide guidance, assistance, or gentle resistance throughout the exercise. A screen offers interactive therapy activities and real-time feedback, creating an engaging and motivating therapy experience.
The InMotion Arm/Handcontinuously adapts to the patient’s abilities, ensuring that every session is challenging and effective. Therapy targets include improving range of motion, coordination, strength, smoothness, and movement speed. The system helps maximize recovery potential and accelerate rehabilitation outcomes by tailoring each movement to the patient’s progress.

C-Mill by Motek
The C-Mill by Motek is a cutting-edge rehabilitation treadmill designed to restore gait and balance in patients recovering from neurological conditions, joint replacement, or chronic pain. Equipped with a body-weight support harness, handrails, and advanced visual feedback, the C-Mill creates immersive training environments using augmented and virtual reality.
This system allows patients to practice walking in real-world scenarios, such as navigating obstacles, moving through crowds, or performing dual tasks while walking. As patients train, the C-Mill automatically records key gait parameters—including step length, frequency, symmetry, and center of pressure—without needing external markers or sensors.
These detailed measurements provide therapists with an in-depth analysis of progress over time, helping to tailor rehabilitation programs and maximize recovery outcomes. By combining safety, technology, and real-world practice, the C-Mill supports patients in regaining independence and confidence in their mobility.

Ekso Indego Exoskeleton
The Ekso Indego® is a lightweight, powered hip-knee exoskeleton designed to support gait training and mobility in individuals with walking impairments. This modular device extends from the waist to the feet, with motorized joints at the hips and knees controlled by a central unit at the belt.
The Ekso Indego is available in two versions:
- Ekso Indego Therapy: Designed for clinical rehabilitation settings, this version allows therapists to guide patients through gait training sessions with customizable assistance and progression.
- Ekso Indego Personal: This exoskeleton, created for community and home use, allows individuals with mobility challenges to walk independently outside the clinic.
Both versions feature intuitive, posture-based controls, where leaning forward initiates walking, and motors and sensors respond to the user’s natural movements. At the same time, your therapist can adjust assistance levels wirelessly to transition from full robotic support to partial assistance as recovery progresses. Many patients are able to stand and walk during their very first session with the device.
The Barrow Neuro-Rehabilitation Center is the only facility in Arizona with specialists certified in the clinical and personal-use of the Ekso Indego.
EksoNR
The Ekso Bionics EksoNR is a cutting-edge robotic exoskeleton designed to help patients recover from lower extremity weakness or paralysis caused by spinal cord injury, stroke, traumatic brain injury (TBI), or neurological conditions such as multiple sclerosis (MS) and Guillain-Barré syndrome.
This wearable device fits securely around the torso and legs, with padded straps and motorized joints at the hips and knees. Once in place, the EksoNR allows patients to stand and walk, even when they cannot move their legs independently. Its intelligent software and sensors provide adaptive assistance, adjusting in real time to each step and offering a more natural gait and postural support.
As patients build strength and coordination, the therapist can customize the settings on the device, encouraging patients to use their muscles and optimizing their progression by
tailoring each therapy session to the patient’s unique needs and progress.
By delivering consistent, high-quality repetitions of standing and walking, the EksoNR helps retrain the brain and muscles to restore proper movement patterns. This early mobility accelerates physical recovery and profoundly impacts emotional well-being, boosting confidence, motivation, and hope.
Barrow Neurological Institute is proud to be an Ekso Bionics Center of Excellence. In this role, we rigorously test new technology, advance research, and help expand access to the most effective robotic rehabilitation tools.
Note: EksoNR is not approved for home use at this time.

Fourier Rehab ArmMotus M2 Pro
The Fourier ArmMotus™ M2 Pro is an advanced robotic rehabilitation system for treating upper limb movement impairments caused by neurological or musculoskeletal conditions. This innovative device combines intelligent robotics with an immersive, game-like therapy experience to help patients regain motor control and functional ability in the shoulder and elbow joints.
The ArmMotus M2 Pro uses real-time force feedback and haptic technology, allowing patients to see their progress and “feel” their interaction with therapy activities. The system supports multiple training modes—passive, assistive, active, and resistive—so therapists can incorporate the patient’s current abilities and recovery stage.
Therapists receive detailed performance reports, enabling them to create personalized training programs that match each patient’s physical and cognitive needs. The engaging therapy games and goal-directed tasks motivate patients to complete the high number of repetitions needed for recovery, while keeping therapy both effective and enjoyable.

Harmony SHR
Harmony SHR® is a robotic device that helps people regain movement in their arms and shoulders after an injury or illness, such as a stroke, brain injury, or specific muscle and joint conditions. Designed to move the way your body does naturally, it gives patients safe, effective therapy while providing therapists with clear feedback on progress.
The shoulder is a complex joint that recruits the muscles and joints of the shoulder blade (scapula) to move. Harmony copies the natural teamwork between these units, so exercises feel smoother, safer, and closer to everyday movement. Supporting most of the shoulder’s natural range of motion, it helps patients rebuild strength and flexibility while protecting the joint.
The Harmony SHR device allows both arms to work together, recruiting the stronger arm to can guide the weaker one, helping the brain relearn movement patterns. This mirrored motion is a powerful tool in recovery after a stroke or brain injury. Your physical therapist can also adjust the amount of support provided. Harmony can provide full lifting assistance for those who need it, or lighter guidance for those further along in recovery. As you improve, your neuro-rehabilitation team can gradually reduce the help so you supply more of the effort.
Because it takes weight off the shoulder, Harmony makes it possible to start safe movement earlier, even for people with profound weakness. This reduces the risk of complications like shoulder dislocation while encouraging progress from the beginning. It also allows many repetitions of everyday arm and shoulder motions, which are key to retraining the body. Built-in sensors track range of motion, strength, and repetition counts, giving therapists precise information to adjust therapy and mark recovery milestones.

Myomo MyoPro Arm Orthosis
The Myomo MyoPro® is a powered arm brace that helps regain arm and hand function in people with partial paralysis or weakness due to conditions such as stroke, spinal cord injury, traumatic brain injury, brain tumor, amyotrophic lateral sclerosis, multiple sclerosis, and other neurological disorders and injuries.
This wearable device fits over the arm and hand, with lightweight frame components that strap around the upper and lower arm. A computer controls small motors at the elbow, while electrodes inside the brace detect even the faintest muscle signals from the skin. When a person attempts to move—such as reaching for an object or bringing food to the mouth—the device amplifies those weak signals to assist the movement.
Because the MyoPro continuously monitors and responds to muscle activity, it can be used for rehabilitation in clinical settings or daily functional support at home, helping patients regain independence in everyday tasks.
The Neuro Sensory Motor Integrator (NSMI)
The Neuro Sensory Motor Integrator (NSMI) is a therapeutic system that helps neuro-rehabilitation patients improve their brain’s ability to process sensory information and translate it into appropriate motor responses. It uses an interactive touchscreen to deliver individualized therapies that enhance visual tracking, eye-hand coordination, balance, and other cognitive and motor skills. The NSMI creates customized treatment plans to address issues stemming from strokes, brain injuries, and balance disorders, ultimately improving their coordination, function, and overall quality of life.
At its core, the system works by improving sensorimotor integration, the process by which the nervous system combines sensory input (sight, touch, balance) with motor output to create coordinated movement. A large, interactive touchscreen presents a variety of therapy procedures, such as eye-hand coordination exercises, saccadic eye movements, and vestibular balance training. It can also assist in improving cognitive abilities, including divided attention, visual search, and visual memory.
Olympus Digital Swallowing Station (DSS)
The Olympus Digital Swallowing Station (DSS) is an advanced imaging system that helps diagnose and monitor swallowing disorders (dysphagia). Swallowing difficulties may occur after head and neck cancer, brain injury, neurological disease, or surgical complications. They can significantly impact health and quality of life.
At Barrow, speech-language pathologists (SLPs)—specialists in swallowing disorders—use DSS to perform fiber optic endoscopic evaluation of swallowing (FEES). This minimally invasive procedure involves gently passing a flexible endoscope through the nasal passage to provide a magnified, real-time view of the throat during swallowing. Patients receive foods and liquids of varying consistencies, mixed with food coloring for visibility, so the SLP can directly observe how the muscles and structures of the throat are functioning.
FEES provides an early and accurate diagnosis by identifying underlying physiological deficits. It helps reduce the risk of aspiration pneumonia, guides safe diet advancement, and allows SLPs to create individualized therapy programs. By tailoring swallowing exercises and dietary recommendations, this technology plays a critical role in restoring safety and independence for patients with dysphagia.
ProtoKinetics Zeno Walkway
The ProtoKinetics Zeno Walkway™ is a pressure-sensitive mat that provides detailed, quantitative data on gait and balance. Thousands of embedded sensors capture measurements such as walking speed, stride length, stance time, and center of pressure, which are then analyzed using PKMAS software.
This system supports clinicians in:
- Diagnosing gait abnormalities and movement disorders
- Monitoring progress and measuring the effectiveness of therapy
- Comparing performance with different assistive devices
- Providing patients with objective feedback to encourage engagement and adherence
Portable and precise, the Zeno Walkway enhances clinical care and research by making gait and balance assessment a measurable, trackable process.

RAPAEL Smart Glove
The RAPAEL Smart Glove combines wearable technology with interactive, game-like therapy to improve hand, wrist, fingers, and forearm movement following a stroke, brain injury, or spinal cord injury.
This lightweight, flexible glove straps around the hand and wrist and uses built-in stretch sensors to detect minute active movements. Patients interact with engaging virtual reality exercises that simulate real-life tasks, such as gripping, lifting, or rotating the wrist. As the glove translates each motion into the therapy program, patients receive real-time feedback to guide and motivate their progress.
The RAPAEL Smart Glove also tracks performance over time, allowing therapists and patients to see measurable improvements. Its interactive design encourages high-repetition, task-specific training, making therapy more enjoyable while promoting long-term recovery.

Restorative Therapies RT300
The RT300® system by Restorative Therapies combines functional electrical stimulation (FES) with motor-assisted cycling for the arms, legs, or core. By stimulating peripheral nerves, RT300 activates muscles and supports repetitive movement patterns. This therapy helps prevent muscle atrophy, manage spasticity, improve circulation, and restore function for individuals with paralysis or weakness.
Integrated biofeedback and data tracking allow therapy to be tailored to each patient’s needs, whether in a clinic or at home.

Restorative Therapies Xcite
The Xcite® system by Restorative Therapies is a multi-channel functional electrical stimulation (FES) device that helps patients regain motor function through task-specific, coordinated movements.
By delivering electrical pulses to motor nerves, Xcite triggers muscle contractions that mimic natural actions like grasping, feeding, and transferring. The system uses wireless technology and guided activities to promote muscle re-education, improve coordination, and increase range of motion.

SMARTfit System
The SMARTfit® system is an interactive rehabilitation platform that blends physical activity with cognitive challenges—a method known as dual-task training. During therapy, patients engage in both movement and problem-solving simultaneously. For example, a game might require striking a target with a ball while solving a math or spelling problem displayed on the screen.
This training enhances neuroplasticity, helping the brain form new pathways that support improvements in memory, concentration, processing speed, and problem-solving. The gamified design makes therapy engaging while providing effective rehabilitation for conditions such as concussion, stroke, and traumatic brain injury.

Synchrony Dysphagia Solutions
The Synchrony Dysphagia System by ACP is an interactive therapy tool designed to help patients relearn how to swallow through biofeedback and electrical stimulation.
Using surface electromyography (sEMG) biofeedback, small electrodes are placed on the neck and cheek to monitor the activity of swallowing muscles. Patients and therapists can then see this muscle activity in real time on a screen, receiving both visual and auditory feedback. This helps patients understand if they are performing exercises correctly and reinforces the use of proper muscle movements.
The Synchrony system combines this feedback with gamified virtual reality exercises to make therapy more engaging and motivating. Its therapeutic approach works by:
- Strengthening muscles of the throat and jaw through sEMG biofeedback and electrical stimulation
- Boosting motivation with interactive, game-like exercises
- Encouraging neuroplasticity by helping the brain re-establish correct muscle patterns
- Providing measurable outcomes with data-driven tracking to refine treatment plans
By blending advanced technology with evidence-based therapy, the Synchrony system enhances recovery for patients with swallowing difficulties, helping them achieve safer, more effective function.
TerrainHopper
The TerrainHopper is a powerful, battery-powered, all-terrain mobility device designed to traverse challenging environments like sand, mud, snow, and steep hills. It is categorized as an other power-driven mobility device (OPDMD). People with mobility impairments use it to access public spaces and outdoor areas, such as parks, beaches, and trails.
It enables people to help resume some activities that their current disability makes difficult due to limitations of their mobility or mobility device. The TerrainHopper provides a means to navigate challenging outdoor environments, restoring access to activities they might otherwise miss. This may include outdoor recreation like hunting, fishing, camping, and beach walks, which can have significant benefits for their physical and mental well-being. It can handle a wide range of difficult surfaces, including deep mud, soft sand, rocky terrain, and steep inclines.

Tyromotion Diego
The Tyromotion DIEGO® is a state-of-the-art robotic system for arm and shoulder rehabilitation. Our physical medicine and neuro-rehabilitation specialists use it to help patients regain motor function after neurological injuries.
DIEGO uses intelligent gravity compensation (IGC) to make arm movements easier and more natural. It works by reducing the effects of gravity so patients can practice functional activities with greater success. The system provides a three-dimensional therapy space, allowing for a wide range of motion and task-oriented exercises that mirror everyday activities.
DIEGO also incorporates virtual reality training modules to enhance motivation. These modules encourage patients to actively participate in therapy while increasing the number of repetitions completed during sessions. Its adaptable design supports both one-armed (unilateral) and two-armed (bilateral) training, making it suitable for patients across all phases of neuro-rehabilitation.
Therapists can tailor the level of support—from fully assisted to actively resisted movement—to meet the needs of each individual, while also customizing software and control settings to ensure patients work at their maximum ability. Importantly, DIEGO can be used with patients of all ages, providing versatile rehabilitation options throughout the recovery journey.
Vestibular Rehabilitation Suite
The vestibular system—the body’s system for maintaining balance and orientation, located in the inner ear—is critical in helping you stay steady and confident in your movements. Disorders of this system may develop after a stroke, concussion, or inner ear condition, leading to dizziness, imbalance, or motion sensitivity.
Our vestibular suite combines advanced diagnostic and treatment tools to restore balance and improve quality of life.
One of the primary systems in our suite is the SMART Balance Master®, which evaluates how well you maintain balance under changing conditions. The system provides real-time feedback about your balance and postural control by adjusting the walls and floor while you complete tasks on a screen. We also use RealEyes™ Video Frenzel goggles, which record and replay eye movements to detect abnormalities that guide individualized treatment planning.
Virtual, Augmented & Mixed Reality
Virtual Reality (VR)
Virtual Reality (VR) creates immersive, computer-generated environments that stimulate multiple senses to enhance rehabilitation. Patients can rebuild strength, coordination, and balance through repetitive, goal-directed tasks. Virtual reality also supports cognitive rehabilitation by simulating daily activities, such as grocery shopping, to strengthen memory and problem-solving skills. In addition, VR can help with pain management by reducing the brain’s perception of chronic pain, and it allows patients to safely practice real-world scenarios like crossing a busy street.
Augmented Reality (AR)
Augmented Reality (AR) layers digital elements over the real world to create immersive and personalized therapy experiences. Patients can practice tasks that improve motor skills, gait, posture, and cognitive function, while clinicians benefit from enhanced diagnostic support. For patients with conditions like Parkinson’s disease, AR-based dual-task training can strengthen balance and movement.

Mixed Reality (MR)
Mixed Reality (MR) merges real and virtual environments, enabling patients to interact with digital elements while remaining aware of their physical surroundings. This approach provides safe, immersive training for conditions such as stroke, traumatic brain injury, and Parkinson’s disease. Mixed reality offers real-time feedback, customizable therapy environments, and detailed performance data, allowing your team to track your progress and guide your treatment.

ZeroG by Aretech
The ZeroG® by Aretech is an advanced robotic system designed to improve walking, balance, and functional mobility in patients with neurological deficits. This innovative technology provides dynamic body-weight support in a controlled, reduced gravity environment, allowing patients to safely practice walking, standing, and other everyday activities without the risk of falling.
The system uses an overhead track and trolley that moves with the patient, continuously monitoring and responding to their movements. ZeroG prevents falls and enables therapists to safely introduce challenges such as TRiP perturbations, sit-to-stand training, and floor transfers. By removing the danger of falling, patients can attempt more demanding activities earlier in their recovery.
Therapists can tailor each session by adjusting fall protection settings and robotic assistance levels, either facilitating or resisting walking movements depending on the patient’s needs. This safe, high-intensity practice helps promote neuroplasticity—the brain’s ability to rewire itself—supporting the restoration of motor function and independence.